Pediatric Radiology — MCQs

On this page
The "triangular cord sign" on ultrasonography is indicative of which condition in a neonate?
A neonate presented on day one of life with bilious vomiting. What is the first investigation to be done?
The lung-head ratio is useful in the diagnosis of which of the following conditions?
Given the provided X-ray of a neonate, what is the diagnosis?
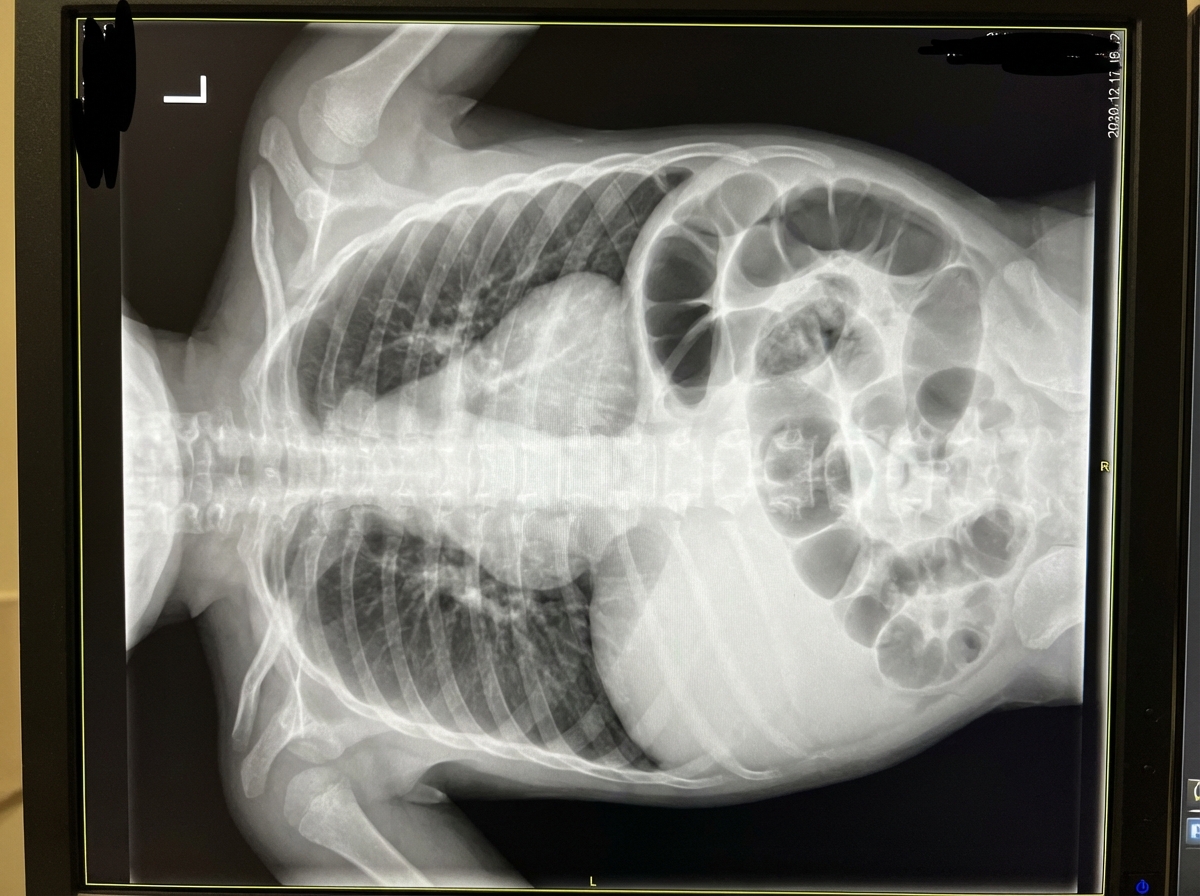
Wimberger's ring is seen in:
A premature infant born at 34 weeks presented with acute onset lethargy and cessation of feeding. What is the imaging modality of choice to screen for intraventricular haemorrhage?
An invertogram is typically taken after how many hours of birth?
Congenital hypertrophic pyloric stenosis is diagnosed by which imaging modality?
Time sector imaging is preferred in infants because:
The diagnostic feature of congenital diaphragmatic hernia on prenatal ultrasonography is:
Practice by Chapter
Normal Pediatric Developmental Anatomy
Practice Questions
Neonatal Imaging
Practice Questions
Pediatric Chest Imaging
Practice Questions
Pediatric Abdominal Imaging
Practice Questions
Pediatric Musculoskeletal Imaging
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital Heart Disease Imaging
Practice Questions
Pediatric Oncology Imaging
Practice Questions
Child Abuse Imaging
Practice Questions
Pediatric Interventional Radiology
Practice Questions
Radiation Protection in Pediatrics
Practice Questions
Sedation in Pediatric Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
