Chest Radiology — MCQs

On this page
CXR was done for a 15-year-old boy with low cardiac output. Which is incorrect about the patient?
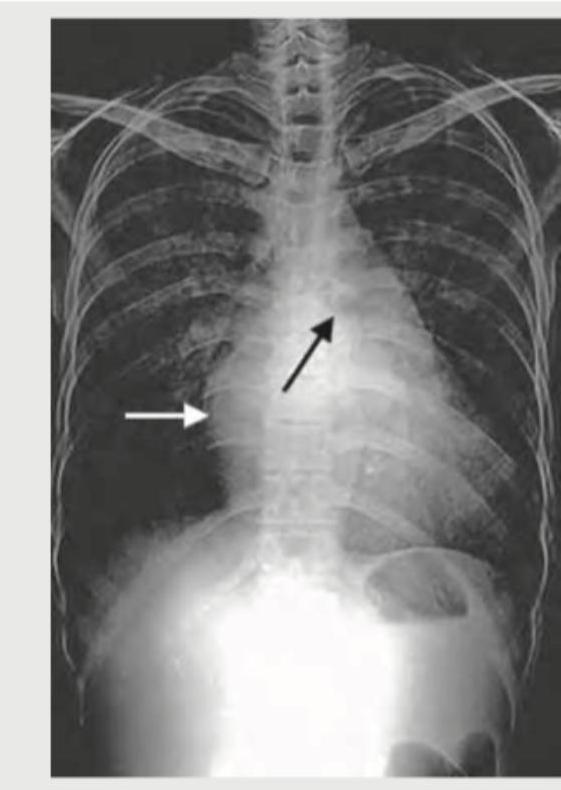
An adult undergoes multiple FFP transfusions for excessive bleeding after cardiac surgery and develops respiratory distress. CXR done is shown below. What does it indicate?
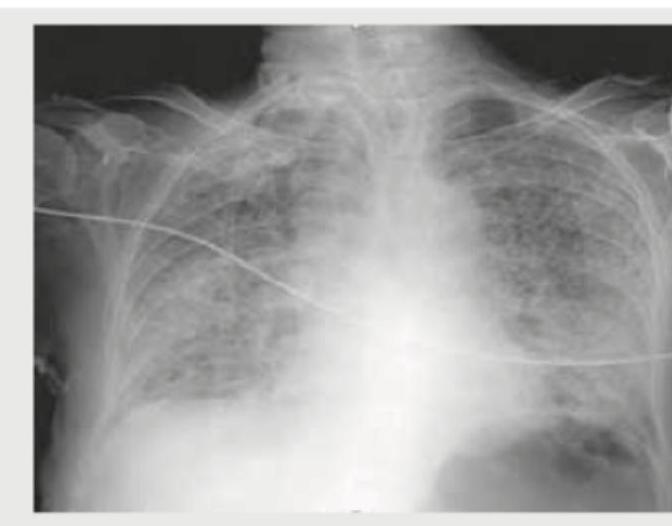
What is the diagnosis based on the CXR of a patient of cystic fibrosis shown below?
