Musculoskeletal Radiology — MCQs

On this page
Which one of the following conditions is not associated with cupping and fraying of metaphyses of long bones in children?
Wimberger ring sign is present in which condition?
The Scottish terrier sign is typically observed in which radiographic view?
In a patient presenting with shoulder pain and no clear history of trauma, what does this radiograph most likely suggest?
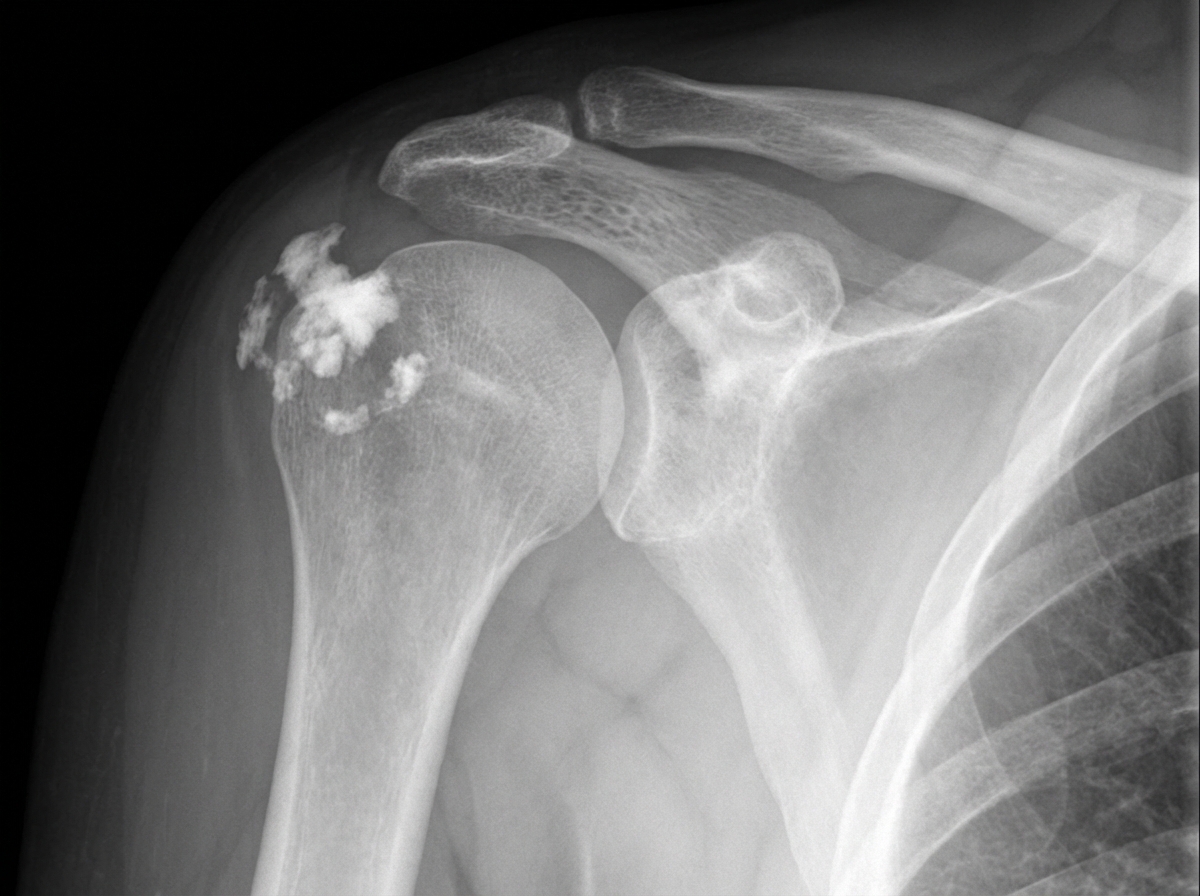
What is the possible diagnosis based on the provided X-ray image?
