Contrast Media and Reactions — MCQs

On this page
Which of the following drugs is NOT used to prevent contrast nephropathy?
Which contrast agent is typically used for Magnetic Resonance Imaging (MRI)?
Which of the following contrast agents is preferred in a patient with decreased renal function to avoid contrast nephropathy?
Contrast-induced nephropathy is defined as a rise in serum creatinine by:
What contrast dye(s) are used in MRI?
Which of the following is a non-iodinated contrast agent?
A patient is to undergo angiography for unstable angina and has an elevated serum creatinine. Which of the following measures is NOT used to prevent contrast nephropathy?
Allergic-like reactions to radiological contrast agents are predominantly:
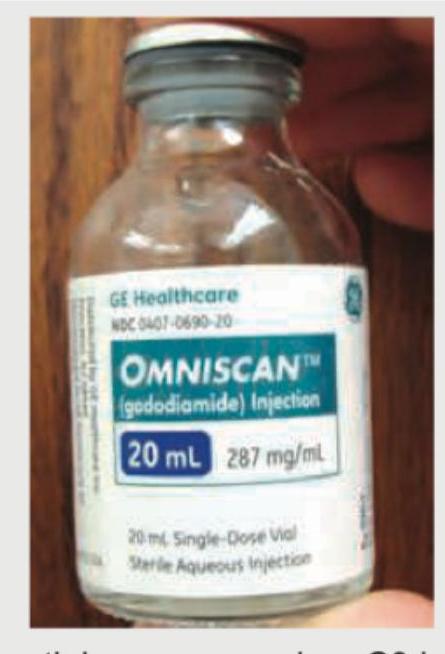
Which of the following investigations must be performed before giving the agent shown to a patient?
Iodine particle ratio for Ionic dimer is
Practice by Chapter
Chemistry of Contrast Media
Practice Questions
Pharmacokinetics of Contrast Agents
Practice Questions
Classification of Contrast Reactions
Practice Questions
Risk Factors for Contrast Reactions
Practice Questions
Prevention of Contrast Reactions
Practice Questions
Treatment of Acute Contrast Reactions
Practice Questions
Contrast-Induced Nephropathy
Practice Questions
Nephrogenic Systemic Fibrosis
Practice Questions
Extravasation of Contrast Media
Practice Questions
Guidelines for Contrast Administration
Practice Questions
Alternative Contrast Agents
Practice Questions
Documentation and Medicolegal Aspects
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
