Contrast and Radiological Procedures — MCQs

On this page
What is the primary use of a probe in a medical context?
Light radiographic film is due to what processing error?
What is the most serious complication of myelography?
Which of the following is the most specific and sensitive screening test for renovascular hypertension?
Intravenous pyelogram (IVP) should be cautiously performed in which of the following conditions?
Cervical burnout is a phenomenon caused by?
Which element is the basis for contrast agents commonly used in CT scans?
The string sign of Kantor is seen in which condition?
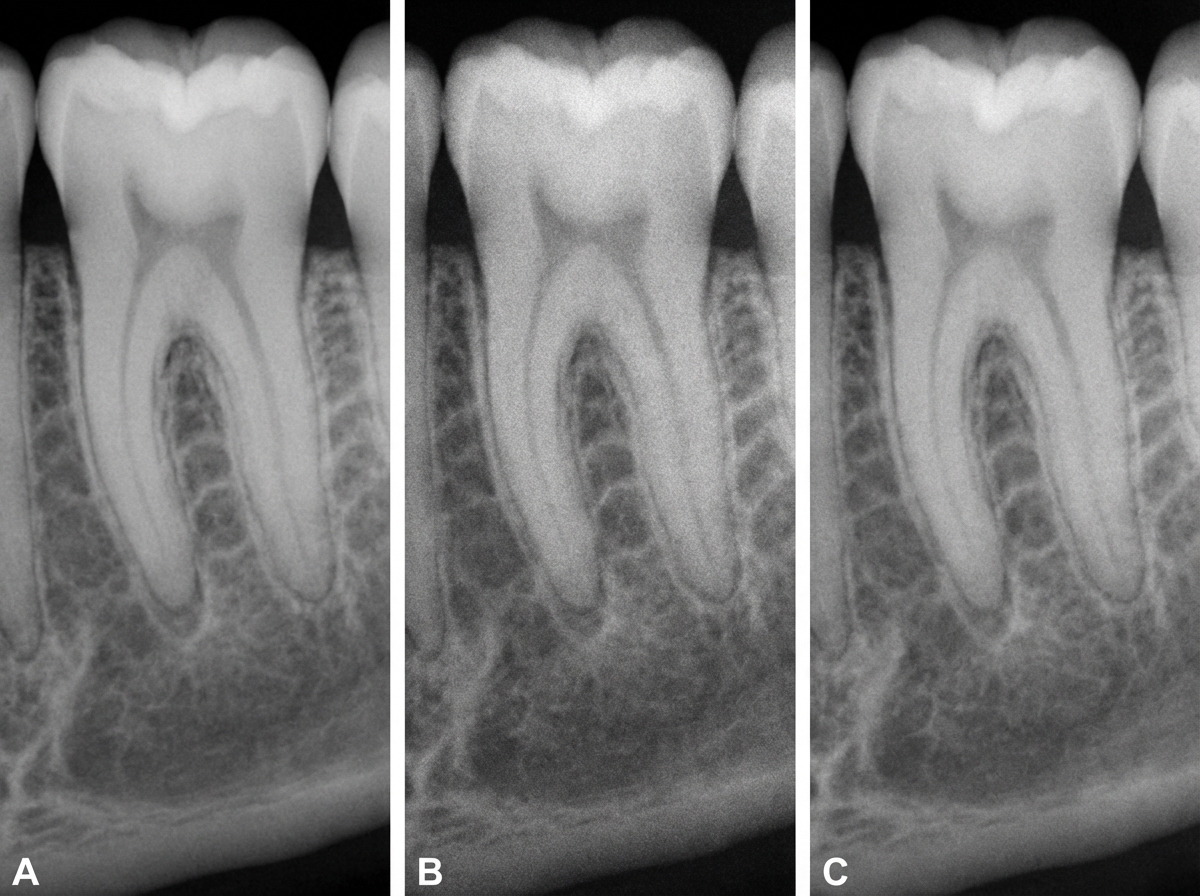
Three radiographs of the same tooth were taken using a digital intra-oral X-ray system, an intensifying screen/film cassette combination, and conventional dental film (F speed). Which of the following X-rays was taken with conventional dental film?
A 16-film radiographic survey consists of the 12-film survey and the addition of which of the following?
Practice by Chapter
Iodinated Contrast Media
Practice Questions
MRI Contrast Agents
Practice Questions
Ultrasound Contrast Agents
Practice Questions
Adverse Reactions to Contrast Media
Practice Questions
Management of Contrast Reactions
Practice Questions
Contrast-Induced Nephropathy
Practice Questions
Barium Studies
Practice Questions
Intravenous Urography
Practice Questions
Angiography Techniques
Practice Questions
Lymphangiography
Practice Questions
Contrast Administration Protocols
Practice Questions
Pretesting and Premedication
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
