Neuroradiology — MCQs

On this page
A 55 year old male came with history of hoarseness of voice for which direct laryngoscopy was done and the lesion was biopsied to detect squamous cell carcinoma. He now requires investigation to detect extent of cartilage involvement, imaging of pre and paraglottic spaces and any extension to deep neck structures. Most appropriate investigation of choice will be:
Indications of computed tomography after head injury include all EXCEPT:
The term mid-line shift is associated with:
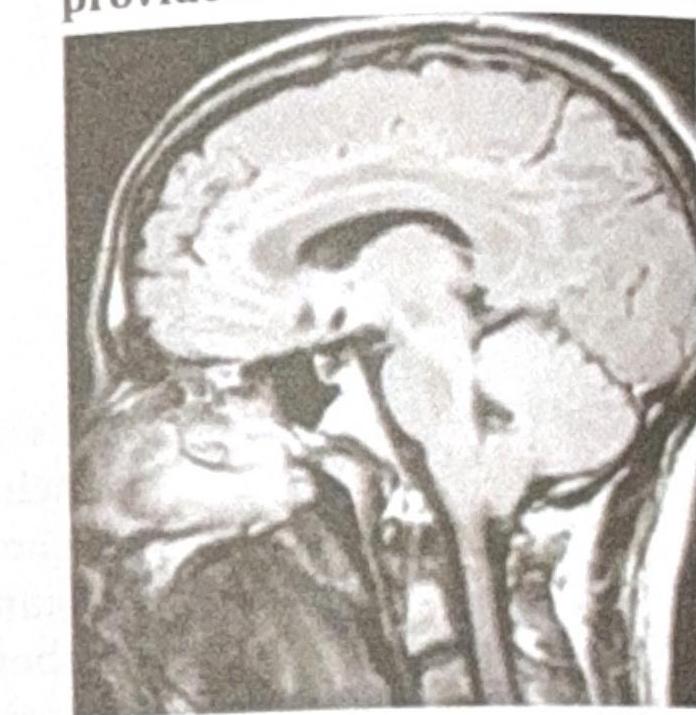
Identify the diagnosis using the MRI provided.
A 40-year-old male presents with a history of headaches, fever, and new-onset seizures. An MRI of the brain is performed, revealing a ring-enhancing lesion with central restricted diffusion on diffusion-weighted imaging (DWI). What is the most likely diagnosis?
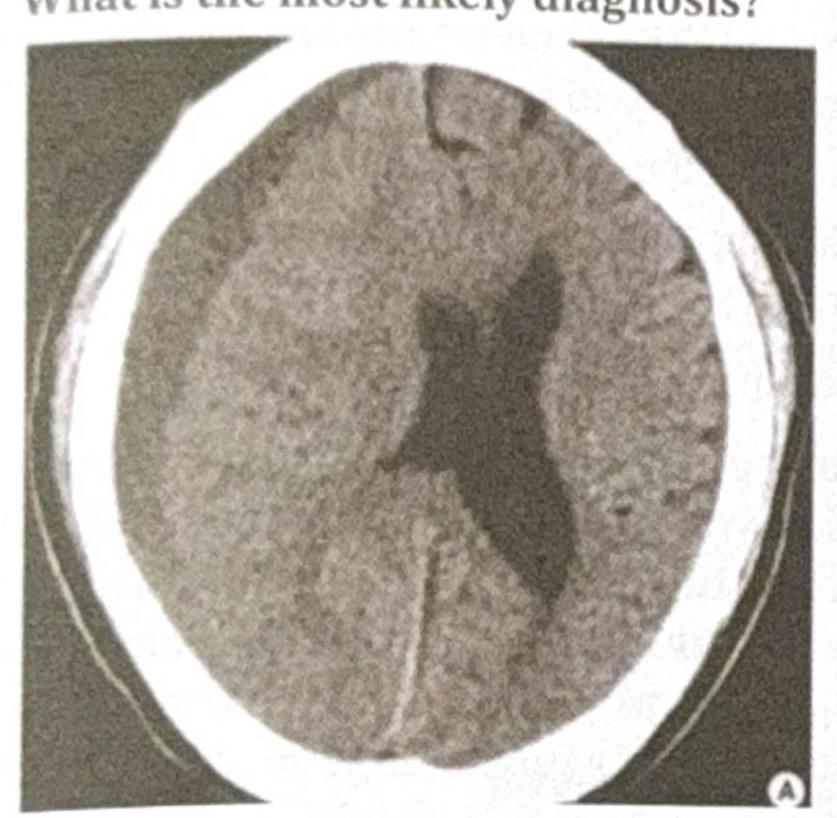
An 80-year-old male with a history of frequent falls presents with progressive headache, confusion, and mild hemiparesis over the past few weeks. A CT scan of the head is performed, and the image provided shows a crescent-shaped, hypodense collection over the left cerebral hemisphere with a slight midline shift. What is the most likely diagnosis?
A patient presents with ear discharge. The CT image is shown below. Based on the clinical presentation and imaging, what is the most likely diagnosis?
