Neuroradiology — MCQs

On this page
In intervertebral disc prolapse, what does a Schmorl node on MRI imply?
What is the characteristic appearance of a subdural hematoma on CT scan?
The dural tail sign is highly suggestive of which of the following?
Focal bilateral thalamic, posterior internal capsule showing hyperdensity and calcification in CT scan and extensive involvement of deep white matter is characteristic of which condition?
This classical "Ice-cream cone" appearance of an intensely enhancing lesion at the right CP angle recess suggests:
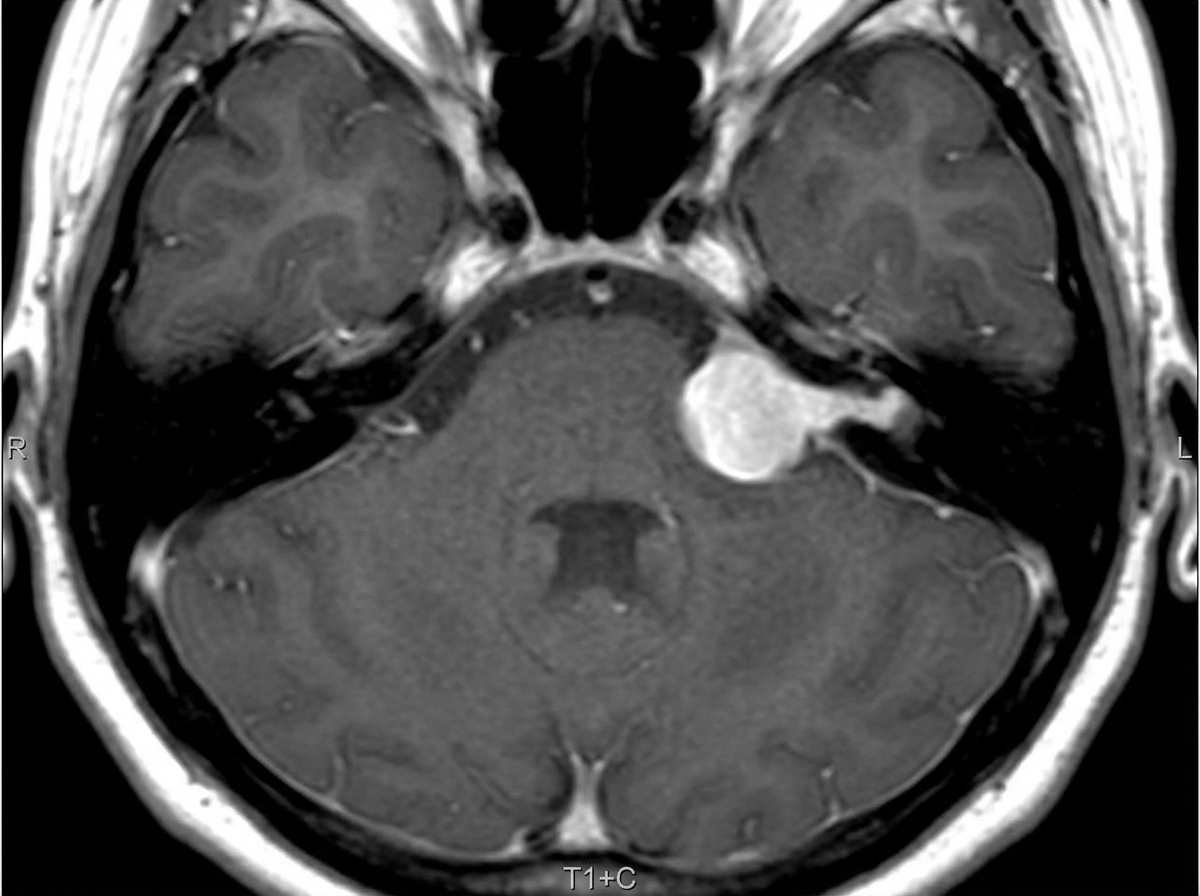
A tumour showing dural enhancement with a tail is characteristic of which of the following entities?
What condition is characterized by a "tram track" appearance on a CT scan of the head?
Wine glass appearance on T2W-MRI Brain is seen with which condition?
All of the following are MRI features of Mesial temporal sclerosis, except:
Trouser leg appearance in myelography is typically seen in which type of spinal cord tumor?
Practice by Chapter
Neuroanatomy for Radiologists
Practice Questions
Cerebrovascular Diseases
Practice Questions
Intracranial Tumors
Practice Questions
CNS Infections
Practice Questions
Demyelinating and Degenerative Diseases
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Imaging: Trauma and Degenerative Disease
Practice Questions
Spine Tumors and Infections
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital CNS Anomalies
Practice Questions
Functional Neuroimaging
Practice Questions
Neurointerventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
