Neuroradiology — MCQs

On this page
Identify the condition shown in the CT scan image.
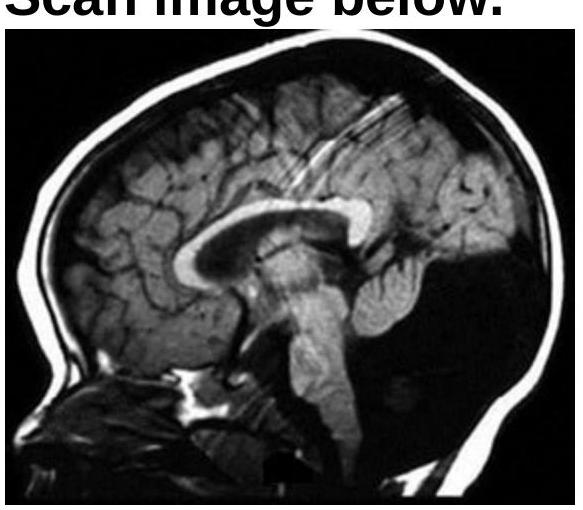
Which of the following abnormalities is most commonly detected as a vascular malformation on skull MRI?
Investigation of choice for acute intracerebral hemorrhage is -
On imaging, diffuse axonal injury is characterized by -
Which imaging modality is most effective in differentiating between epidermoid cyst and arachnoid cyst?
What is the CT scan finding in a carotid cavernous sinus fistula?
Which condition is characterized by a specific radiological appearance resembling a sunburst pattern?
What are the X-ray findings associated with chronic otitis media?
All the following are true of craniopharyngioma except:
Investigation of choice for intramedullary SOL is -
Practice by Chapter
Neuroanatomy for Radiologists
Practice Questions
Cerebrovascular Diseases
Practice Questions
Intracranial Tumors
Practice Questions
CNS Infections
Practice Questions
Demyelinating and Degenerative Diseases
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Imaging: Trauma and Degenerative Disease
Practice Questions
Spine Tumors and Infections
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital CNS Anomalies
Practice Questions
Functional Neuroimaging
Practice Questions
Neurointerventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
