Neuroradiology — MCQs

On this page
Which of the following is NOT a typical radiological finding in meningioma?
Lytic "punched-out" or "beaten-metal" lesions are seen in a skull X-ray, the most likely cause is:
CT findings in Epidural Hematoma (EDH) are typically described as?
Upstream and downstream hydrocephalus is seen in which of the following conditions?
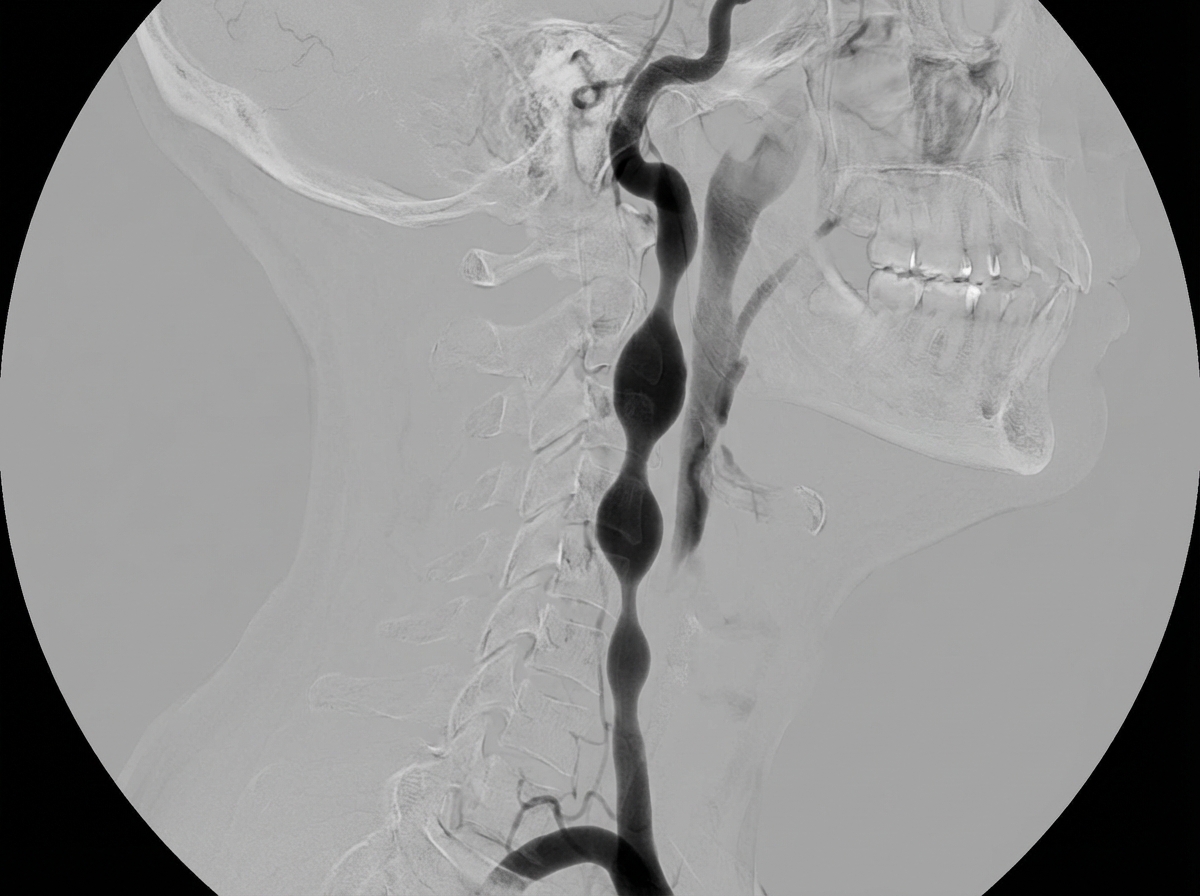
A 35-year-old female presented with a history of multiple transient ischemic attacks. What is the most likely diagnosis suggested by the given carotid angiogram?
What are the characteristic imaging findings in Alzheimer's disease?
What condition presents with a hyperdense biconvex appearance on a cranial CT scan?
Which of the following conditions is characterized by bracket calcification?
What are the characteristic features of tubercular meningitis on MR imaging?
A 10-year-old male patient presents with a 20-day history of headache and vomiting. Examination reveals an ataxic gait. NCCT shows a fourth ventricular mass causing obstructive hydrocephalus. CE-MRI is performed to characterize the lesion. What is the most probable diagnosis?
Practice by Chapter
Neuroanatomy for Radiologists
Practice Questions
Cerebrovascular Diseases
Practice Questions
Intracranial Tumors
Practice Questions
CNS Infections
Practice Questions
Demyelinating and Degenerative Diseases
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Imaging: Trauma and Degenerative Disease
Practice Questions
Spine Tumors and Infections
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital CNS Anomalies
Practice Questions
Functional Neuroimaging
Practice Questions
Neurointerventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
