Neuroradiology — MCQs

On this page
J-Shaped sella turica is seen in which condition?
Which of the following represents a midline intra-cranial cyst?
On MRI, how can epidermoids be differentiated from arachnoid cysts?
A patient presents with loss of consciousness following a road traffic accident. CT scan shows multiple spotty hemorrhages and full basal cisterns. What is the most likely diagnosis?
An expansile lytic lesion at the skull base, typically involving the clivus with specks of calcification, is suggestive of which of the following?
Which MRI sequence is used to detect cytotoxic edema before vasogenic edema?
How can an epidermoid cyst be differentiated from an arachnoid cyst?
Which type of hemorrhage classically presents as a lenticular shape on imaging?
What is the imaging modality of choice for diagnosing brain metastases?
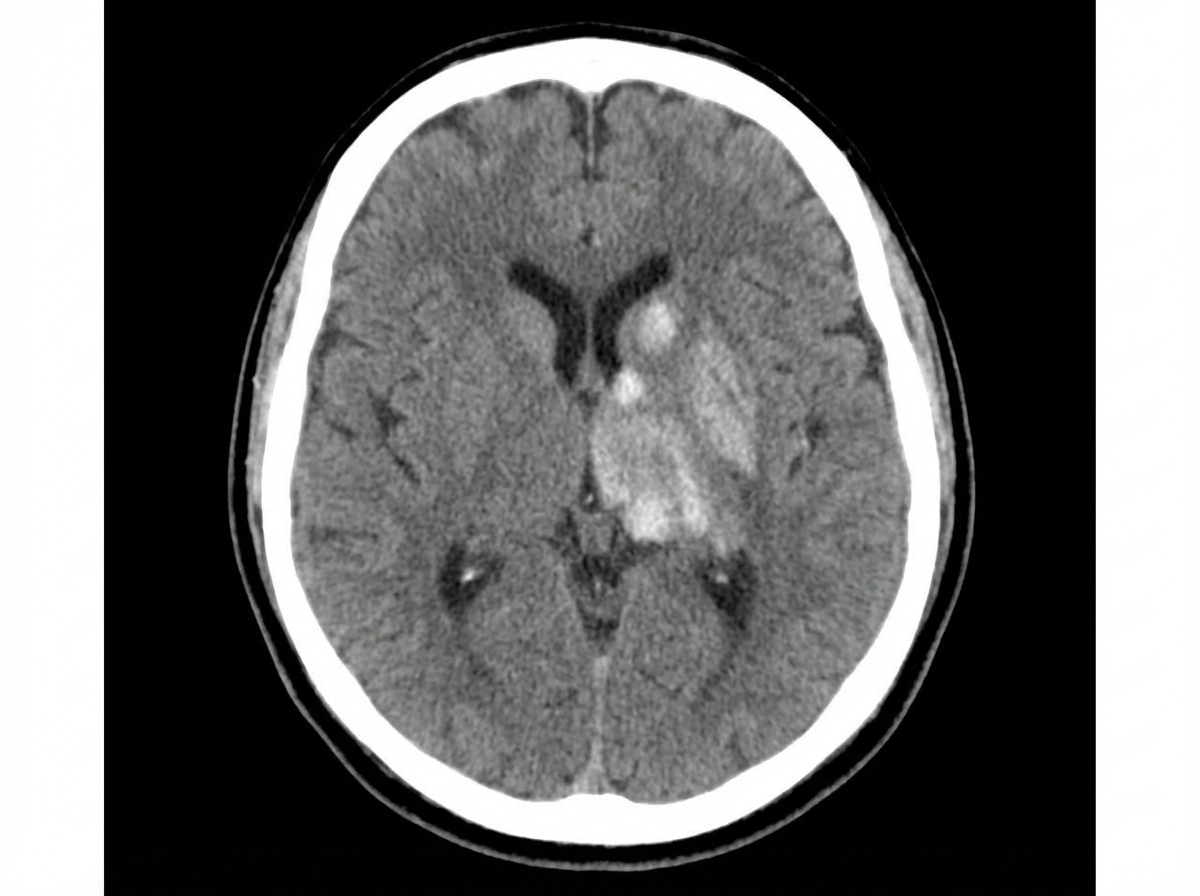
A patient presents with the CT finding shown in the image. Which one of the following signs is this finding most likely to produce?
Practice by Chapter
Neuroanatomy for Radiologists
Practice Questions
Cerebrovascular Diseases
Practice Questions
Intracranial Tumors
Practice Questions
CNS Infections
Practice Questions
Demyelinating and Degenerative Diseases
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Imaging: Trauma and Degenerative Disease
Practice Questions
Spine Tumors and Infections
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital CNS Anomalies
Practice Questions
Functional Neuroimaging
Practice Questions
Neurointerventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
