Contrast and Radiological Procedures — MCQs

On this page
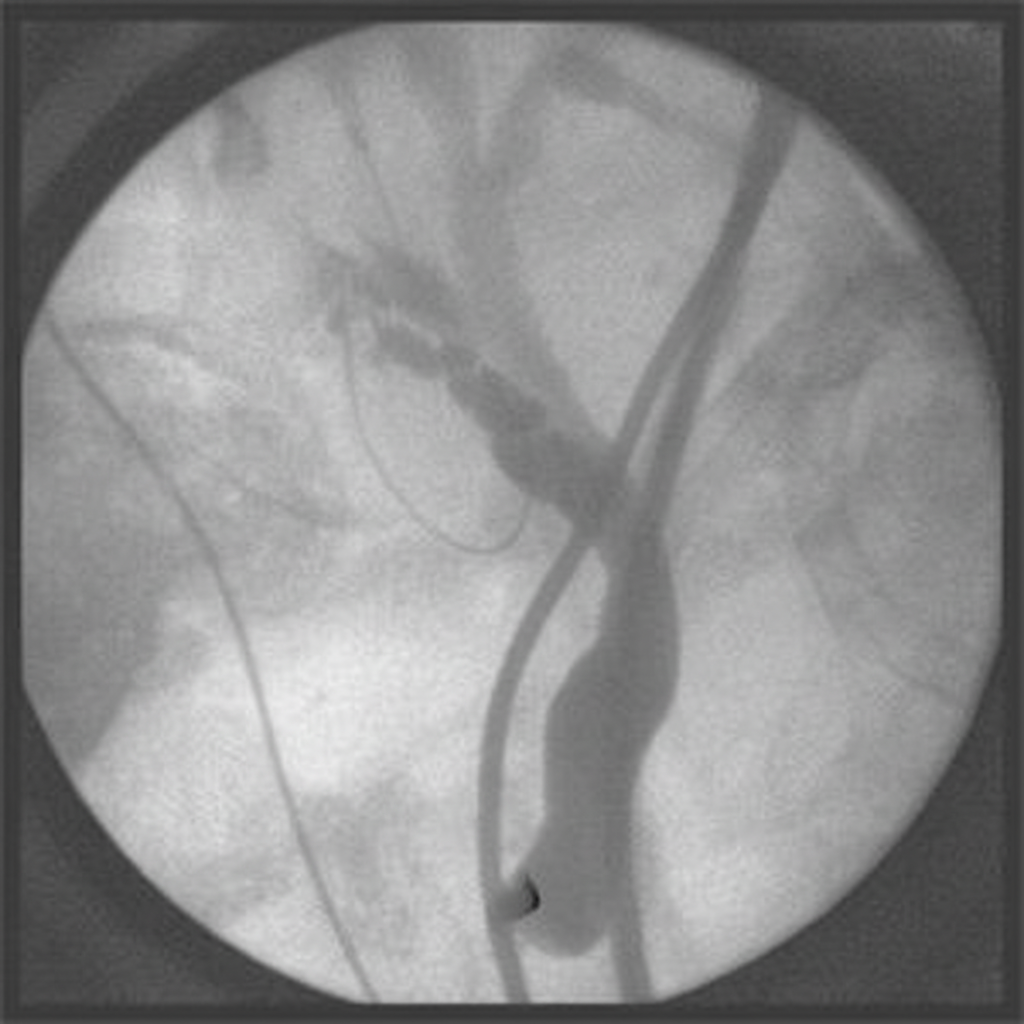
What is the most appropriate diagnostic finding in this scenario?
What is one advantage of digital radiography?
Which of the following is NOT a radiological feature of achalasia cardia?
On barium swallow, what characteristic appearance is shown by a leiomyoma?
Which of the following is NOT a radiological evidence of Achalasia Cardia?
On which day of a normal 28-day menstrual cycle should a hysterosalpingogram be performed for a woman with a 5-day menstrual period?
Who is credited with developing cerebral angiography?
What contrast agent is typically used for Magnetic Resonance Imaging (MRI)?
What contrast agent is used in a barium enema?
What contrast agent is used for MRI?
Practice by Chapter
Iodinated Contrast Media
Practice Questions
MRI Contrast Agents
Practice Questions
Ultrasound Contrast Agents
Practice Questions
Adverse Reactions to Contrast Media
Practice Questions
Management of Contrast Reactions
Practice Questions
Contrast-Induced Nephropathy
Practice Questions
Barium Studies
Practice Questions
Intravenous Urography
Practice Questions
Angiography Techniques
Practice Questions
Lymphangiography
Practice Questions
Contrast Administration Protocols
Practice Questions
Pretesting and Premedication
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
