Intravenous Urography — MCQs

Which of the following contrast agents is PREFERRED in a patient with renal dysfunction for the prevention of contrast-induced nephropathy?
The most sensitive imaging modality to detect early renal tuberculosis is:
What is the investigation of choice in a patient with blunt abdominal trauma with hematuria?
A patient presents with acute renal failure (ARF) and complete anuria, with a normal ultrasound of the kidneys. Which investigation will provide the best initial information regarding renal function?
A dense nephrogram is obtained by
Which of the following statements about contrast in radiography is true:
A one-year-old male child presented with a poor urinary stream since birth. The initial investigation of choice for evaluation is:
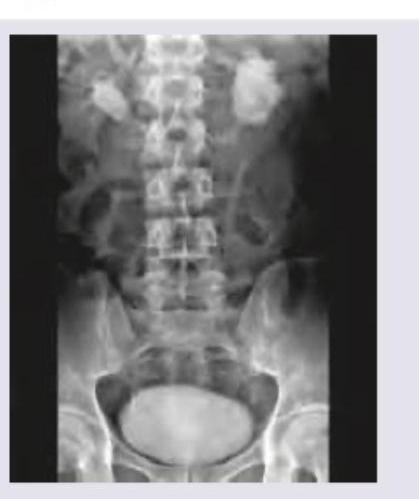
The following IVU shows:
What is the investigation of choice in a patient with blunt abdominal trauma with hematuria?
A dense persistent nephrogram may be seen in all of the following except:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
