Emergency Radiology — MCQs

On this page
A patient presents with a forefinger injury from glass, with suspicion of a retained foreign body. What is the initial investigation of choice?
For the evaluation of blunt abdominal trauma, which of the following imaging modalities is ideal?
What is the full form of FAST?
A tripod fracture is a fracture of which bone?
A patient presents with a blood pressure of 90/60 mmHg and a pulse rate of 150 beats per minute following blunt abdominal trauma. What is the initial assessment tool you would use?
Based upon this coronal CT view of the face in a 25-year-old man with eye pain, what is the MOST likely diagnosis?
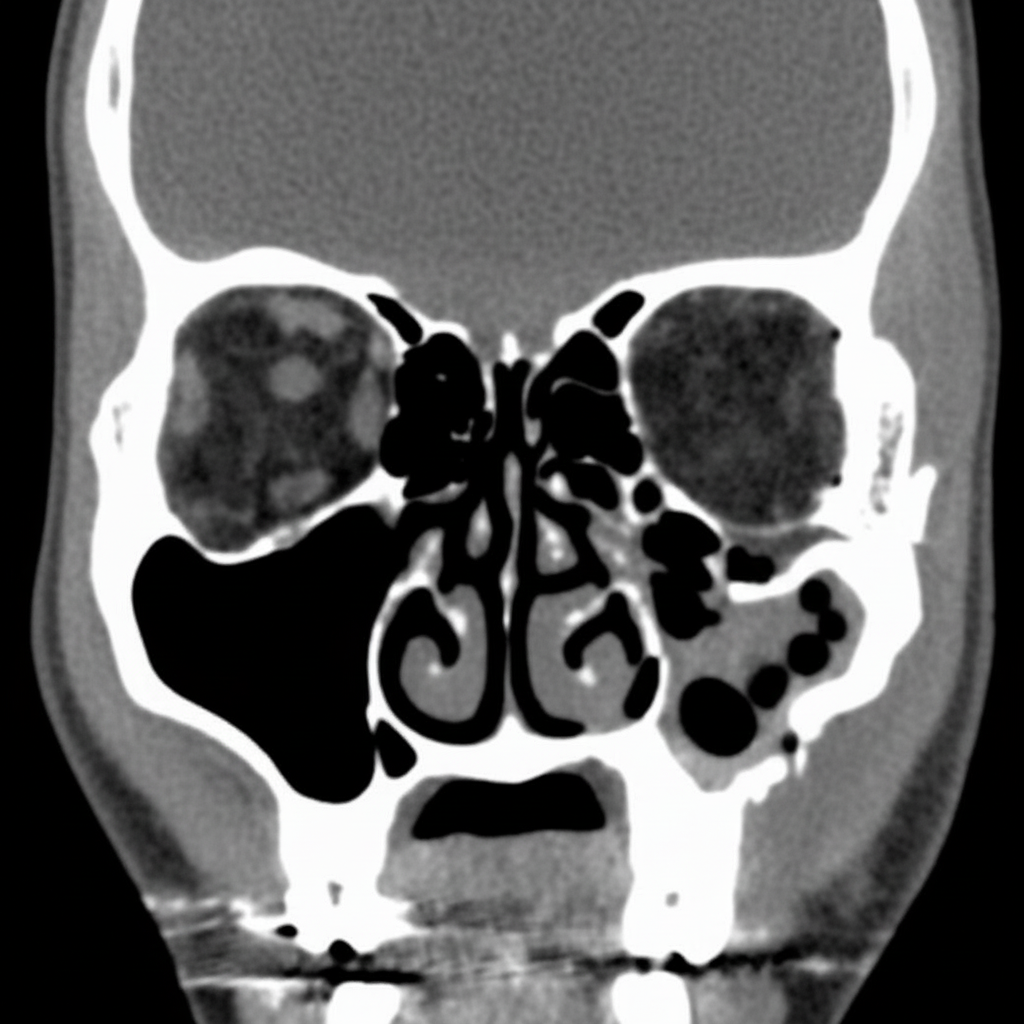
Splenic injury is best detected by:
The "tear drop sign" is characteristic of which of the following conditions?
