Chest Radiology — MCQs

On this page
A patient presented with sudden onset difficulty in breathing with RR 28/min, normal blood pressure. X-ray was taken which is given below. What is the diagnosis?
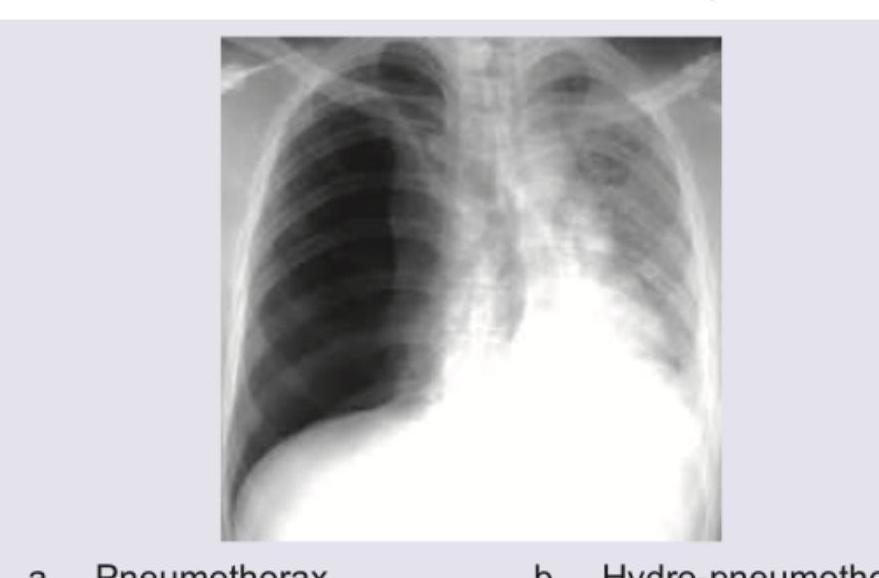
Curve A signifies which of the following?
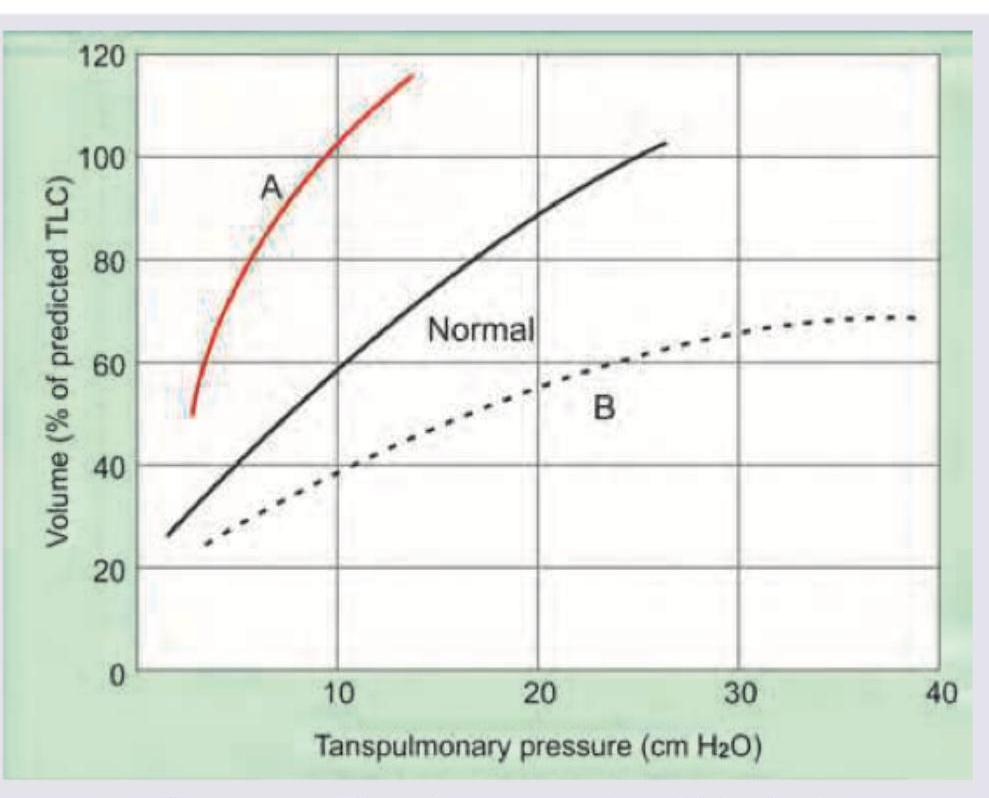
What is indicated by the 'water bottle appearance' of the heart size?
