Neuroradiology — MCQs

On this page
Which of the following is true about giant aneurysms?
In cerebral angiography, through which artery is the dye typically injected?
Which of the following statements about CT scan is FALSE?
Cerebral angiography was performed by whom?
Which condition is characterized by the Lyre sign?
"Lyre sign" is a feature of:
The "face of the giant panda" sign on MRI brain is characteristic of which condition?
A 39-year-old man presents to his physician with the complaint of loss of peripheral vision. The subsequent magnetic resonance imaging (MRI) scan demonstrates what abnormality?
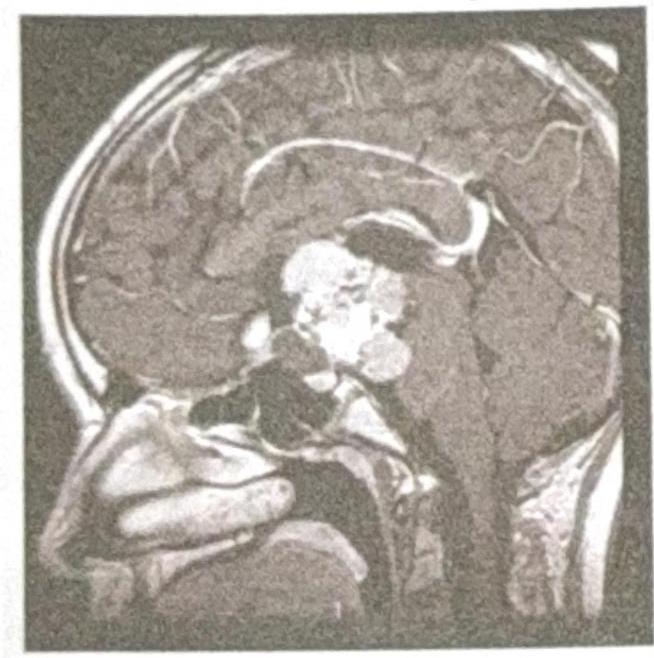
What is your diagnosis?
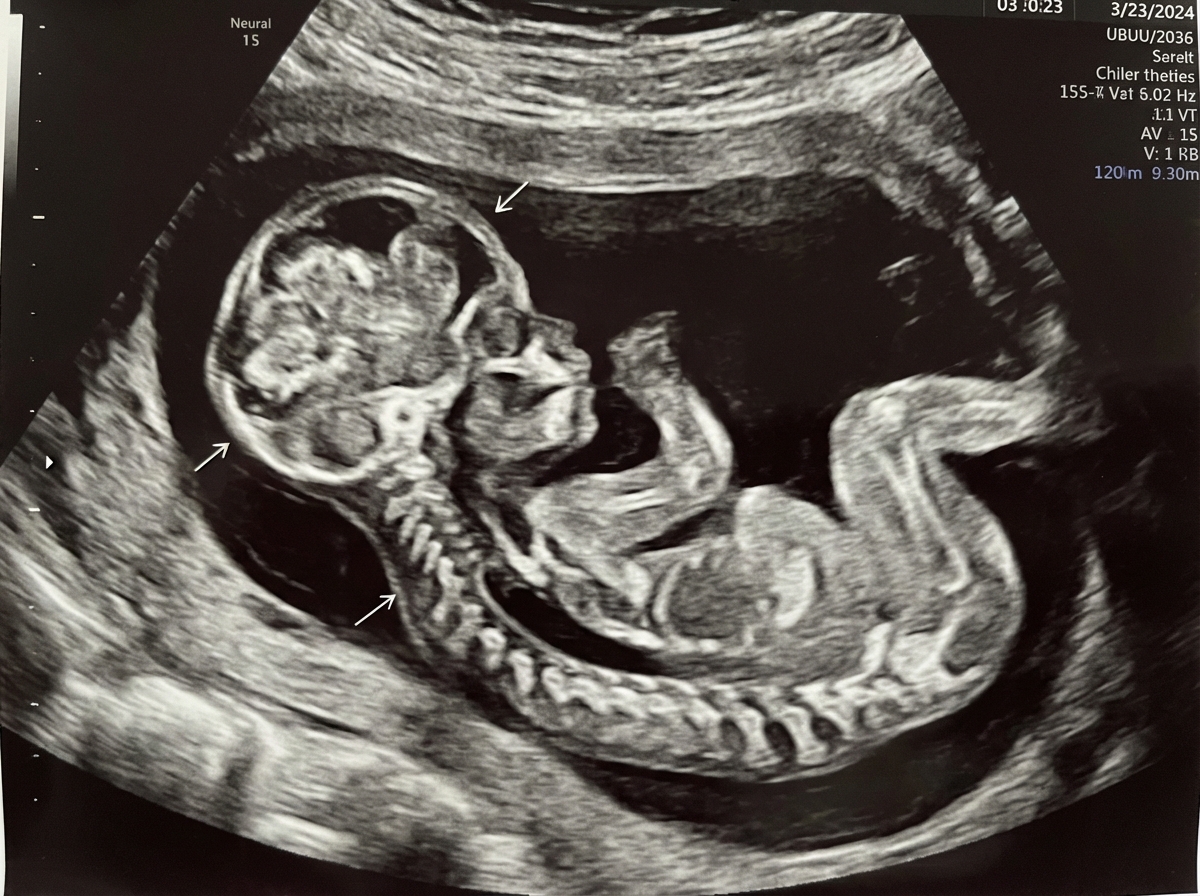
The "Tiger eye sign" on MRI is characteristic of which of the following conditions?
Practice by Chapter
Neuroanatomy for Radiologists
Practice Questions
Cerebrovascular Diseases
Practice Questions
Intracranial Tumors
Practice Questions
CNS Infections
Practice Questions
Demyelinating and Degenerative Diseases
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Imaging: Trauma and Degenerative Disease
Practice Questions
Spine Tumors and Infections
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital CNS Anomalies
Practice Questions
Functional Neuroimaging
Practice Questions
Neurointerventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
