Musculoskeletal Radiology — MCQs

On this page
What is the normal metacarpal index?
Subperiosteal erosion is seen in which of the following conditions?
Raindrop skull is seen in which of the following conditions?
Which of the following is NOT a radiological feature of rickets?
All of the following are X-ray findings of Rheumatoid Arthritis except?
Subperiosteal resorption, most apparent on the radial aspect of the middle phalanx of the second and third fingers, is characteristic of which condition?
What is the earliest radiological change observed in rheumatoid arthritis (RA)?
The most likely pathology associated with the following radiograph is:
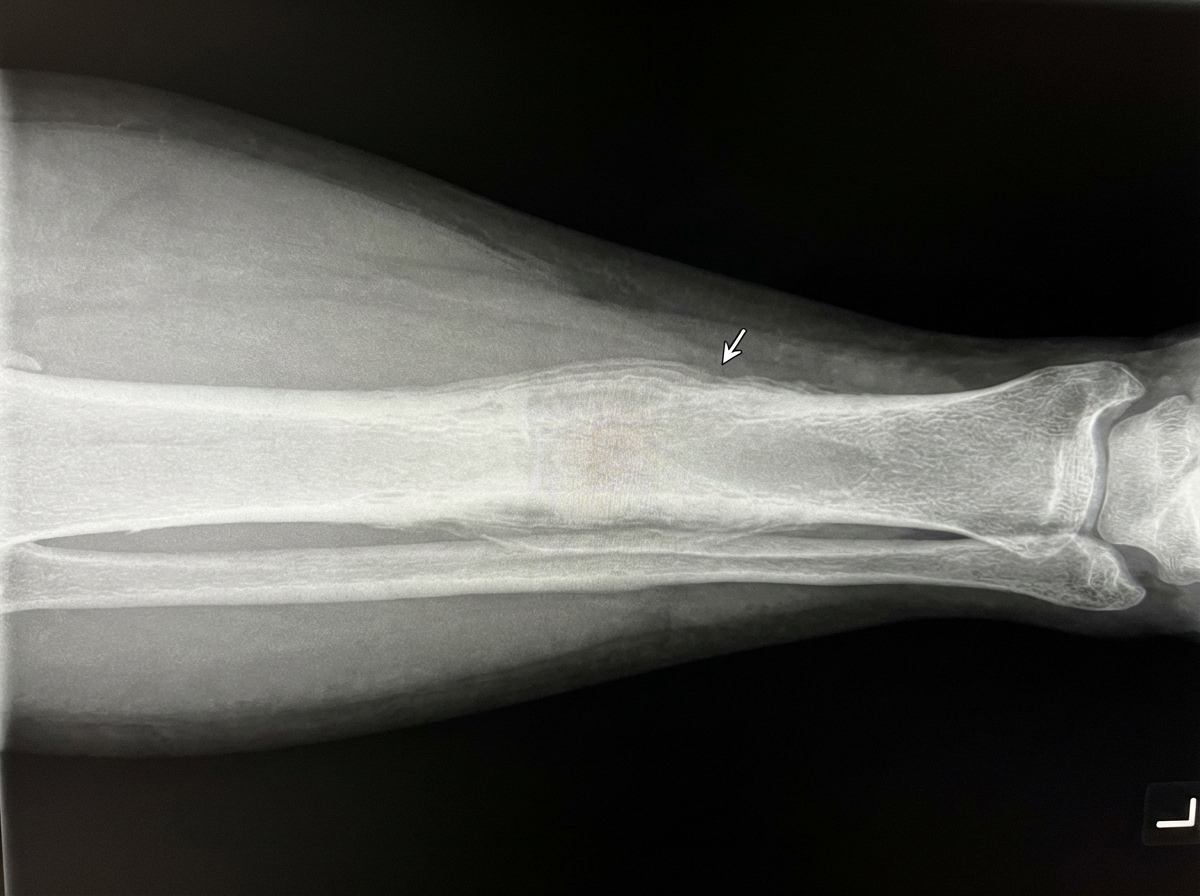
All of the following are radiological signs of scurvy except?
Anterior scalloping of vertebrae is seen in which of the following conditions?
Practice by Chapter
Radiographic Anatomy of Bones and Joints
Practice Questions
Imaging of Fractures and Dislocations
Practice Questions
Arthritides: Inflammatory and Degenerative
Practice Questions
Metabolic Bone Diseases
Practice Questions
Bone and Soft Tissue Tumors
Practice Questions
Congenital Skeletal Anomalies
Practice Questions
Spine Imaging
Practice Questions
Skeletal Infections
Practice Questions
Sports Medicine Imaging
Practice Questions
Imaging of Prostheses and Implants
Practice Questions
Musculoskeletal Ultrasound
Practice Questions
MSK Interventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
