Musculoskeletal Radiology — MCQs

On this page
Investigation of choice for soft tissue sarcoma is -
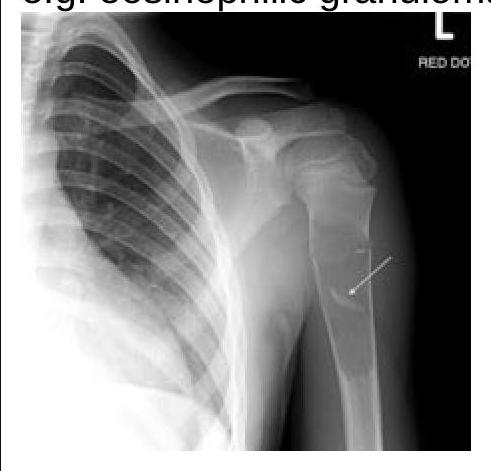
What does the fallen fragment sign indicate in radiology?
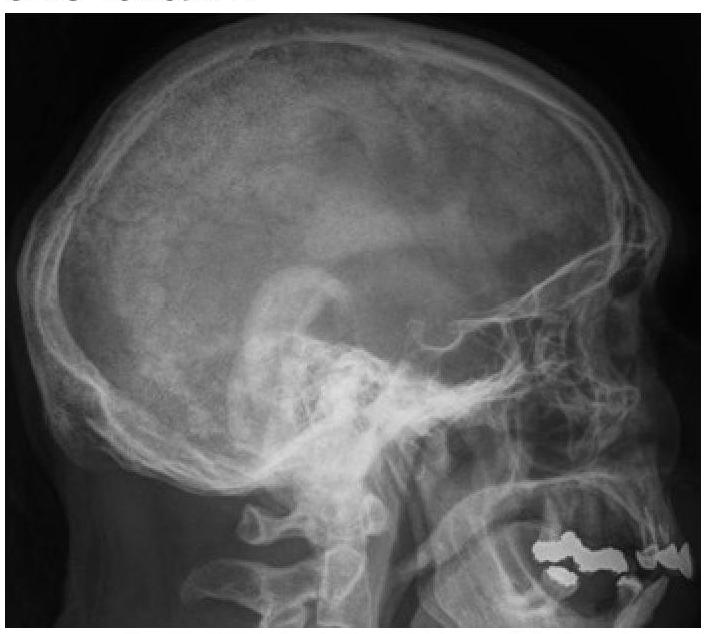
What type of lesions in the skull bones can be identified on this X-ray?
What is the condition characterized by a 'dripping candle wax' appearance on the spine?
Which condition is associated with the pencil in cup deformity?
In which condition is the 'Picture frame vertebra' seen?
Which condition is characterized by a 'moth-eaten' appearance of the bones?
Radiological sign in case of Perthes disease?
"Sunray appearance" on X-rays is suggestive of:
What is seen on x-ray with posterior elbow dislocation
Practice by Chapter
Radiographic Anatomy of Bones and Joints
Practice Questions
Imaging of Fractures and Dislocations
Practice Questions
Arthritides: Inflammatory and Degenerative
Practice Questions
Metabolic Bone Diseases
Practice Questions
Bone and Soft Tissue Tumors
Practice Questions
Congenital Skeletal Anomalies
Practice Questions
Spine Imaging
Practice Questions
Skeletal Infections
Practice Questions
Sports Medicine Imaging
Practice Questions
Imaging of Prostheses and Implants
Practice Questions
Musculoskeletal Ultrasound
Practice Questions
MSK Interventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
