Neuroradiology — MCQs

On this page
Which of the following is the most vascular tumor?
A cystic lesion with calcification is noted in the suprasellar region. What is the most likely diagnosis?
Craniosynostosis occurs due to premature fusion of which suture(s)?
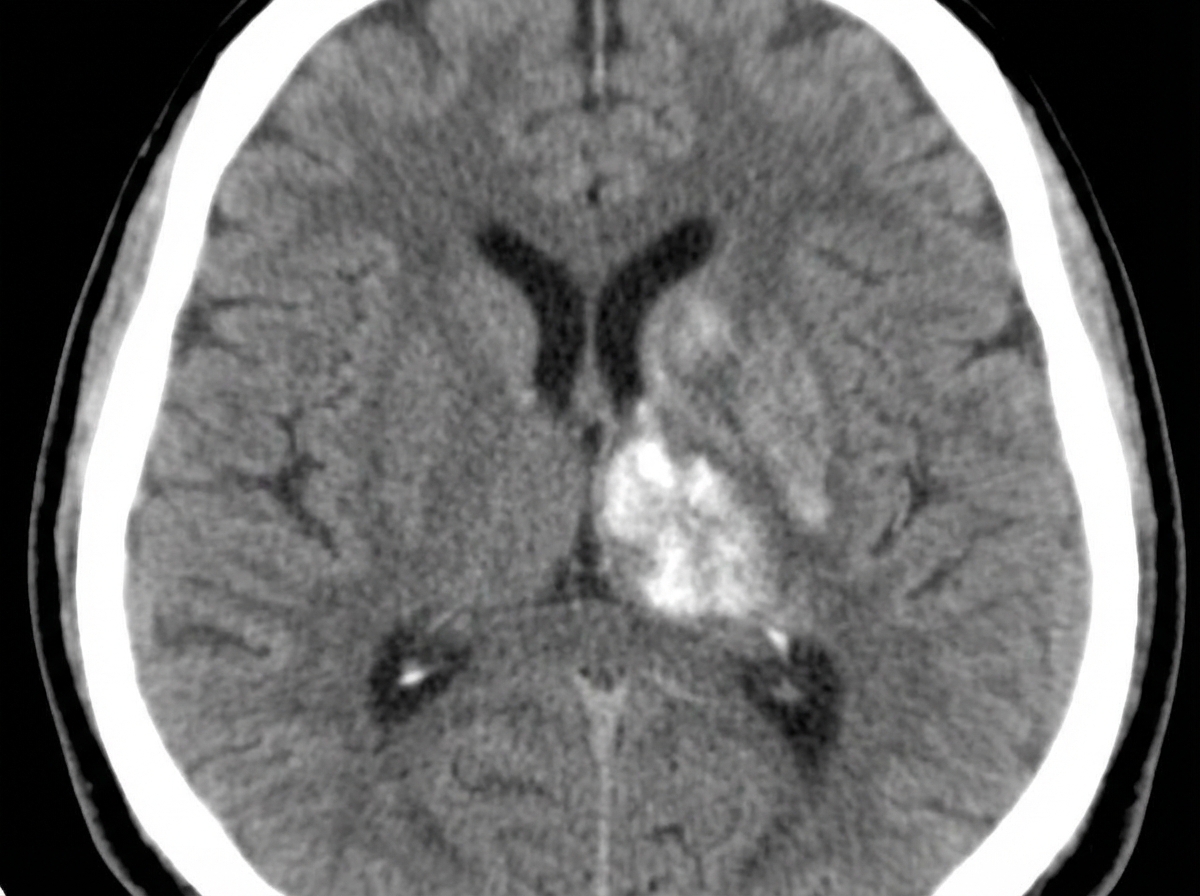
A 63-year-old man complains of worsening headache and right-sided weakness. CT of the head is shown below. What is the most likely diagnosis?
Soap bubble calcification is a feature of which condition?
A hypertensive patient was admitted with right hemiplegia. A plain CT scan shows what?
Basal exudates, infarcts, and hydrocephalus are findings observed in brain imaging studies. What is the most likely diagnosis?
A patient presents with subarachnoid hemorrhage. NCCT reveals blood in the fourth ventricle. The bleeding is most likely to occur from an aneurysm of which of the following arteries?
Premature filling of veins on cerebral angiography is a feature of?
What is the most common cause of intracranial calcification?
Practice by Chapter
Neuroanatomy for Radiologists
Practice Questions
Cerebrovascular Diseases
Practice Questions
Intracranial Tumors
Practice Questions
CNS Infections
Practice Questions
Demyelinating and Degenerative Diseases
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Imaging: Trauma and Degenerative Disease
Practice Questions
Spine Tumors and Infections
Practice Questions
Pediatric Neuroradiology
Practice Questions
Congenital CNS Anomalies
Practice Questions
Functional Neuroimaging
Practice Questions
Neurointerventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
