Contrast and Radiological Procedures — MCQs

On this page
Which law does the paralleling technique in radiography obey?
The angiogram depicted below is most typical of a patient whose history includes:
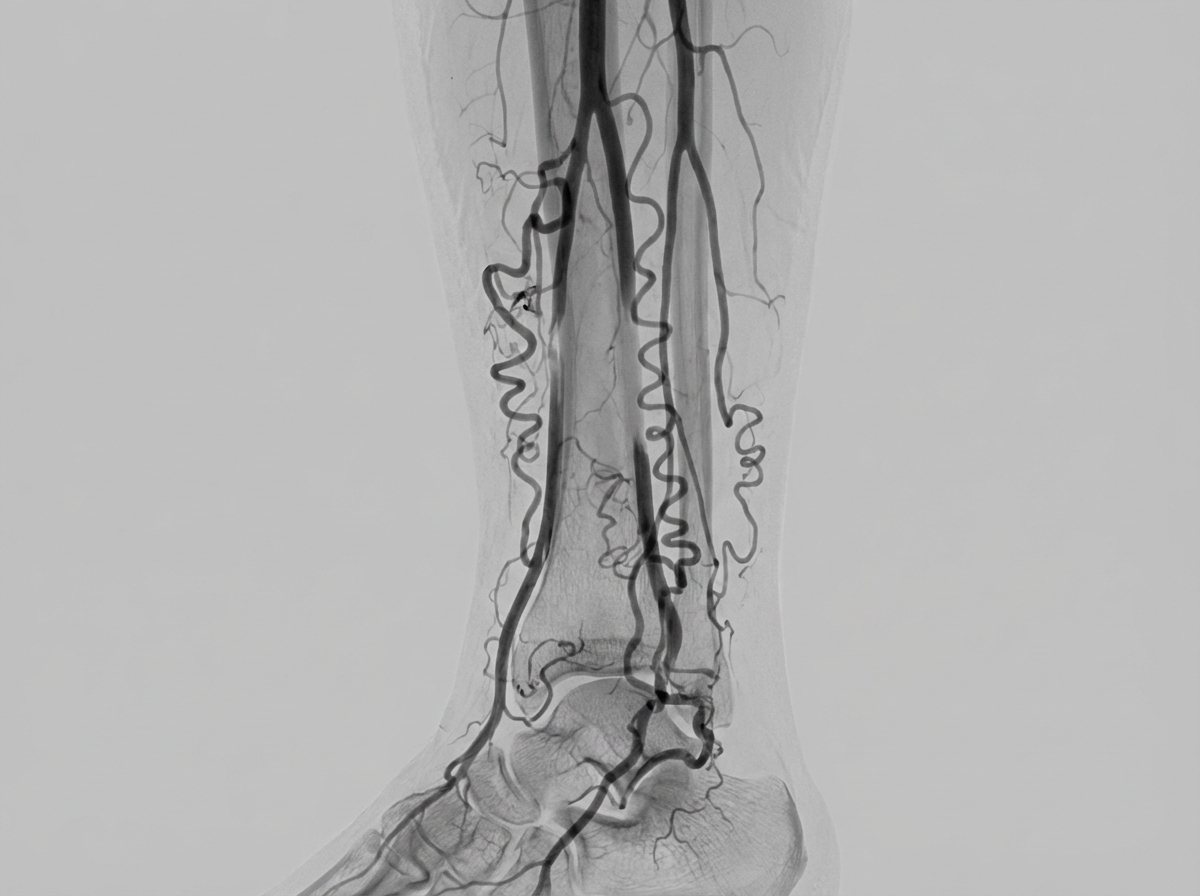
The most common radiographic appearance of an Odontogenic Keratocyst (OKC) is:
Which of the following processing methods is/are used in radiology?
What is the best initial diagnostic test for achalasia cardiae?
Barium meal contrast radiography is better than endoscopy for diagnosing which of the following conditions?
Which anatomical structures can be visualized on a Caldwell view (occipito-frontal) radiograph?
Posterior indentation on a barium swallow study is typically caused by which structure?
What is the recommended pH range for an acidifier used in a fixer solution?
Slip ring technology is useful for which imaging modality?
Practice by Chapter
Iodinated Contrast Media
Practice Questions
MRI Contrast Agents
Practice Questions
Ultrasound Contrast Agents
Practice Questions
Adverse Reactions to Contrast Media
Practice Questions
Management of Contrast Reactions
Practice Questions
Contrast-Induced Nephropathy
Practice Questions
Barium Studies
Practice Questions
Intravenous Urography
Practice Questions
Angiography Techniques
Practice Questions
Lymphangiography
Practice Questions
Contrast Administration Protocols
Practice Questions
Pretesting and Premedication
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