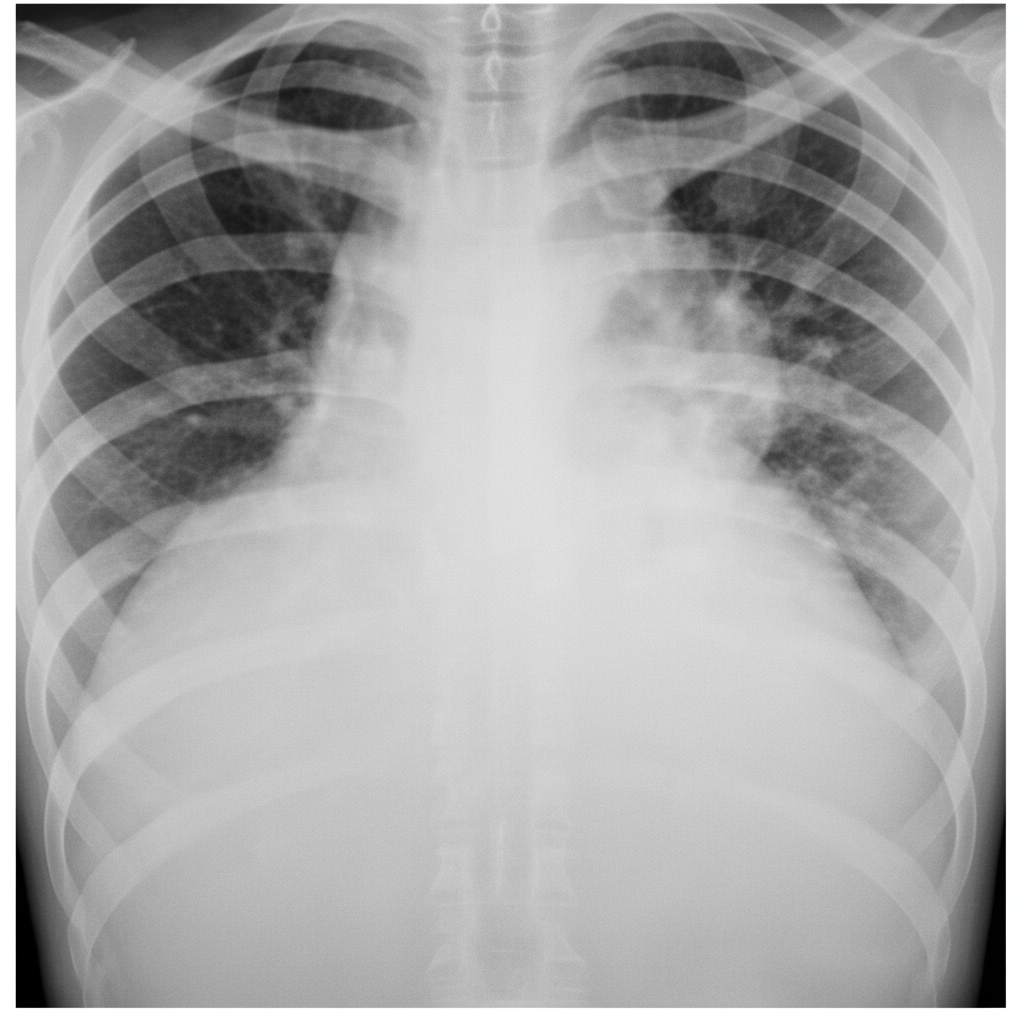
What does the CXR of a patient with cystic fibrosis show?
