Pediatric Radiology — MCQs

On this page
In a newborn, what is the typical time frame for gas to reach the colonic end?
A child presents with multiple vertebral anomalies and a posterior mediastinal mass. What is the likely diagnosis?
Antenatal ultrasound demonstrating a double bubble appearance is typically indicative of which of the following conditions?
What is the characteristic radiological sign observed in Croup?
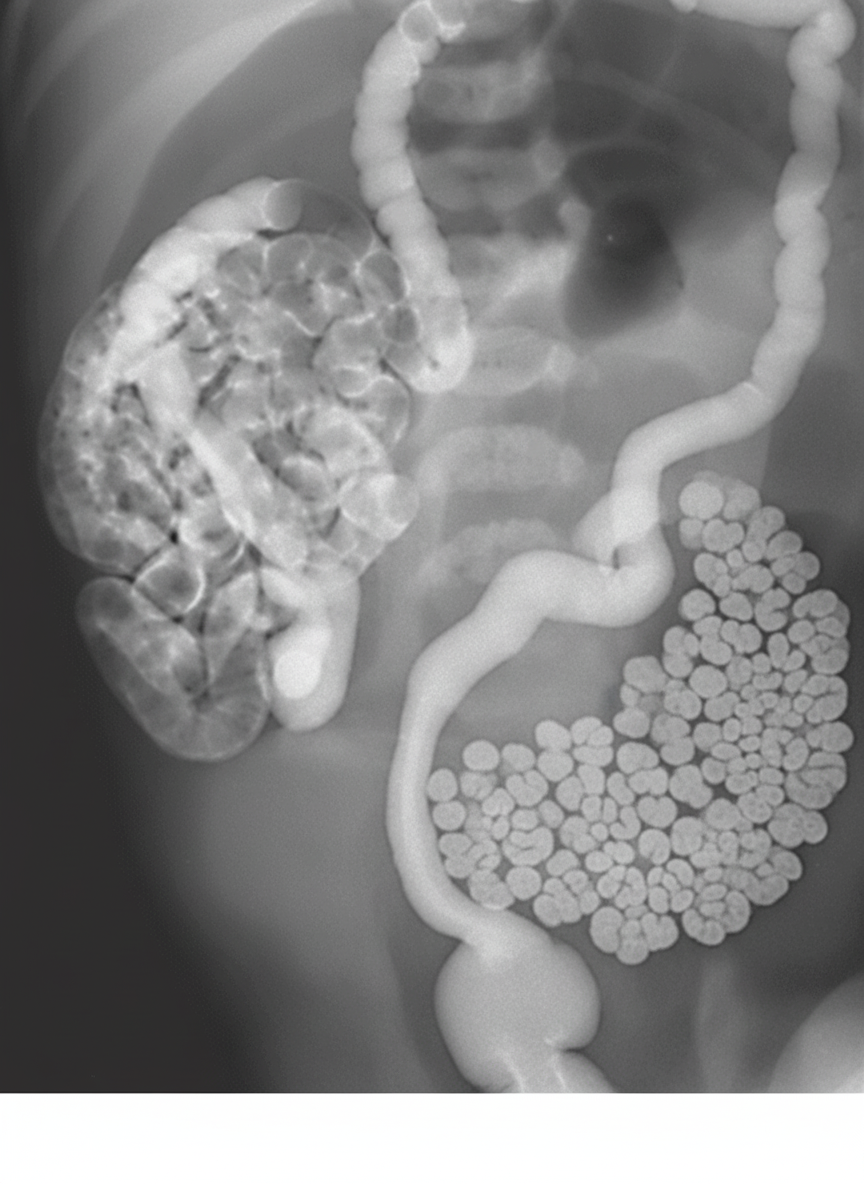
A contrast enema is performed on a one-day-old infant presenting with bilious emesis and abdominal distension. Based on the findings, which of the following is the MOST likely diagnosis?
What is the most common cause of a mass in the posterior mediastinum in children?
Regarding neuroimaging in the neonatal period, all are true except?
What is the name of the study performed on a newborn with an inability to pass stools, often visualized in an X-ray?
A preterm baby suffered perinatal asphyxia and was found to have Periventricular leucomalacia on CNS imaging. Which imaging modality was used?
What is the most characteristic radiographic sign in a child with leukemia?
Practice by Chapter
Normal Pediatric Developmental Anatomy
Practice Questions
Neonatal Imaging
Practice Questions
Pediatric Chest Imaging
Practice Questions
Pediatric Abdominal Imaging
Practice Questions
Pediatric Musculoskeletal Imaging
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital Heart Disease Imaging
Practice Questions
Pediatric Oncology Imaging
Practice Questions
Child Abuse Imaging
Practice Questions
Pediatric Interventional Radiology
Practice Questions
Radiation Protection in Pediatrics
Practice Questions
Sedation in Pediatric Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