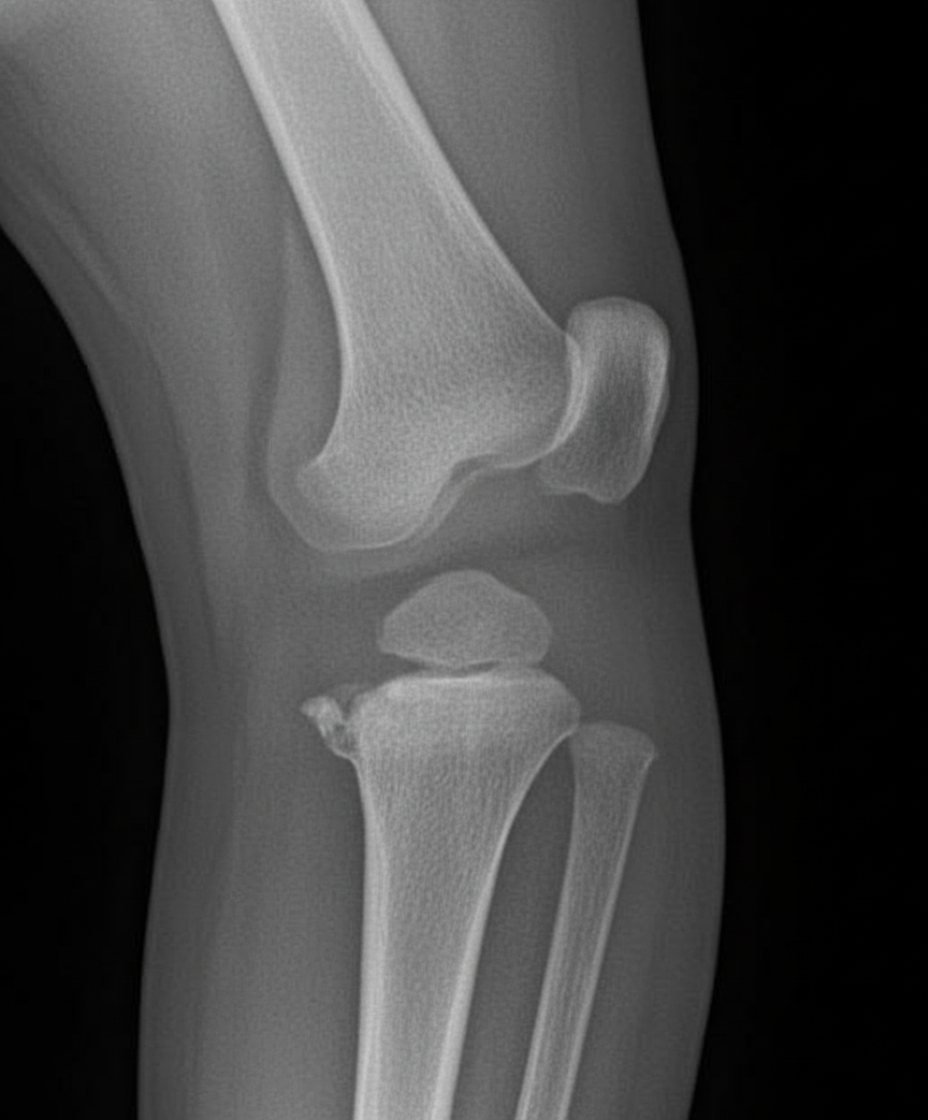
What is the best imaging modality to distinguish acute osteomyelitis from a soft tissue infection?
"Corner sign of Park" is a feature of which of the following conditions?
Bone density is best studied by which imaging modality?
Trolly tract sign is seen in which of the following conditions?
What is the best method to evaluate a discrepancy in the articular disc of the temporomandibular joint (TMJ)?
Practice by Chapter
Radiographic Anatomy of Bones and Joints
Practice Questions
Imaging of Fractures and Dislocations
Practice Questions
Arthritides: Inflammatory and Degenerative
Practice Questions
Metabolic Bone Diseases
Practice Questions
Bone and Soft Tissue Tumors
Practice Questions
Congenital Skeletal Anomalies
Practice Questions
Spine Imaging
Practice Questions
Skeletal Infections
Practice Questions
Sports Medicine Imaging
Practice Questions
Imaging of Prostheses and Implants
Practice Questions
Musculoskeletal Ultrasound
Practice Questions
MSK Interventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
