Nuclear Medicine — MCQs

On this page
All of the following are beta emitting particles except?
Radionuclide scans are useful in all of the following except:
What is the test for reversible cardiac ischemia?
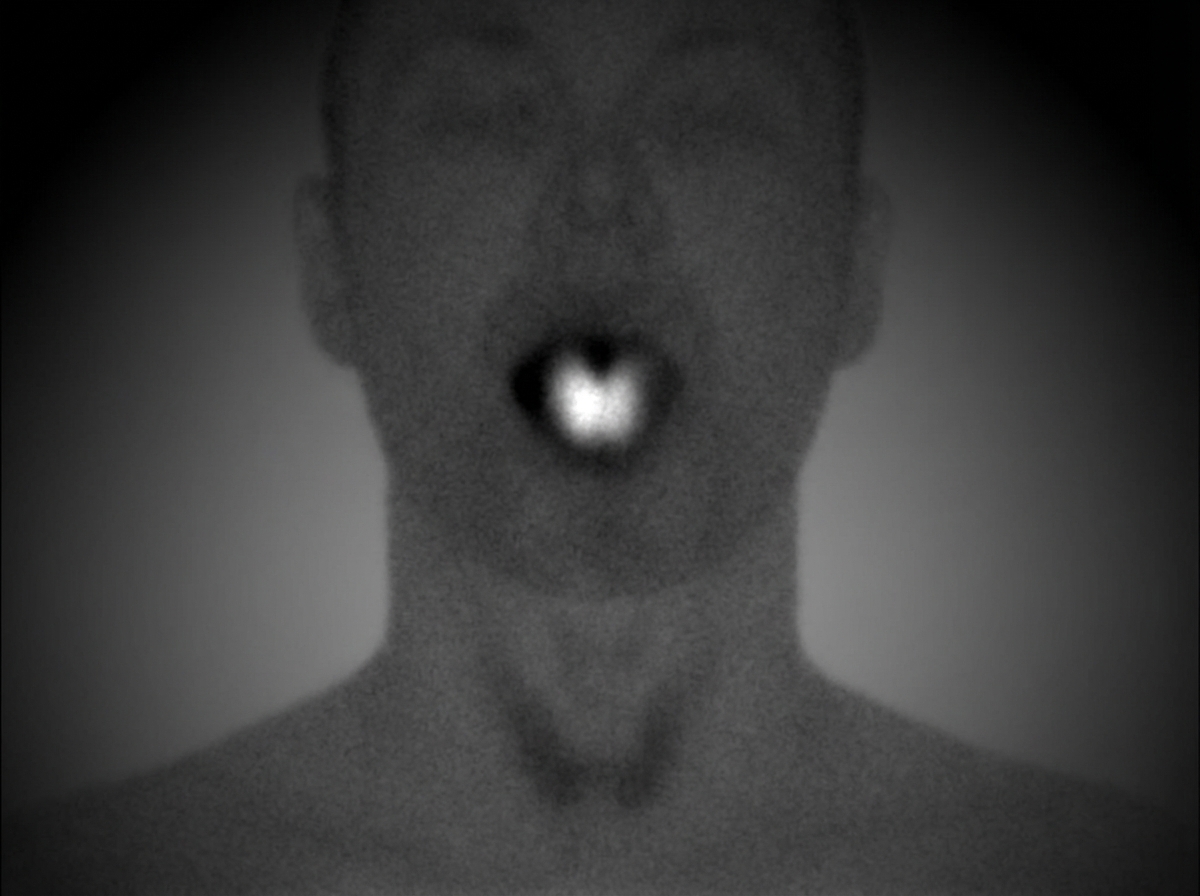
Following RAIU studies demonstrate which of the following conditions?
What dye is used in SPECT?
What is the half-life of Iodine-123?
What is the best imaging modality for neuroendocrine tumors?
A HIDA scan is useful in which of the following conditions?
In the diagnosis of acute myocardial infarction, a hot spot is seen with which imaging modality?
Which iodine isotope is used for the treatment of carcinoma of the thyroid?
Practice by Chapter
Physics of Nuclear Medicine
Practice Questions
Radiopharmaceuticals
Practice Questions
Radiation Detection in Nuclear Medicine
Practice Questions
Thyroid Scintigraphy
Practice Questions
Bone Scintigraphy
Practice Questions
Renal Nuclear Medicine
Practice Questions
Cardiac Nuclear Medicine
Practice Questions
Pulmonary Nuclear Medicine
Practice Questions
Neurological Nuclear Medicine
Practice Questions
PET/CT Principles and Applications
Practice Questions
Radionuclide Therapy
Practice Questions
Radiation Safety in Nuclear Medicine
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
