Chest Radiology — MCQs

On this page
Ground-glass appearance on HRCT is seen in which of the following conditions?
Which of the following is the earliest radiological sign of acute respiratory distress syndrome (ARDS) on chest X-ray?
A 65-year-old male smoker presents with hemoptysis and weight loss. Chest X-ray shows a central hilar mass with mediastinal widening. Which imaging modality is most appropriate for staging the extent of disease?
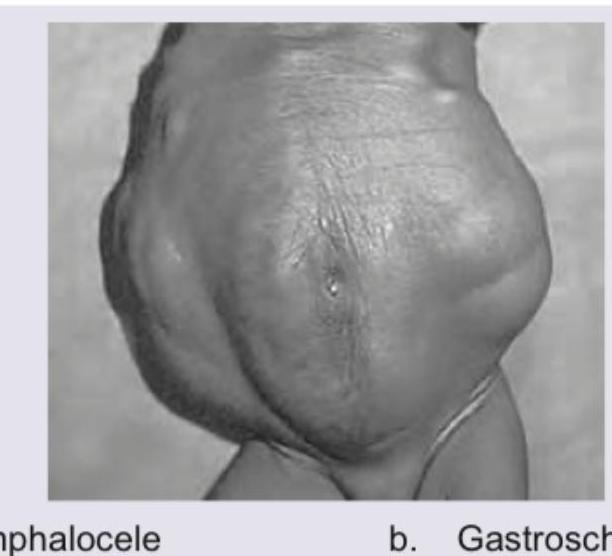
What is the most probable diagnosis based on the image provided?
In croup, the characteristic radiographic finding of subglottic narrowing on a frontal chest X-ray creates a tapering appearance of the upper trachea. This diagnostic sign is commonly referred to as which of the following?

The following X-ray shows:
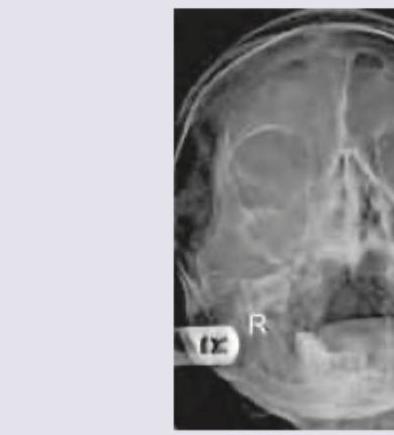
The CT chest shows presence of:
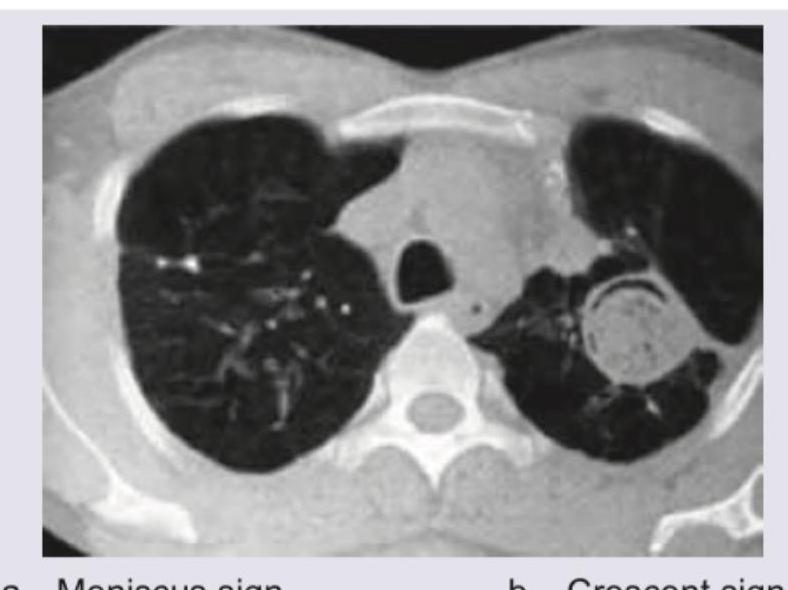
A 35-year-old female presents with a large thyroid swelling. Her chest X-ray is shown below. What is the most likely diagnosis?
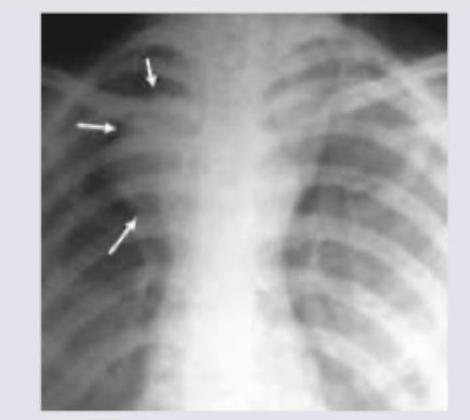
The chest X-ray of a cystic fibrosis patient shows presence of:
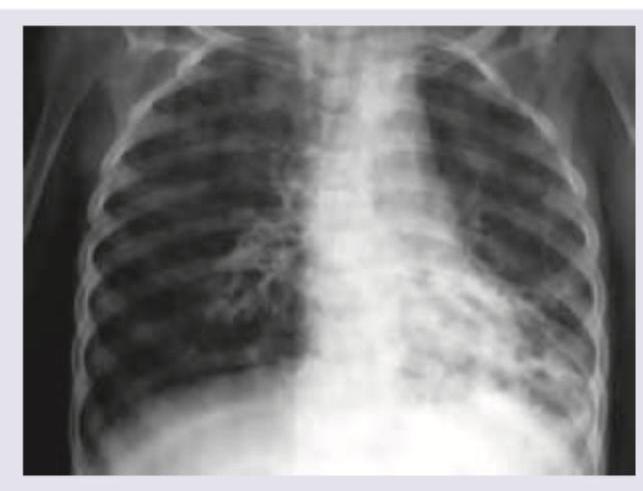
Identify this condition?
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