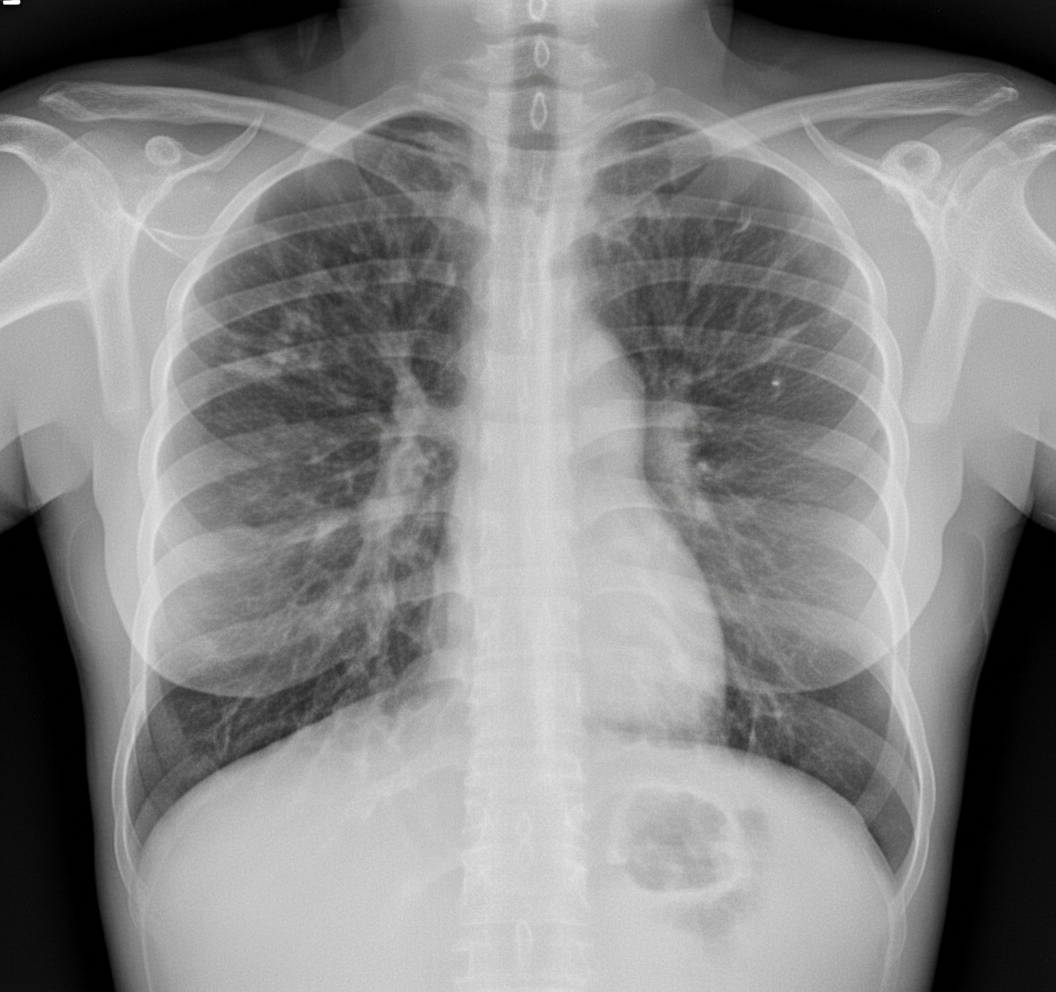
What does this CT chest image show?
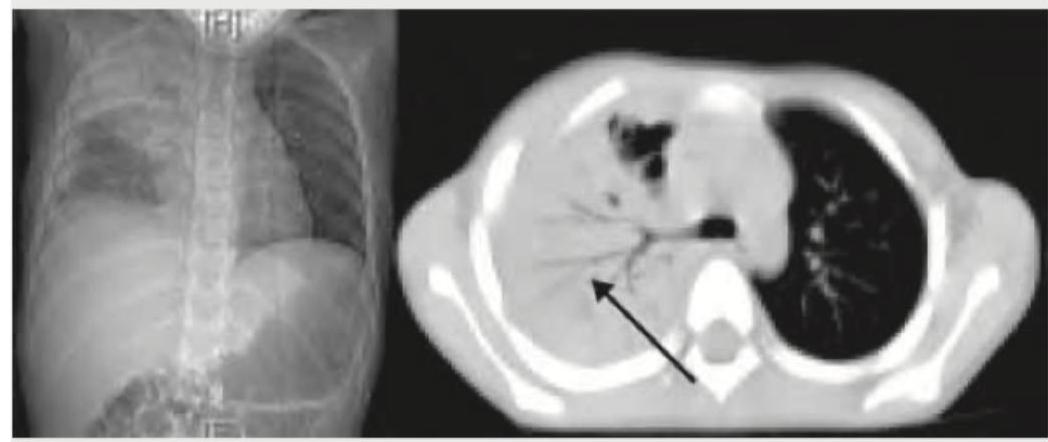
The given contrast enhanced CT scan chest shows presence of:
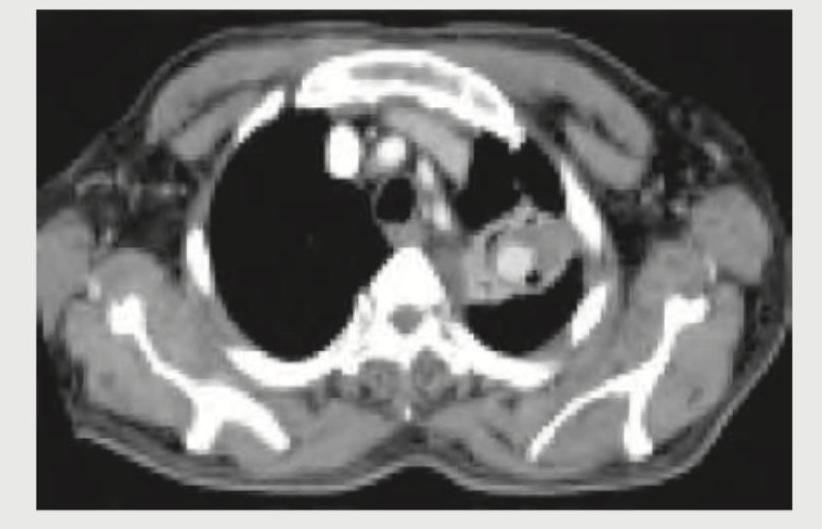
A 30-year-old nephrotic syndrome patient travelled via a non-stop flight from San Francisco to New Delhi. On arrival at the destination, the patient started having difficulty in breathing and was rushed to the hospital. His $\mathrm{SpO}_{2}$ is $85\%$ and ECG shows sinus tachycardia with T wave inversion in lead III. CT chest was performed. What is the diagnosis?
