Spine Imaging — MCQs

Which imaging modality is LEAST useful in the initial diagnosis of stress fractures?
A patient developed paraplegia. On routine examination and X-ray it was found that there are osteoblastic lesions in his spine. What is the MOST probable diagnosis?
Identify the condition shown in the image:
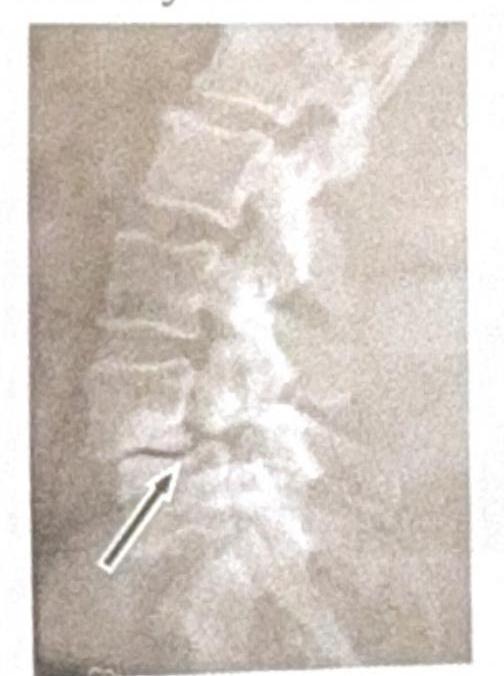
Jefferson fracture is -
Dennis stability concept is based on which of the following?
A 75-year-old female has chronic backache. X-ray of the spine is shown. What is the most likely diagnosis?
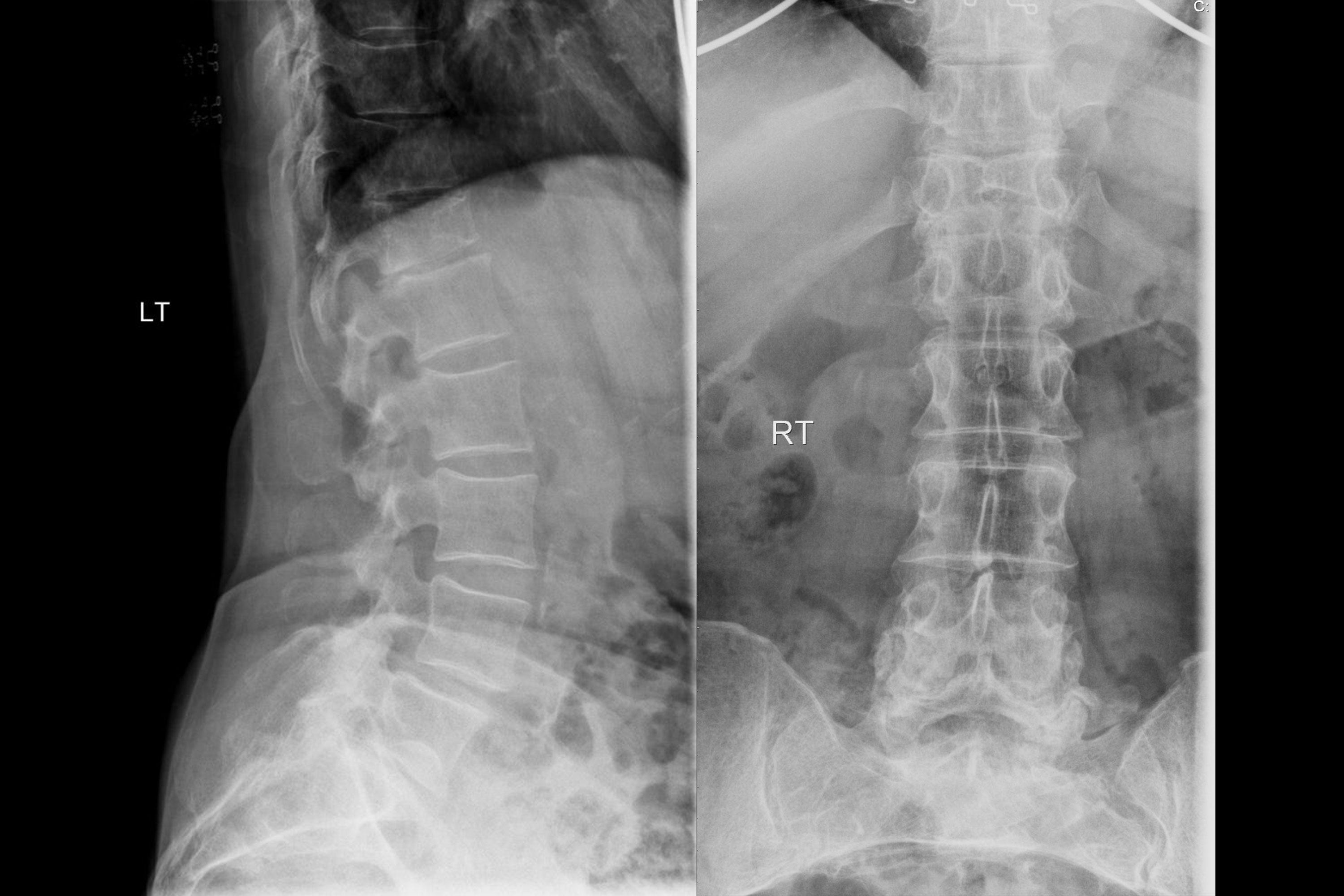
Following are listed as (SpA) spondyloarthritis features except
Scotty dog sign is seen in:
A man presents with back pain following a road traffic accident (RTA). There is no history of neurological deficit. An X-ray of the spine is done. What is the diagnosis based on the image?
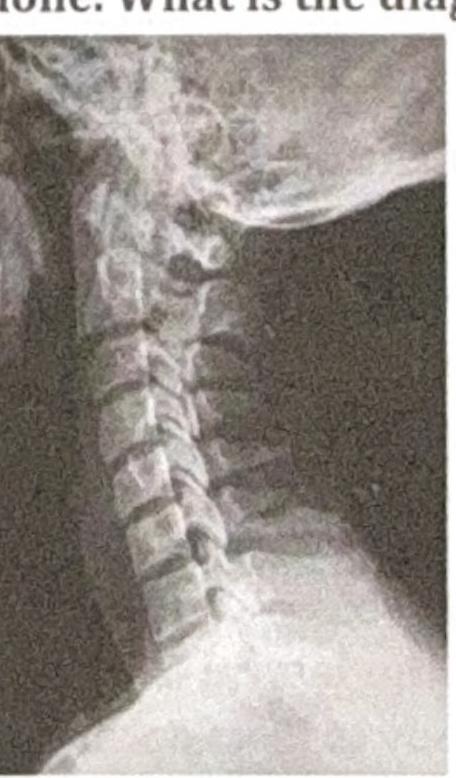
Which of the following is least useful for diagnosing spondylolisthesis?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
