Chest Radiology — MCQs

On this page
Rib notching is typically found in which of the following conditions?
Which of the following does NOT cause a homogenous opacity on X-ray?
What is the name of the sign that shows eggshell calcification?
What is the best view for the tracheo-esophageal groove?
A 22-year-old woman has experienced increasing dyspnea for the past 2 months. On physical examination, she is afebrile and normotensive. Inspiratory wheezes are noted on auscultation of the chest. A chest CT scan shows an 8x10 cm posterior mediastinal mass that impinges on the trachea and esophagus. A mediastinoscopy is performed, and a biopsy of the mass microscopically shows scattered large multinucleated cells, with prominent nucleoli that mark with CD15, and lymphocytes and macrophages separated by dense collagenous bands. Which of the following cells is most likely to be seen microscopically in this biopsy specimen?
A 45-year-old man presents with a 3-day history of breathlessness, fever, and dry cough. He recently traveled to China. Nasal and throat swabs have been collected, and a chest CT scan has been performed. Which of the following CT chest findings is most likely to be observed in this patient?
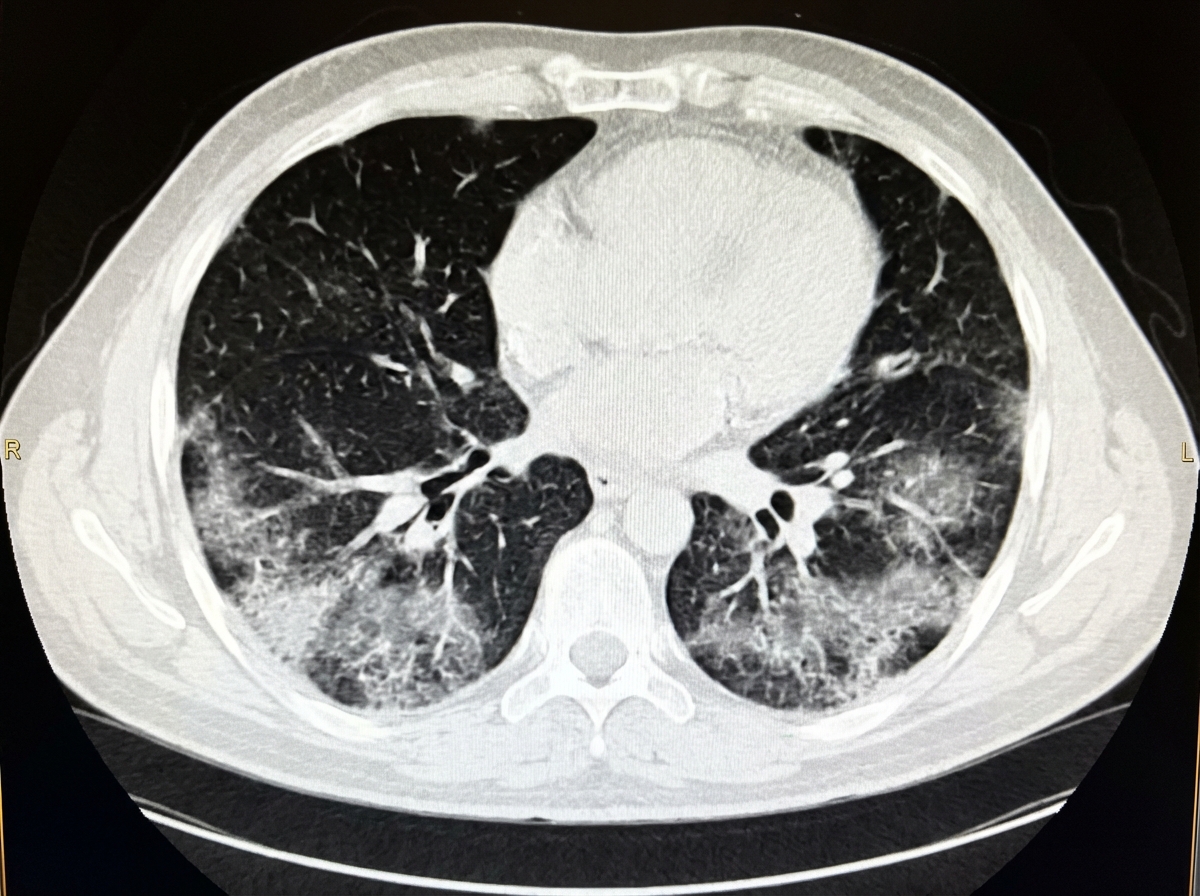
A cruise ship passenger who is a known smoker presents with fever, cough, and shortness of breath for the last 4 days. What do the provided CT chest findings suggest?
Which of the following is NOT a differential diagnosis for a middle mediastinal mass?
All of the following are true regarding bronchial cysts, EXCEPT:
Hampton hump is a characteristic finding in which of the following conditions?
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