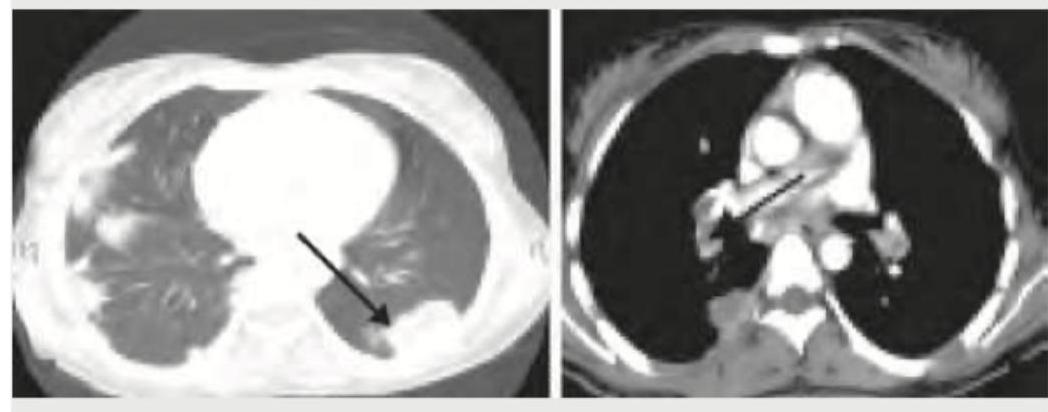
A cement slab fell on the chest of a 20-year-old construction worker. His condition deteriorated over the next 24 hours after admission. A repeat CT chest was performed. What does it show?
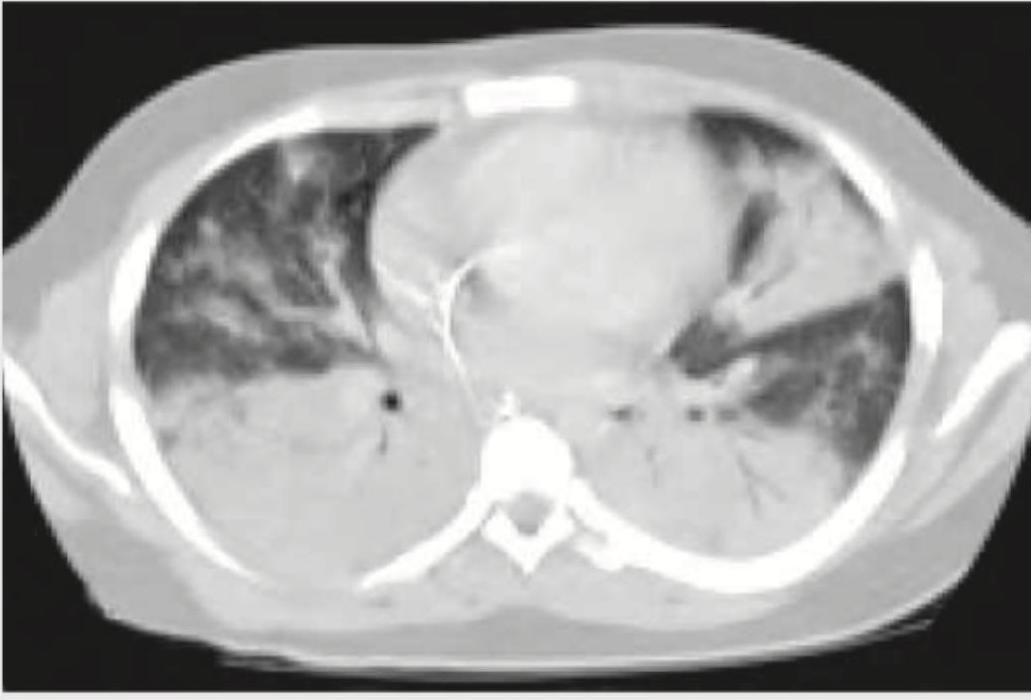
