Spine Imaging: Trauma and Degenerative Disease — MCQs

What is the investigation of choice for diagnosing a stress fracture?
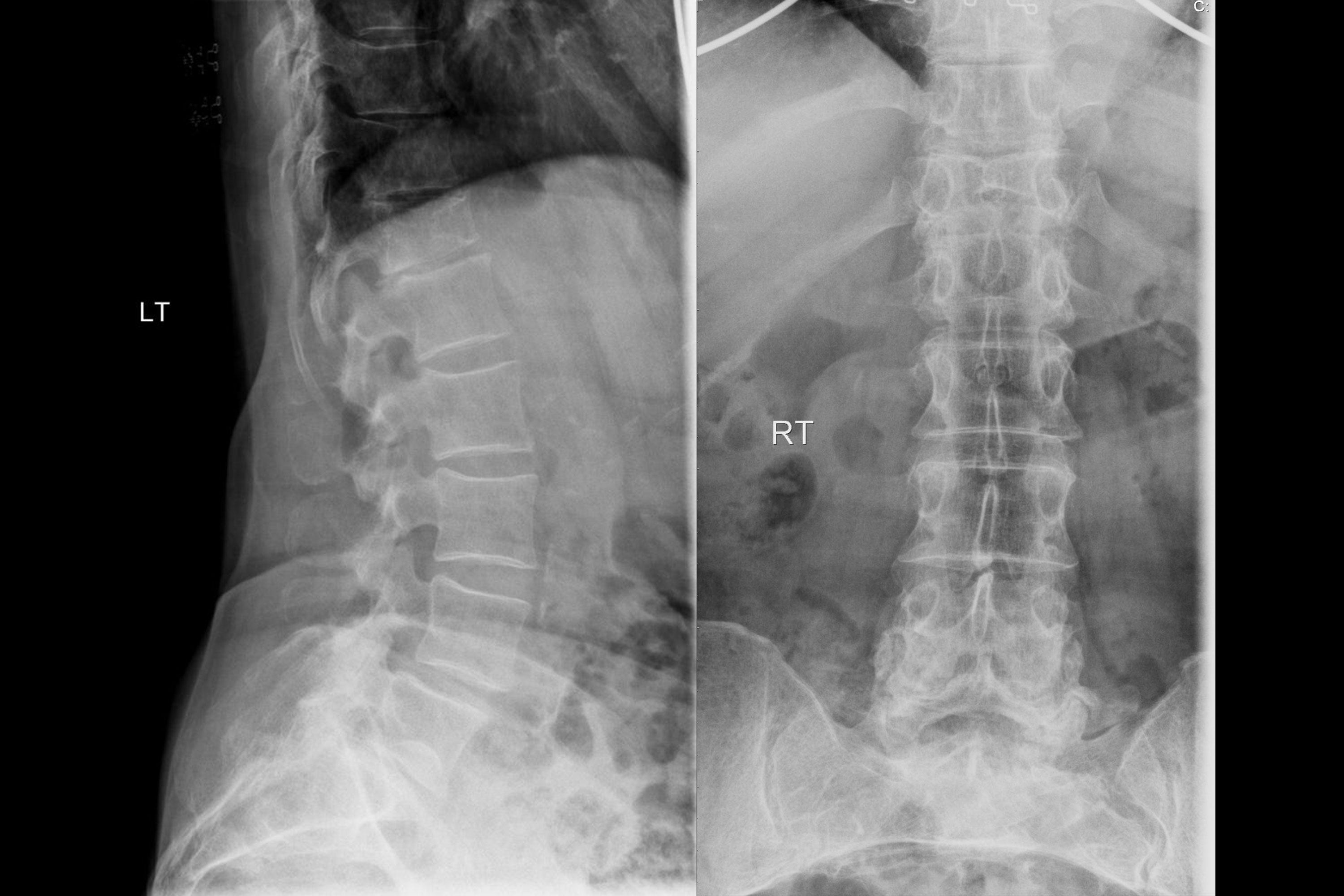
A 75-year-old female has chronic backache. X-ray of the spine is shown. What is the most likely diagnosis?
What is the investigation of choice in a patient with traumatic paraplegia?
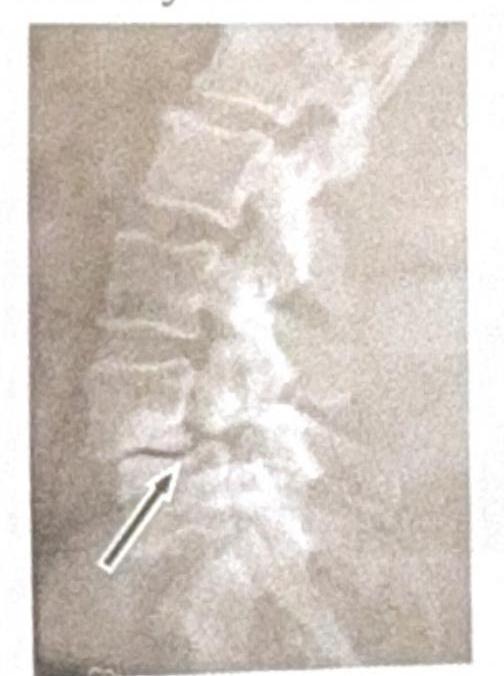
Identify the condition shown in the image:
After chronic use of steroids severe pain in right hip with immobility is due to
Spine MRI shows 'pencil-sharpened' vertebral bodies and 'H-shaped' vertebrae on T1-weighted images. Most likely diagnosis?
A patient with a history of chronic ear infection now presents with manifestations, including headache and vomiting. A CT brain image is shown. What is the most probable diagnosis?

Time of Flight technique is employed in —
What is the primary imaging modality used for diagnosing urethral trauma?
A patient presents with a suspected cervical spine injury following an accident. What is the first step in management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