A 19-year-old boy presents with a swollen lip and fractured maxillary central incisors following trauma. The encircled area in the radiograph shows:
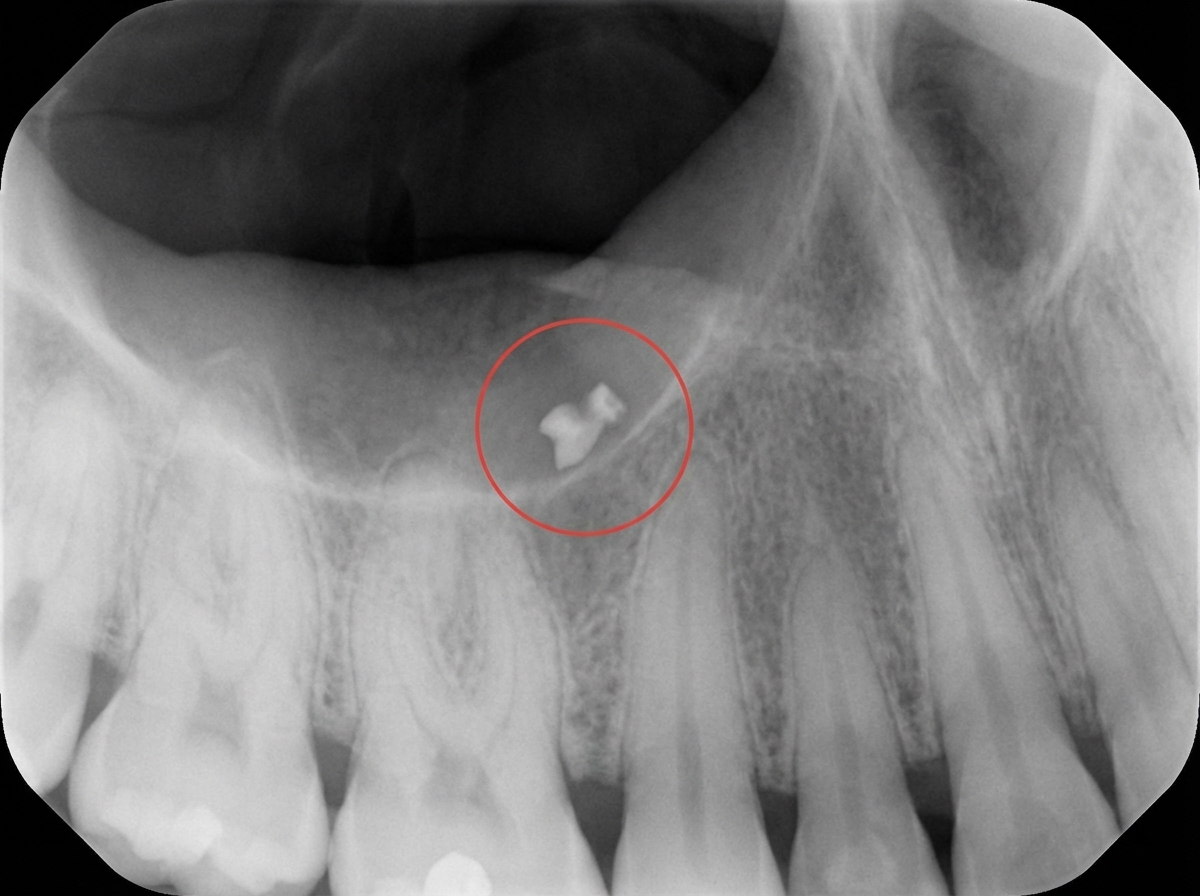
Which imaging modality is the mainstay in trauma imaging?
Practice by Chapter
Trauma Imaging Protocols
Practice Questions
Head Trauma Imaging
Practice Questions
Spine Trauma Imaging
Practice Questions
Chest Trauma Imaging
Practice Questions
Abdominal Trauma Imaging
Practice Questions
Musculoskeletal Trauma Imaging
Practice Questions
Non-traumatic Neurological Emergencies
Practice Questions
Non-traumatic Thoracic Emergencies
Practice Questions
Non-traumatic Abdominal Emergencies
Practice Questions
Vascular Emergencies
Practice Questions
Pediatric Emergency Imaging
Practice Questions
Imaging of Non-accidental Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
