Musculoskeletal Radiology — MCQs

On this page
A 48-year-old man with a long history of low back pain presents with similar symptoms. His previous X-ray 6 years ago showed degenerative disc changes. What should be done next?
Which of the following conditions is NOT associated with the 'bone within a bone' appearance?
In ankylosing spondylitis, what are the first radiological changes seen?
Raindrop skull is a characteristic finding in which of the following conditions?
What is the earliest radiological sign indicative of sacroiliitis on X-ray?
Shenton's line is a radiological line used to determine the pathology of:
All of the following are seen in rickets except?
What is the finding seen on X-ray of the right shoulder?
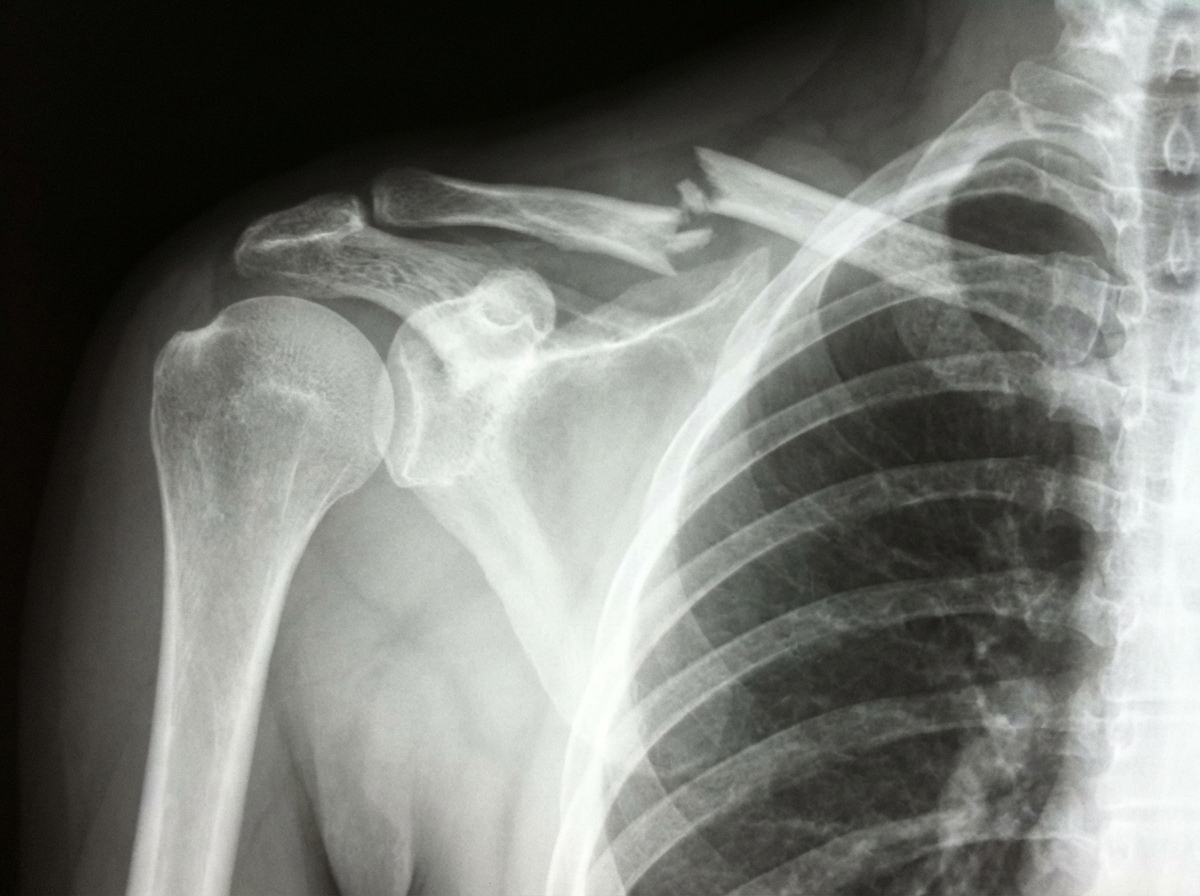
Which of the following is the most common cause of sclerotic skeletal metastasis in a female patient?
A hair on end appearance of the skull is seen in all of the following conditions EXCEPT:
Practice by Chapter
Radiographic Anatomy of Bones and Joints
Practice Questions
Imaging of Fractures and Dislocations
Practice Questions
Arthritides: Inflammatory and Degenerative
Practice Questions
Metabolic Bone Diseases
Practice Questions
Bone and Soft Tissue Tumors
Practice Questions
Congenital Skeletal Anomalies
Practice Questions
Spine Imaging
Practice Questions
Skeletal Infections
Practice Questions
Sports Medicine Imaging
Practice Questions
Imaging of Prostheses and Implants
Practice Questions
Musculoskeletal Ultrasound
Practice Questions
MSK Interventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
