Musculoskeletal Radiology — MCQs

On this page
Intraosseous skeletal tumors are best diagnosed by which imaging modality?
Which condition shows the "bone within bone" appearance radiologically?
Maclean's sign is seen in which of the following conditions?
Multiple periapical radiolucencies are seen in which of the following conditions?
Marble Bone disease is characterized by which of the following conditions?
The "Scottish Dog Terrier" appearance on X-ray is seen in which condition?
A lateral view X-ray of the lumbosacral spine shows which of the following findings?
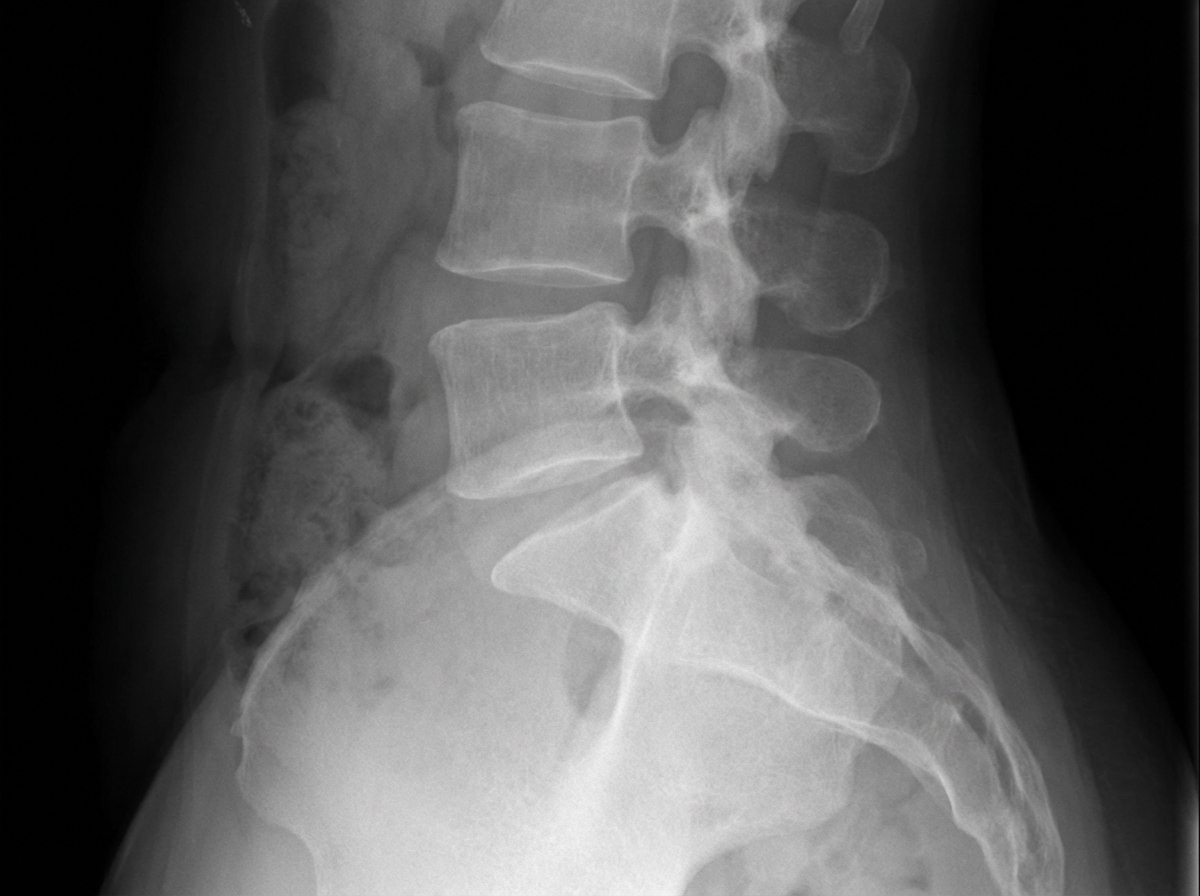
A Judet view on an X-ray is primarily used for visualizing injuries to which anatomical structure?
Which of the following is the most probable diagnosis of the patient with the given X-ray?
