Neuroradiology — MCQs

On this page
Diffuse axonal injury is best detected by which imaging modality?
What is the best investigation of choice for a lesion of the temporal bone?
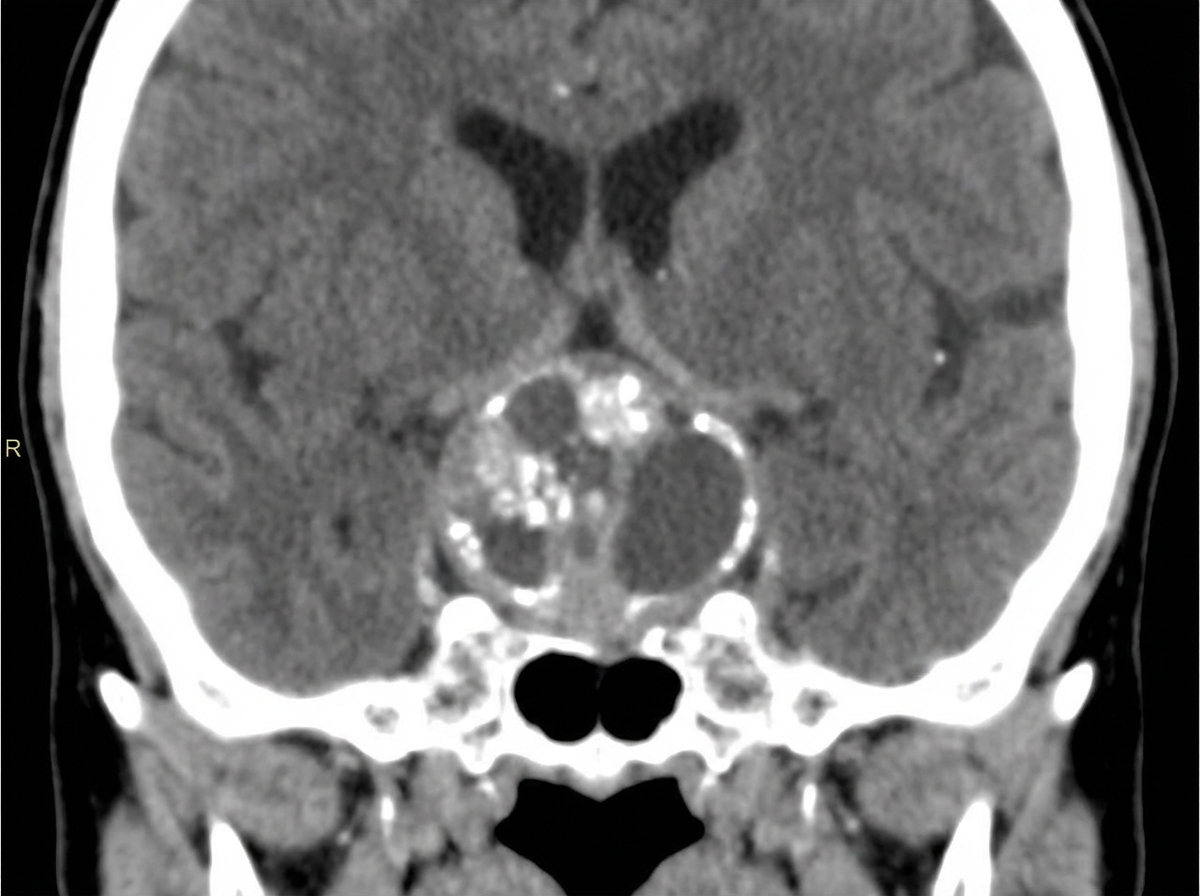
What is the diagnosis for a 10-year-old child presented with vision problems, given the CT scan below?
What does a angiogram of the basilar artery bifurcation show?
What is NOT a feature of Sturge Weber syndrome?
What is the typical Hounsfield unit (HU) value of cerebrospinal fluid (CSF) within the ventricles?
Which of the following is characteristic of Lhermitte-Duclos disease?
