Chest Radiology — MCQs

On this page
The following chest X-ray findings are all suggestive of malignancy except?
A 65-year-old man developed severe, acute onset breathlessness within a few hours of aortic valve replacement. What is the likely diagnosis based on a chest X-ray?
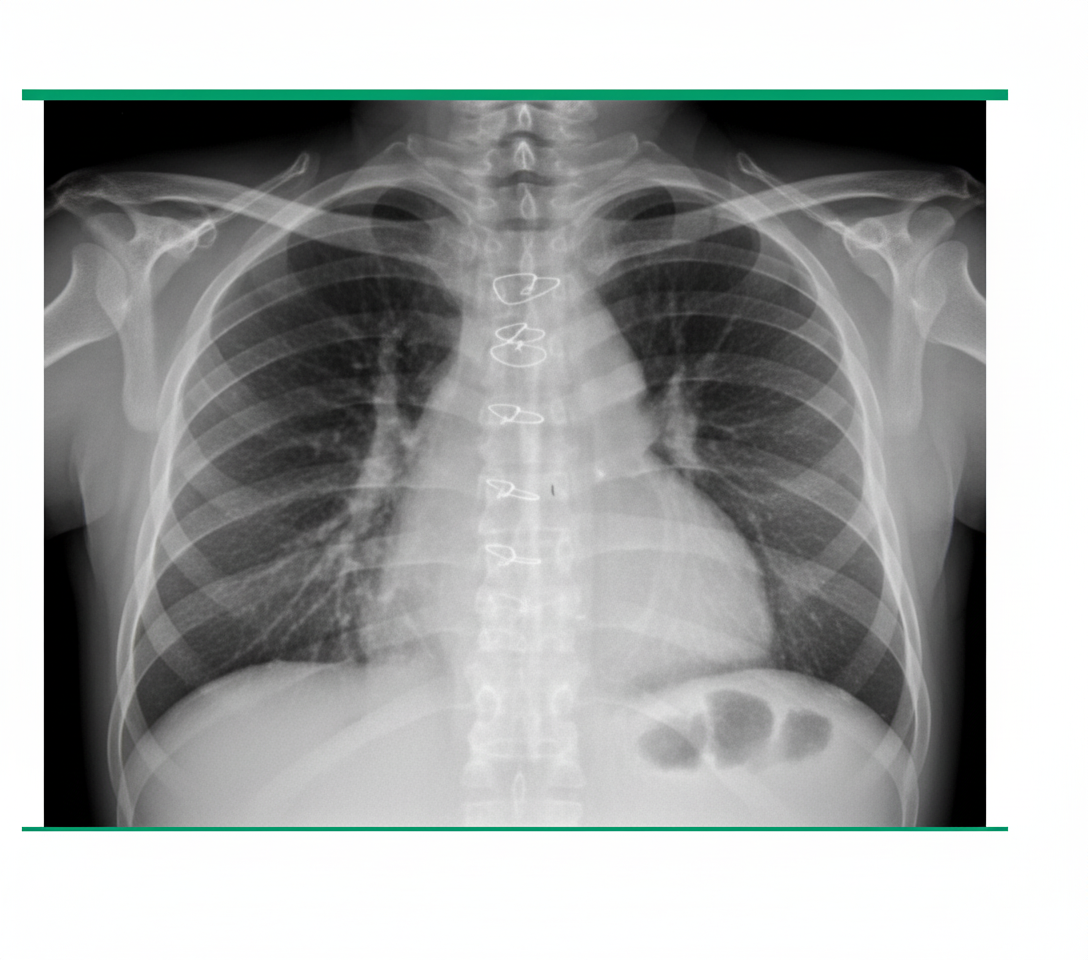
The signet ring sign is typically seen in which of the following conditions?
Miliary mottling is typically found in which of the following conditions?
In coarctation of the aorta, at which aspect of the rib is notching typically observed?
The tube visible in the chest X-ray below is located in which anatomical space?