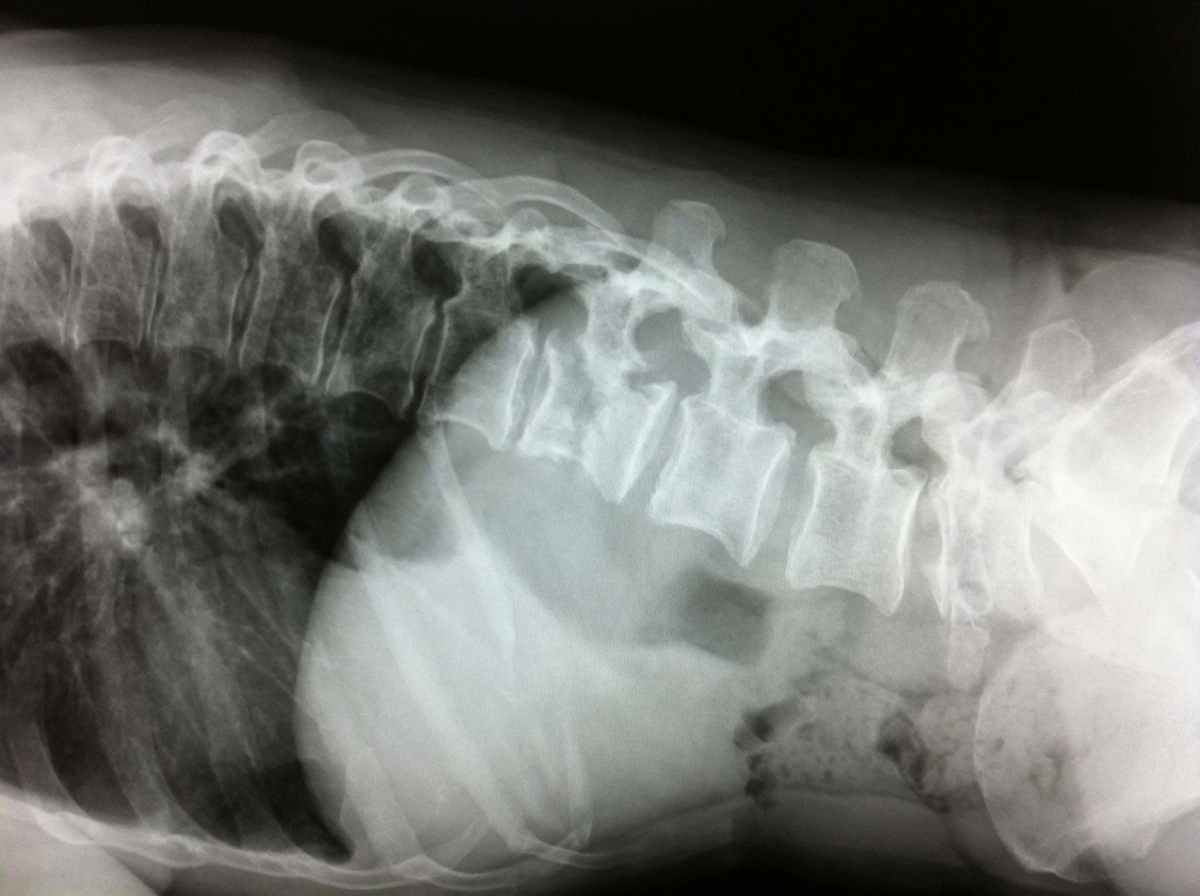
Which X-ray needs to be taken for a 16-year-old male?
Practice by Chapter
Radiographic Anatomy of Bones and Joints
Practice Questions
Imaging of Fractures and Dislocations
Practice Questions
Arthritides: Inflammatory and Degenerative
Practice Questions
Metabolic Bone Diseases
Practice Questions
Bone and Soft Tissue Tumors
Practice Questions
Congenital Skeletal Anomalies
Practice Questions
Spine Imaging
Practice Questions
Skeletal Infections
Practice Questions
Sports Medicine Imaging
Practice Questions
Imaging of Prostheses and Implants
Practice Questions
Musculoskeletal Ultrasound
Practice Questions
MSK Interventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