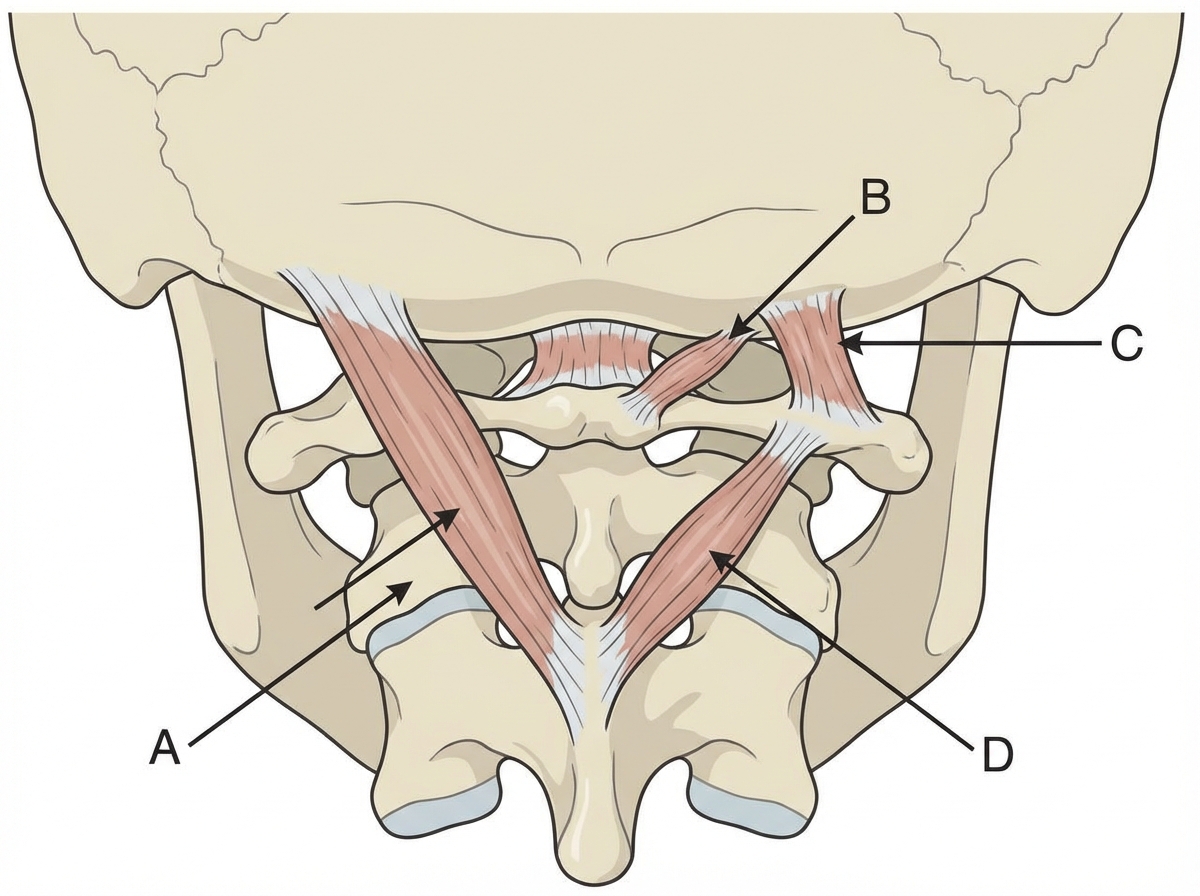
A lesion of the first cervical spinal nerve would cause functional impairment of which structure?
Rail-road calcification in the brain is characteristically found in which of the following conditions?
Which of the following techniques is best for differentiating recurrence of a brain tumor from radiation therapy-induced necrosis?
Practice by Chapter
Neuroanatomy for Radiologists
Practice Questions
Cerebrovascular Diseases
Practice Questions
Intracranial Tumors
Practice Questions
CNS Infections
Practice Questions
Demyelinating and Degenerative Diseases
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Imaging: Trauma and Degenerative Disease
Practice Questions
Spine Tumors and Infections
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital CNS Anomalies
Practice Questions
Functional Neuroimaging
Practice Questions
Neurointerventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