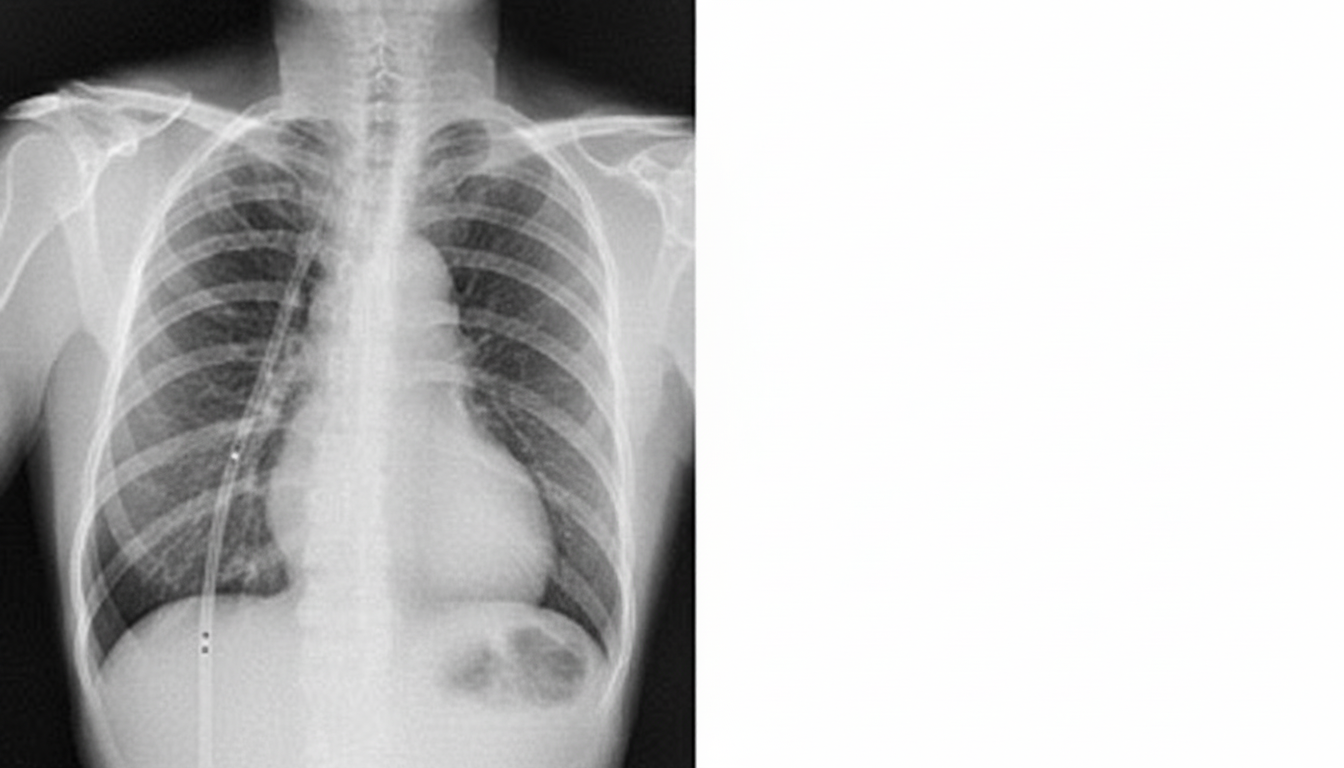
A 53-year-old female nonsmoker is being evaluated with symptoms of progressive shortness of breath. She has a past history of trauma to the right side of the chest. There is no history of asthma, sputum production, or recent chest pain. Chest X-ray is shown. What is the likely diagnosis?
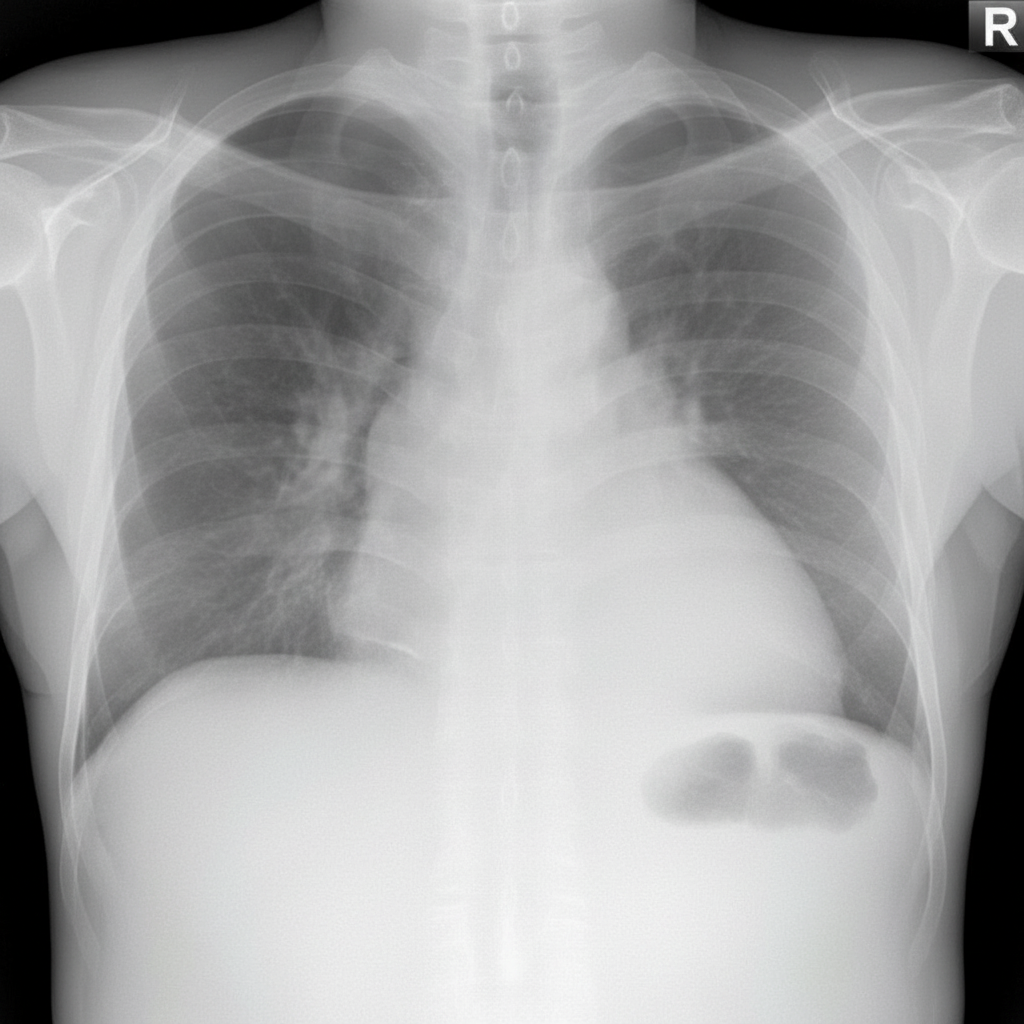
In a right-sided hemithorax on chest X-ray PA view, what can be excluded?
Steeple sign is seen in which of the following conditions?
HRCT is the investigation of choice for diagnosing all of the following conditions, EXCEPT?
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