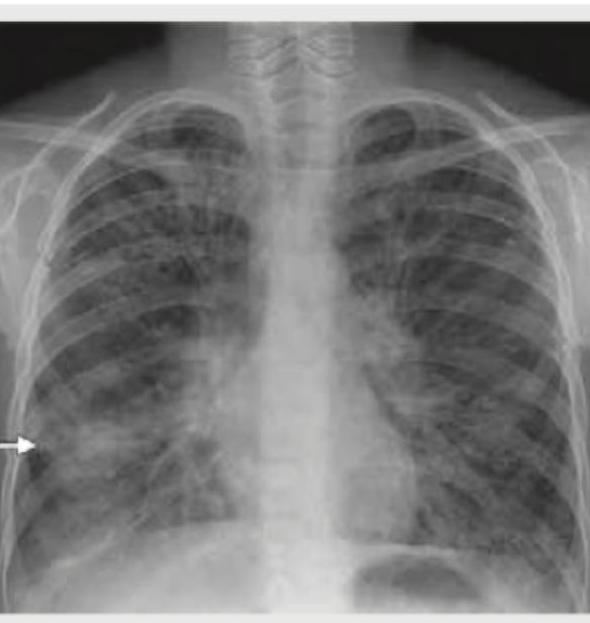
A chest X-ray shows the following appearance. Identify the pathology:
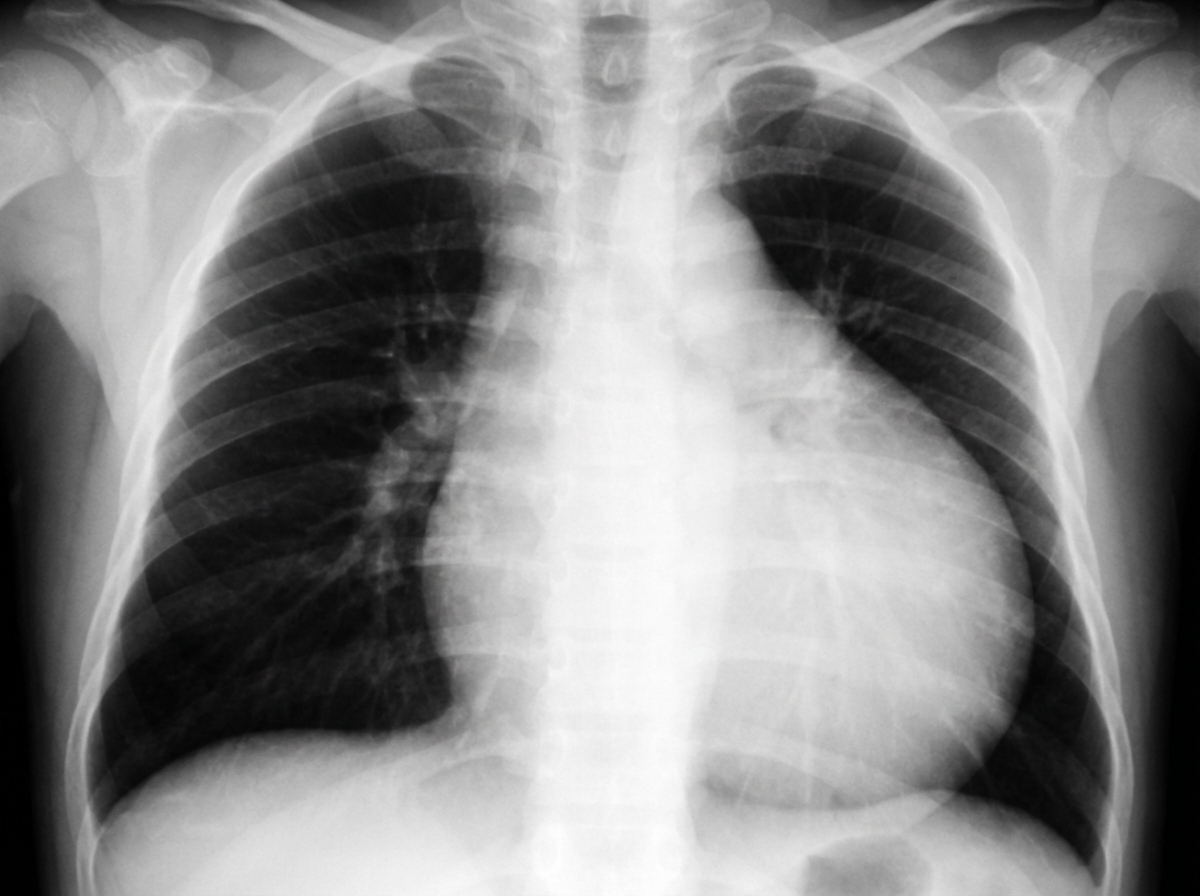
A 40-year-old male presents with sudden onset right-sided chest pain and breathlessness following a road traffic accident. On examination, breath sounds are diminished on the right side. The chest X-ray is shown below. What is the most likely diagnosis?
