Cardiac Nuclear Medicine — MCQs

Cardiotoxicity caused by radiotherapy & chemotherapy is best detected by
MUGA scan is not useful in:
Hot spot in heart is seen in which scan
In the condition shown below, rib notching is present in which of the following ribs? (AIIMS Nov 2015)
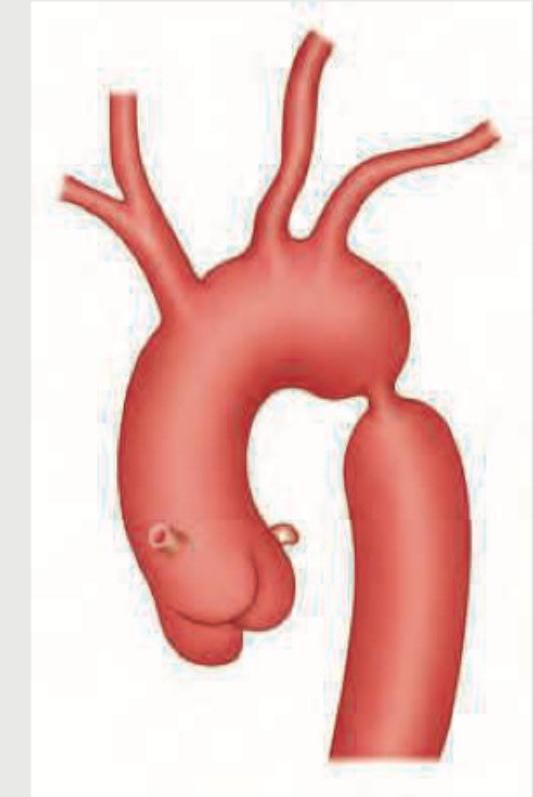
Which artificial radioisotopes are used in nuclear medicine?
Increased radio-isotope uptake is seen in which of the following conditions?
Which of the following isotopes is radioactive?
Precautions advised after outpatient Radioiodine (I-131) therapy are all, EXCEPT:
Which of the following is a functional investigation?
Which of the following is the best method for measuring renal Glomerular Filtration Rate (GFR)?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
