Neuroradiology — MCQs

On this page
In subclavian steal syndrome, there is reversal of blood flow in which artery?
Suprasellar calcification is characteristic of which of the following conditions?
The Lyre sign is observed in which of the following conditions?
What is the characteristic 'thumb sign' on CT head indicative of?
Dawson's fingers on MRI are diagnostic of which condition?
Since 15-20 days, a 40-year-old man is unable to look properly upwards. On CT scan study, a cystic lesion within the inferior oblique muscle with probable mural eccentric 'dot' is noted. What is the most-likely diagnosis?
A 30-year-old female presents with headache and transient obscurations of her vision. On examination, no focal neurological deficit was seen. Which one of the following would you start her on?
Which of the following is the classic CT appearance of an acute subdural hematoma?
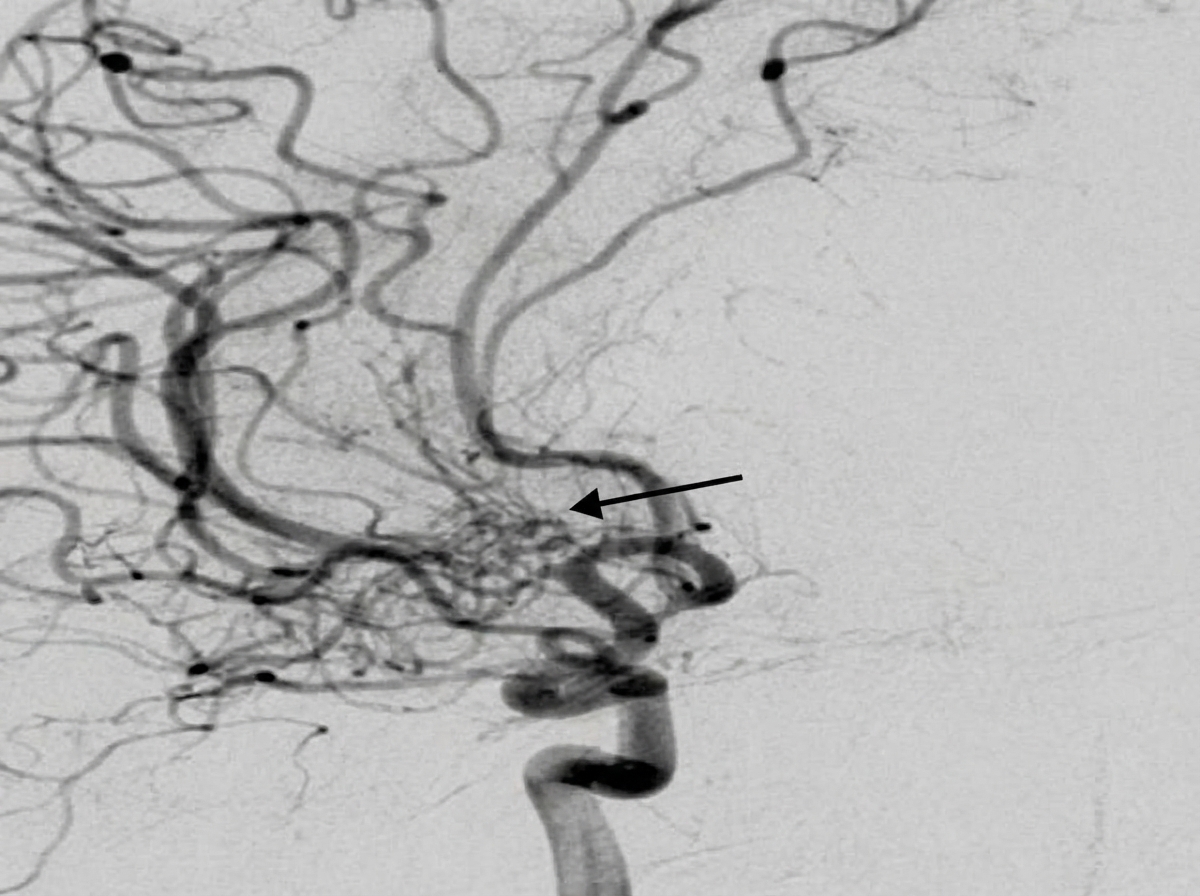
A 20-year-old man from hilly areas presented with epistaxis. DSA showing the sphenopalatine branch of the maxillary artery is provided. The arrow most likely points to which pathology?
The 'swirl sign' is associated with which of the following conditions?
Practice by Chapter
Neuroanatomy for Radiologists
Practice Questions
Cerebrovascular Diseases
Practice Questions
Intracranial Tumors
Practice Questions
CNS Infections
Practice Questions
Demyelinating and Degenerative Diseases
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Imaging: Trauma and Degenerative Disease
Practice Questions
Spine Tumors and Infections
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital CNS Anomalies
Practice Questions
Functional Neuroimaging
Practice Questions
Neurointerventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