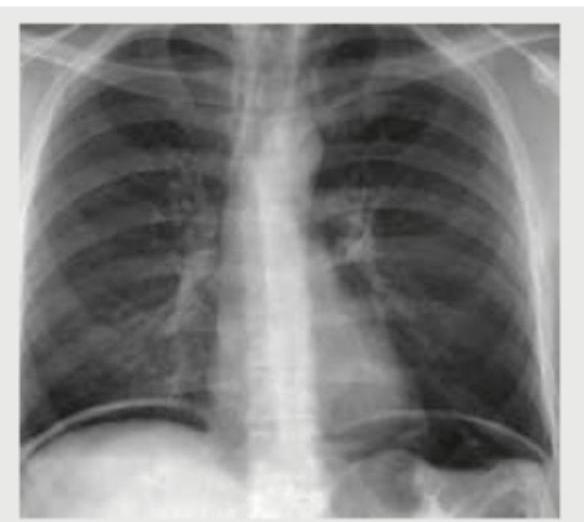
Which is not a finding of the Chest X-ray shown below? (AIIMS May 2017)
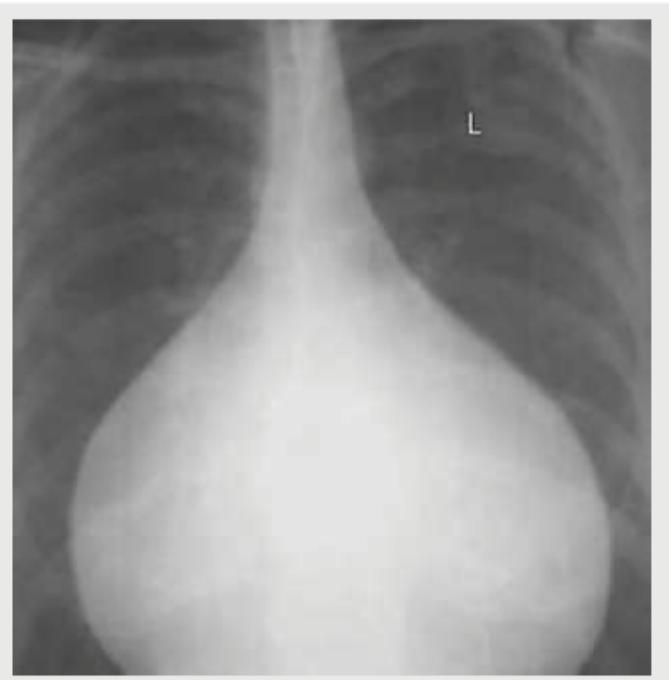
A previously healthy patient, presents with dyspnea and low grade fever since 4 months. His lungs are clear. JVP is normal. ECG showed low voltage complexes. What is the possible diagnosis?
Comment on the diagnosis of the image shown below.
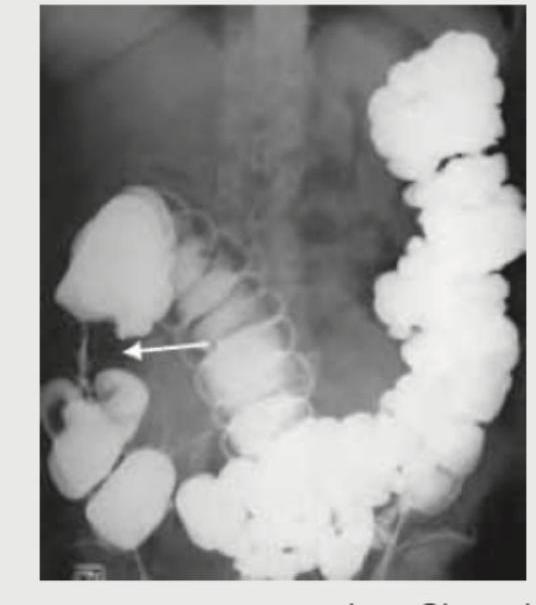
On a chest radiograph, which of the following occupational diseases is most likely to be mistaken as a case of tuberculosis of lungs?
Which of the following are included in common causes of mediastinal masses in superior and anterior mediastinum? I. Goitre II. Thymic tumour III. Neurogenic tumour Select the correct answer using the code given below :
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
