Chest Radiology — MCQs

On this page
A 20-year-old young man presents with exertional dyspnea, headache, and giddiness. On examination, there is hypertension and LVH. X-ray chest shows notching of the anterior ends of the ribs. Which of the following represents the most likely diagnosis?
Left Pleural effusion is detected best in which position?
A single retrocardiac air-fluid level on a chest radiograph typically implies the presence of what?
Kerley B lines in a chest X-ray are a radiological feature of which of the following conditions?
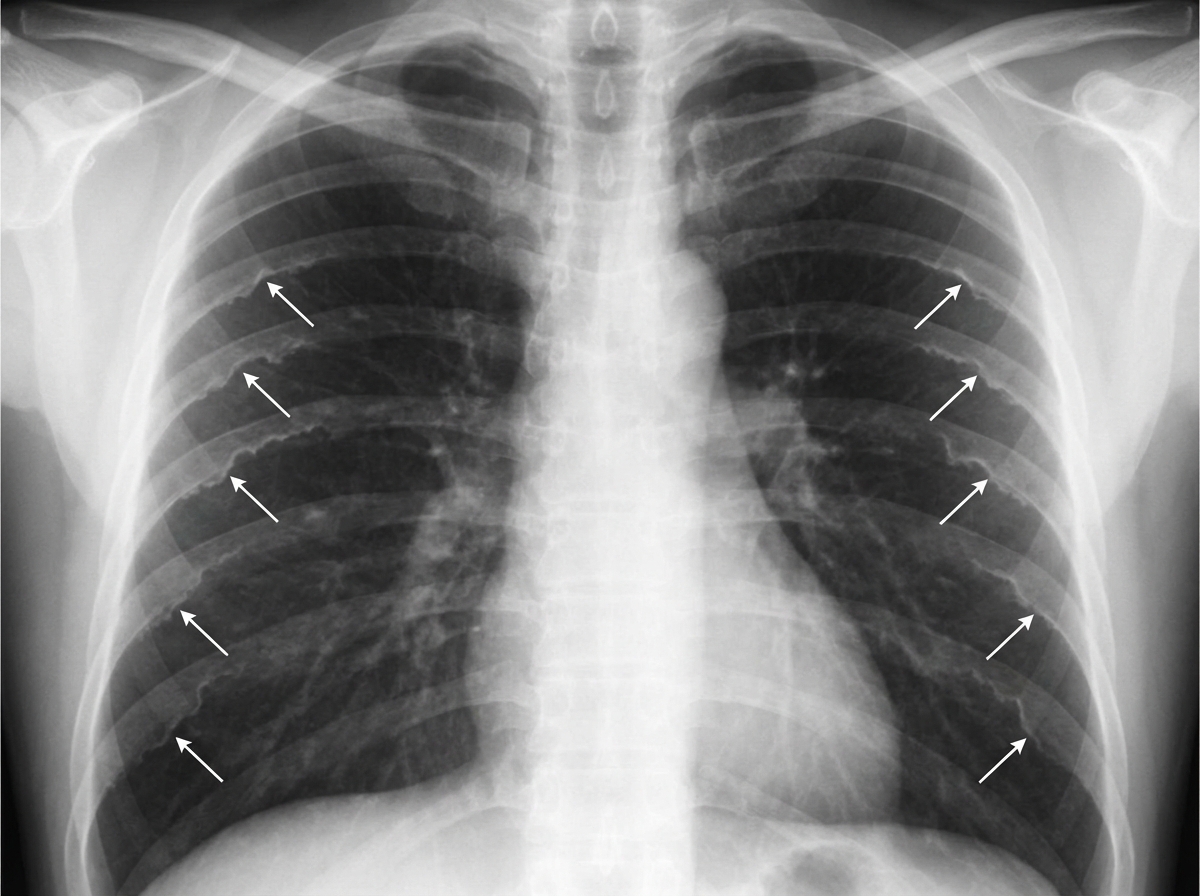
The sign marked by the arrows pointing to the ribs, in the provided chest X-ray, is diagnostic of which of the following conditions?
A 'tear drop heart' is seen in which of the following conditions?
The bone algorithm is used as a principle in which of the following modalities?
Hilar lymph nodes showing eggshell calcification are seen in all of the following EXCEPT?
Hilar markings in a normal chest X-ray are formed by all of the following except:
What is the best method for detecting minimal bronchiectasis?
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