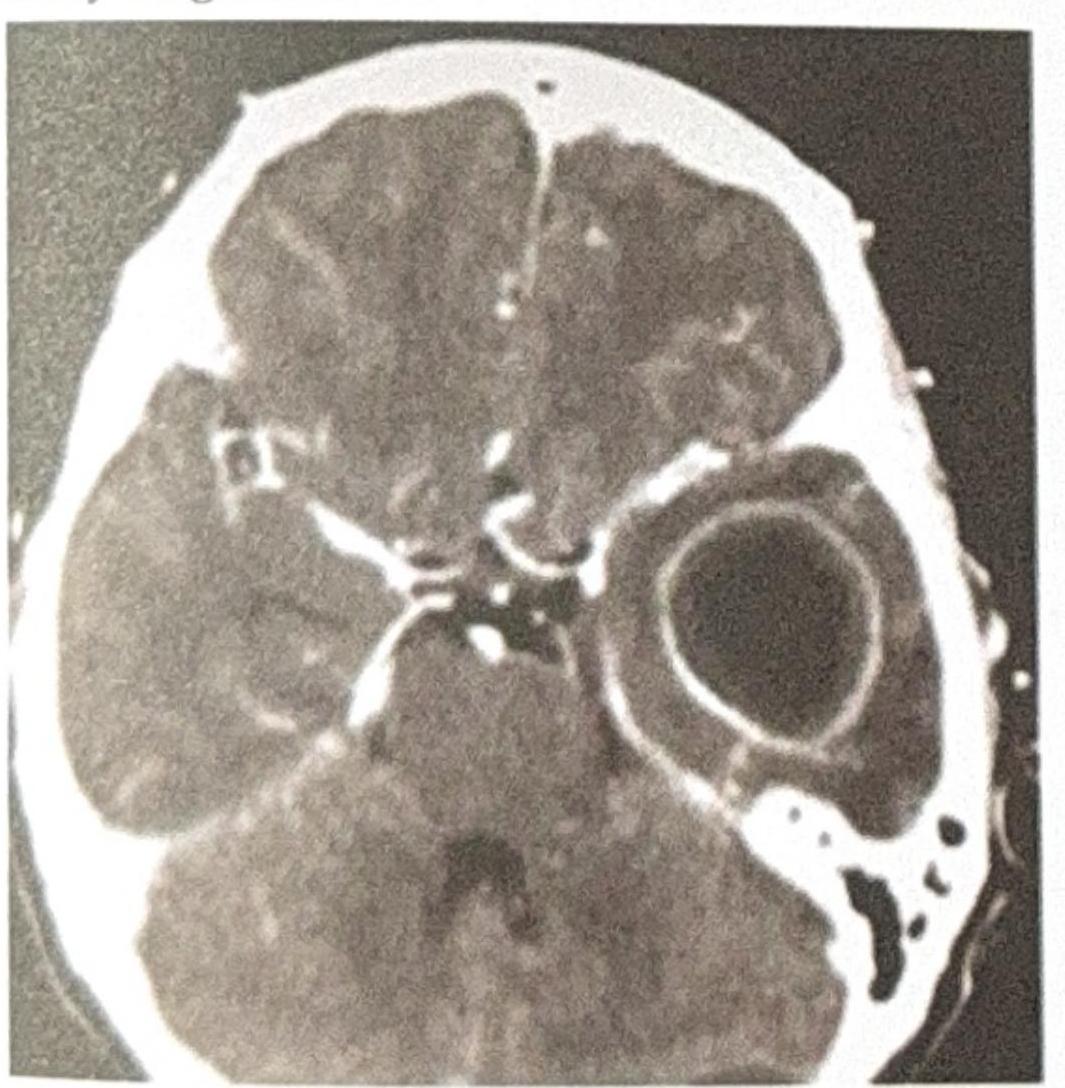
A patient with a history of chronic ear infection now presents with manifestations, including headache and vomiting. A CT brain image is shown. What is the most probable diagnosis?

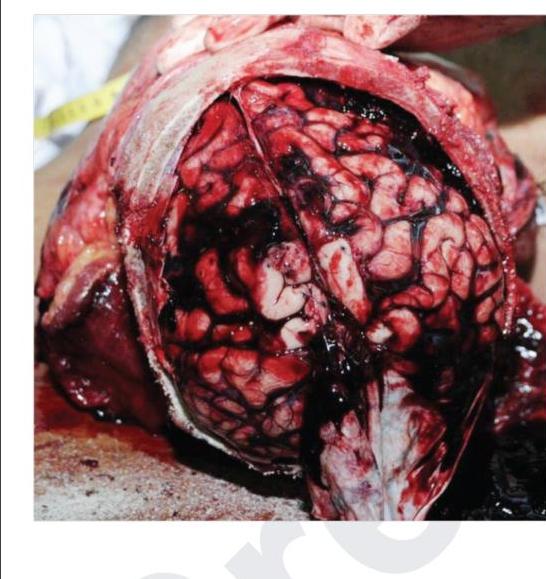
Bleeding as shown in the image is due to which of the following vessels?
A cerebral angiogram shows stenosis of the terminal internal carotid arteries with an abnormal network of collateral vessels. Which finding is most characteristic of moyamoya syndrome?
Practice by Chapter
Neuroanatomy for Radiologists
Practice Questions
Cerebrovascular Diseases
Practice Questions
Intracranial Tumors
Practice Questions
CNS Infections
Practice Questions
Demyelinating and Degenerative Diseases
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Imaging: Trauma and Degenerative Disease
Practice Questions
Spine Tumors and Infections
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital CNS Anomalies
Practice Questions
Functional Neuroimaging
Practice Questions
Neurointerventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
