Contrast and Radiological Procedures — MCQs

On this page
Identify the radiological procedure shown in the image?
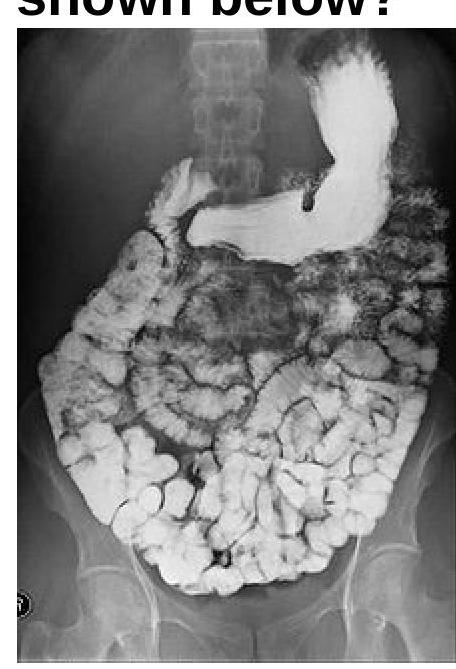
The Barium Swallow examination shows a mass in the esophagus. What can be the most probable diagnosis?
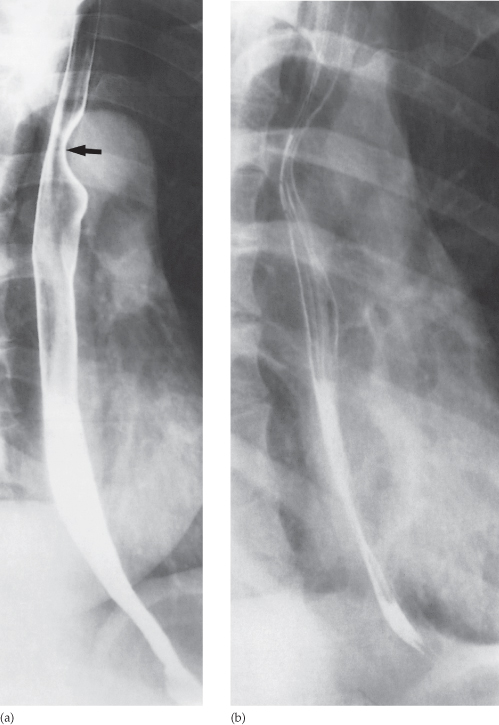
Which of the following imaging techniques is NOT typically used for diagnosing uterine anomalies?
What is the structure seen in the X-ray?
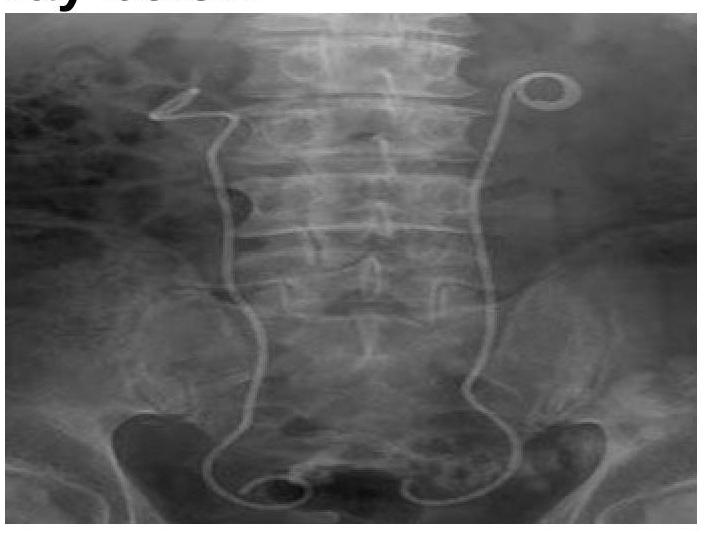
What does the following radiograph from a double contrast esophagram represent?
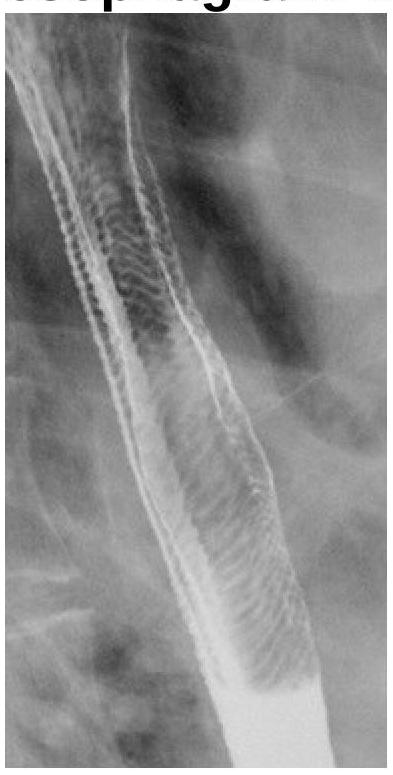
Which of the following is not considered a contraindication for undergoing an MRI?
What is an X-ray artifact?
What is the investigation of choice for whole body imaging in metastatic breast cancer?
Barium swallow is used for -
The procedure of choice for the evaluation of aortic aneurysms is -
Practice by Chapter
Iodinated Contrast Media
Practice Questions
MRI Contrast Agents
Practice Questions
Ultrasound Contrast Agents
Practice Questions
Adverse Reactions to Contrast Media
Practice Questions
Management of Contrast Reactions
Practice Questions
Contrast-Induced Nephropathy
Practice Questions
Barium Studies
Practice Questions
Intravenous Urography
Practice Questions
Angiography Techniques
Practice Questions
Lymphangiography
Practice Questions
Contrast Administration Protocols
Practice Questions
Pretesting and Premedication
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
