MSK Interventional Procedures — MCQs

Identify the condition shown in the image:
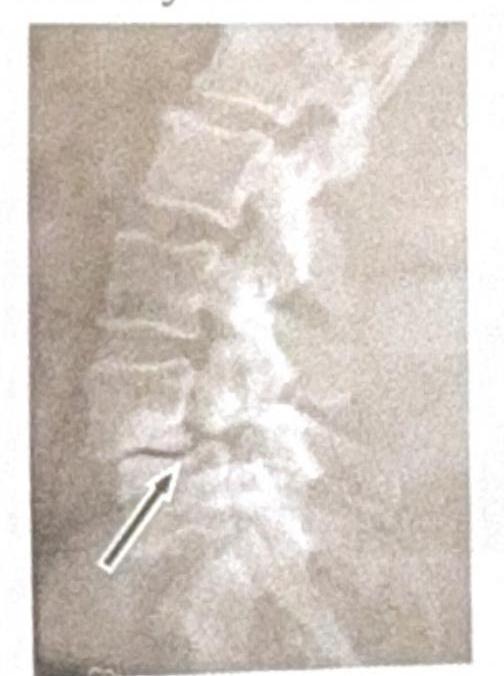
An athlete sustained an injury around the knee joint, suspecting cartilage damage. Which of the following is the investigation of choice?
Which of the following thyroid carcinomas cannot be definitively diagnosed by fine needle aspiration cytology (FNAC)?
A 10 cm tumor is found on the anterior surface of the thigh. What is the most appropriate procedure to obtain a diagnosis?
A 10-year-old obese boy was referred to the emergency department with a history of hip pain. He was observed to be limping and complained of severe pain. Which of the following investigations is least appropriate for this condition?
In which condition is the cleavage plane sign typically observed?
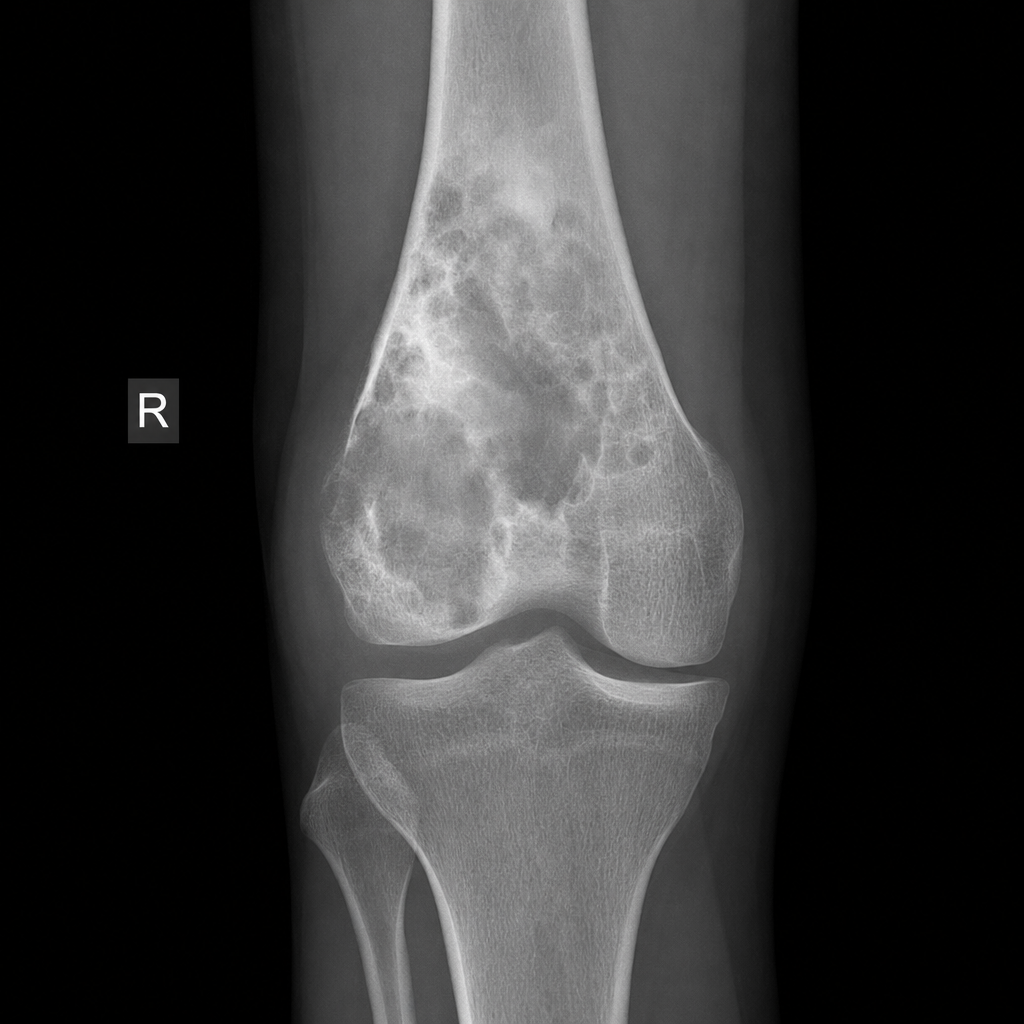
A 16-year-old male presents with a 6-week history of progressively worsening pain and swelling around the right knee. The pain is worse at night and does not respond to analgesics. There is no history of trauma. Serum alkaline phosphatase is markedly elevated. A plain radiograph of the distal femur is shown in Image 3. Which investigation should be performed next to best assess local extent of disease and guide surgical planning?
Superior rib notching is caused by which of the following?
What is the most common source of error leading to a false positive finding of dental caries?
Spoke wheel calcification in an osteolytic lesion is seen in which of the following conditions?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
