Emergency Radiology — MCQs

On this page
What is the imaging modality of choice in the setting of head trauma?
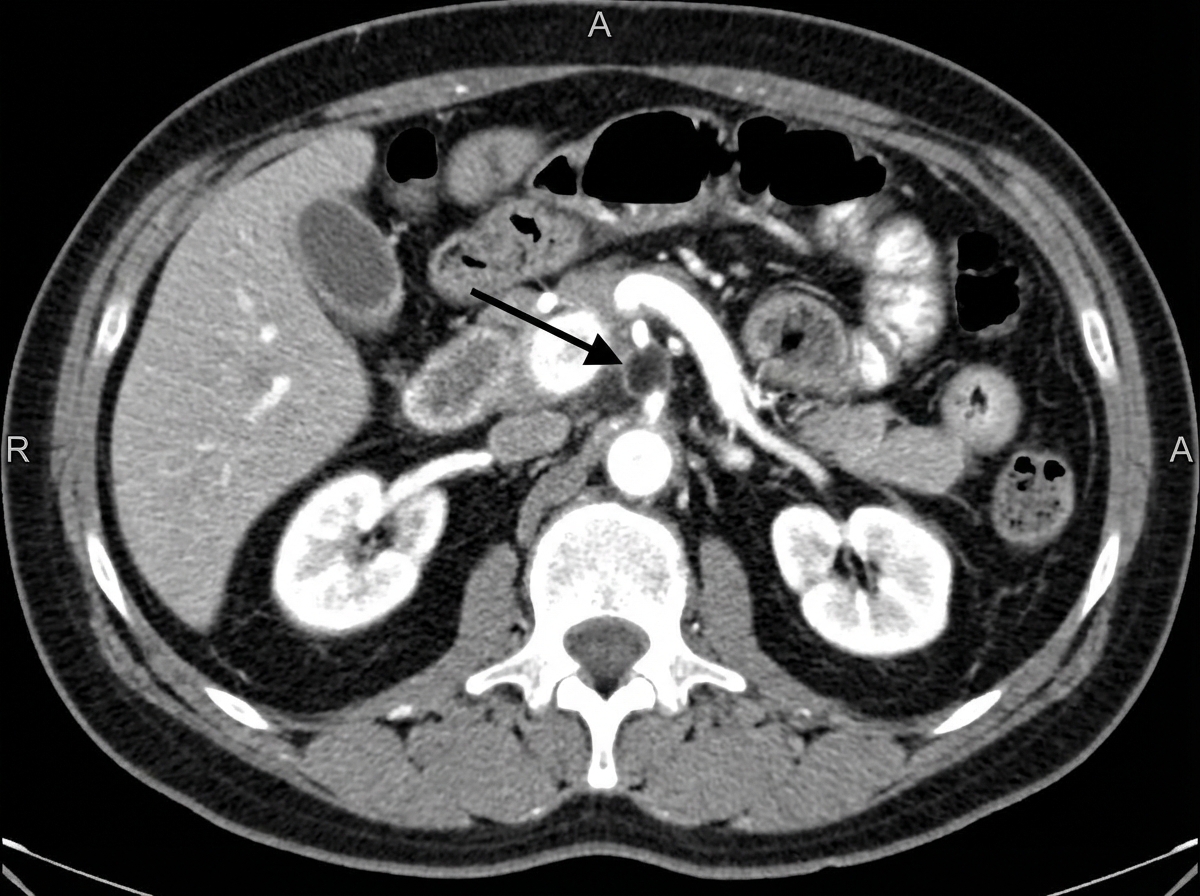
A patient presents to the emergency department with abdominal pain. What is the MOST significant diagnosis?
Pneumatocele is seen in fracture of which sinus?
The dependant viscera sign is seen in which of the following conditions?
Computed tomography (CT) is useful in the formulation of a treatment plan of blow-out fractures because:
What is the investigation of choice for the evaluation of upper abdominal trauma in a patient with stable vitals?
Which of the following appears hyperdense on CT?
Which radiographic view best visualizes zygoma fractures?
Pneumocephalus is most commonly seen with fractures of which anatomical structure?
Tear drop sign is seen in:
Practice by Chapter
Trauma Imaging Protocols
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Trauma Imaging
Practice Questions
Chest Trauma Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Musculoskeletal Trauma Imaging
Practice Questions
Non-traumatic Neurological Emergencies
Practice Questions
Non-traumatic Thoracic Emergencies
Practice Questions
Non-traumatic Abdominal Emergencies
Practice Questions
Vascular Emergencies
Practice Questions
Pediatric Emergency Imaging
Practice Questions
Imaging of Non-accidental Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