A cement slab fell on the chest of a 20-year-old construction worker. The arrow in the given CT chest points to:
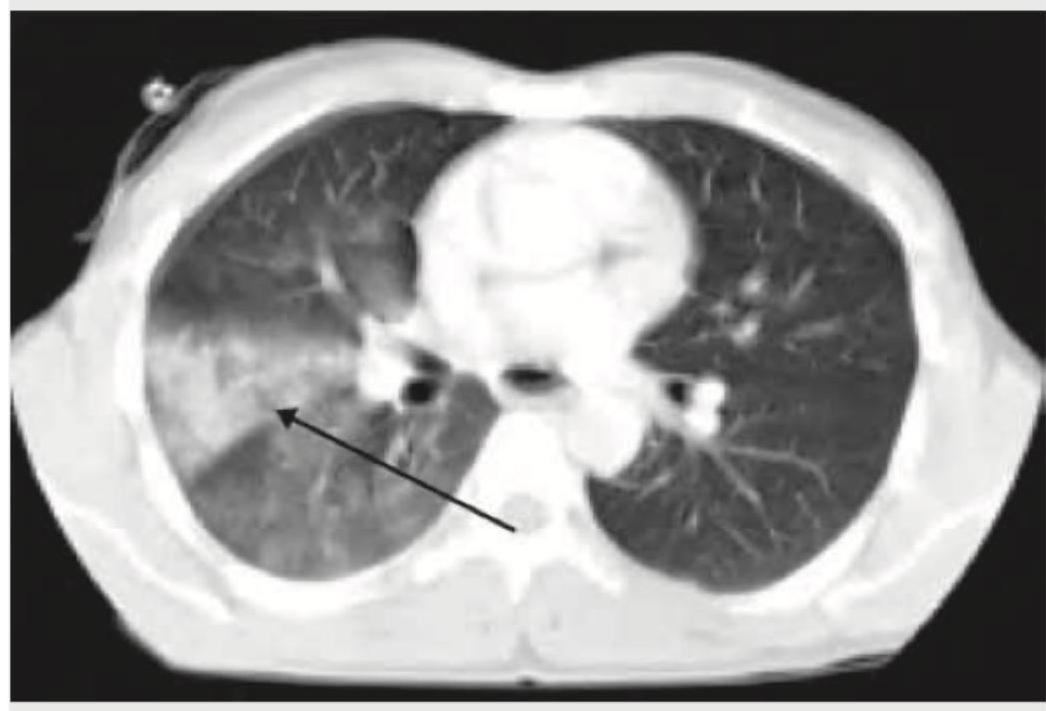
The arrow in the given CT chest points to:
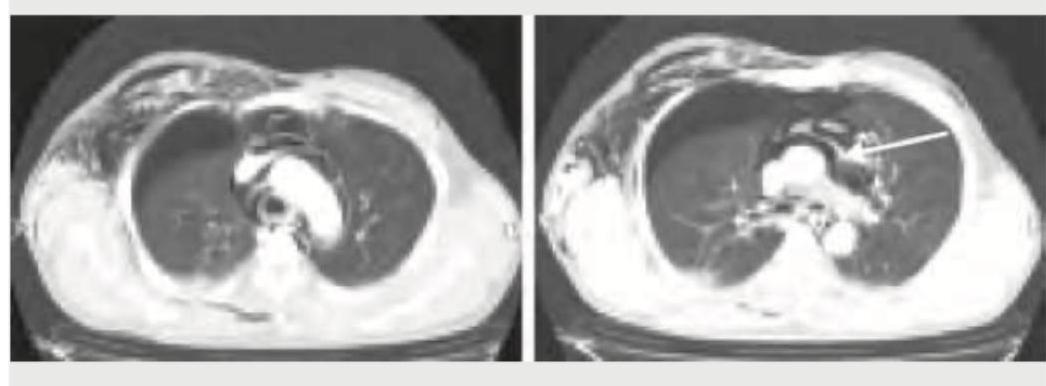
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
