Emergency Radiology — MCQs

On this page
Most sensitive investigation for abdominal trauma in a hemodynamically stable patient is-
In a hemodynamically stable patient with abdominal trauma, which imaging modality is considered the gold standard for diagnosing and grading solid organ injuries?
A 45-year-old female presents with the acute onset of a severe headache and vomiting. A non-contrast CT shows a crescent-shaped hyperdense area crossing suture lines. What is the most likely diagnosis?
What is the investigation of choice for diagnosing solid organ injuries in abdominal trauma?
A 75-year-old male with a history of hypertension presents with sudden-onset severe abdominal pain radiating to the back. Which diagnostic tool would be most beneficial in differentiating between a ruptured abdominal aneurysm and acute pancreatitis?
Investigation of choice to evaluate intracranial hemorrhage of less than 48 hours is -
Tear drop sign is seen in?
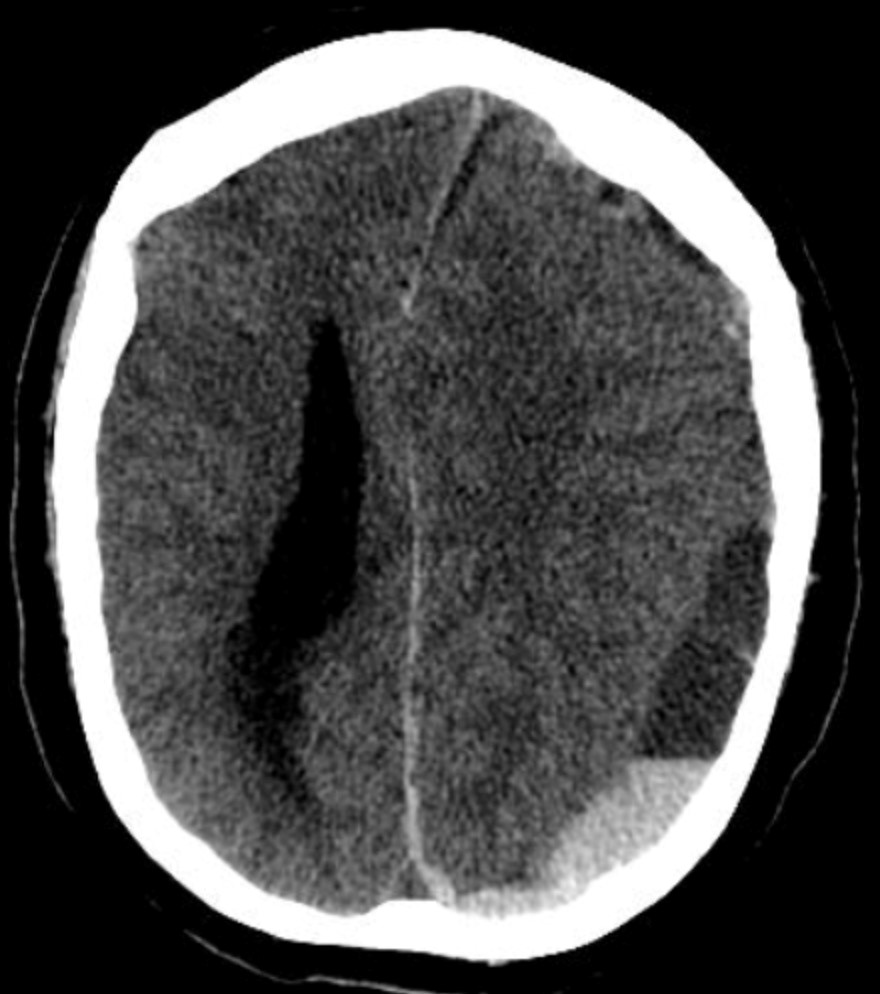
A polytrauma patient's CT brain shows a crescent-shaped extra-axial collection with a concave inner margin. What is the most likely diagnosis?
The most appropriate investigation to diagnose and determine the extent of renal injury in a 15-year-old boy who presents with hematuria and left-sided abdominal pain 48 hours after sustaining a blunt abdominal injury, with a pulse rate of 96/minute, blood pressure of 110/70 mmHg, hemoglobin of 10.8 gm%, and packed cell volume of 31%, would be-
Thumb sign in lateral X-ray of the neck is seen in?
Practice by Chapter
Trauma Imaging Protocols
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Trauma Imaging
Practice Questions
Chest Trauma Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Musculoskeletal Trauma Imaging
Practice Questions
Non-traumatic Neurological Emergencies
Practice Questions
Non-traumatic Thoracic Emergencies
Practice Questions
Non-traumatic Abdominal Emergencies
Practice Questions
Vascular Emergencies
Practice Questions
Pediatric Emergency Imaging
Practice Questions
Imaging of Non-accidental Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
