Musculoskeletal Radiology — MCQs

On this page
"Rugger-jersey spine" in X-rays is a characteristic feature of which condition?
What is the characteristic finding on MRI described as a "double line sign"?
Which of the following radiographic projections is contraindicated in patients with cervical spondylitis?
Erlenmeyer flask deformity is seen in which of the following conditions?
Residual asymmetric deformity of the mandible is seen in which condition?
What radiological feature differentiates myositis ossificans from a bone tumor?
What pathology can be seen on X-ray?
Which of the following is NOT a radiological finding seen in rickets?
On an X-ray, what is the appearance of dead bone?
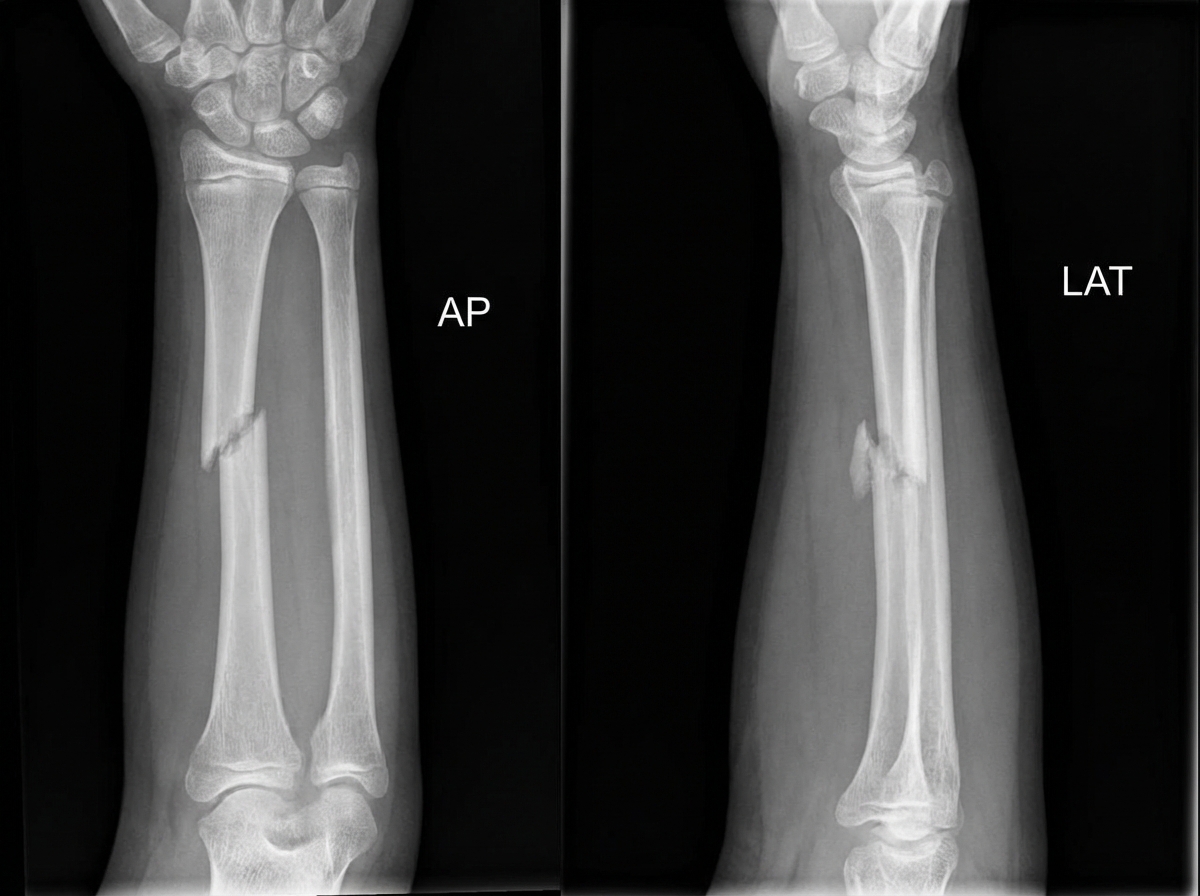
A 13-year-old male presents with forearm pain and deformity after a fall onto his palm. Examination reveals an obvious angulation at the mid-forearm, with intact finger movement, circulation, and sensation. X-rays of the forearm are obtained. What is the most likely diagnosis?
Practice by Chapter
Radiographic Anatomy of Bones and Joints
Practice Questions
Imaging of Fractures and Dislocations
Practice Questions
Arthritides: Inflammatory and Degenerative
Practice Questions
Metabolic Bone Diseases
Practice Questions
Bone and Soft Tissue Tumors
Practice Questions
Congenital Skeletal Anomalies
Practice Questions
Spine Imaging
Practice Questions
Skeletal Infections
Practice Questions
Sports Medicine Imaging
Practice Questions
Imaging of Prostheses and Implants
Practice Questions
Musculoskeletal Ultrasound
Practice Questions
MSK Interventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
