Musculoskeletal Radiology — MCQs

On this page
What is the main diagnostic feature of osteoarthritis on X-ray imaging?
Which investigation is least effective in diagnosing acute osteomyelitis?
Shenton's line is seen in X-ray of -
First radiological sign for active tubercular arthritis is?
X-ray appearance of sequestrum?
Cotton wool skull is a radiological feature of which condition?
Which of the following is not a typical radiological finding in rheumatoid arthritis?
Based on the X-ray image, which condition is indicated by a sunray appearance?
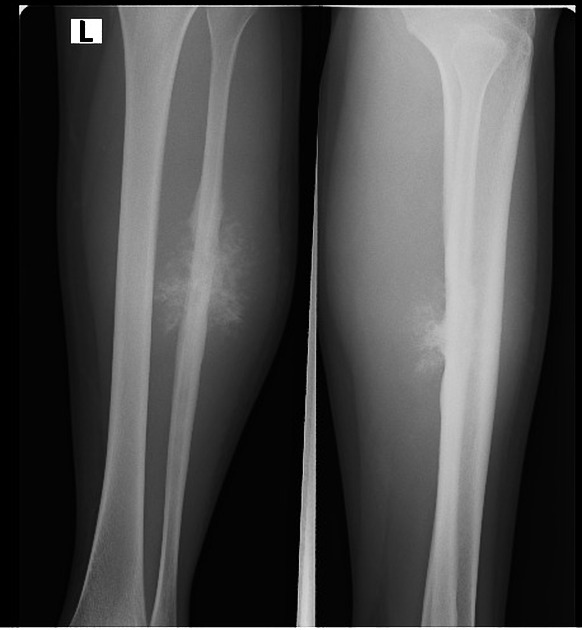
The given image is an x-ray of a 22-year-old female. What is the probable diagnosis based on the x-ray?

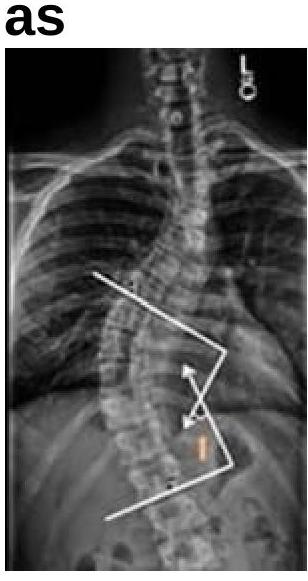
What is the angle shown in the image known as?
Practice by Chapter
Radiographic Anatomy of Bones and Joints
Practice Questions
Imaging of Fractures and Dislocations
Practice Questions
Arthritides: Inflammatory and Degenerative
Practice Questions
Metabolic Bone Diseases
Practice Questions
Bone and Soft Tissue Tumors
Practice Questions
Congenital Skeletal Anomalies
Practice Questions
Spine Imaging
Practice Questions
Skeletal Infections
Practice Questions
Sports Medicine Imaging
Practice Questions
Imaging of Prostheses and Implants
Practice Questions
Musculoskeletal Ultrasound
Practice Questions
MSK Interventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
