Chest Radiology — MCQs

On this page
The Hilar Dance Sign is characteristically seen in which of the following cardiac conditions?
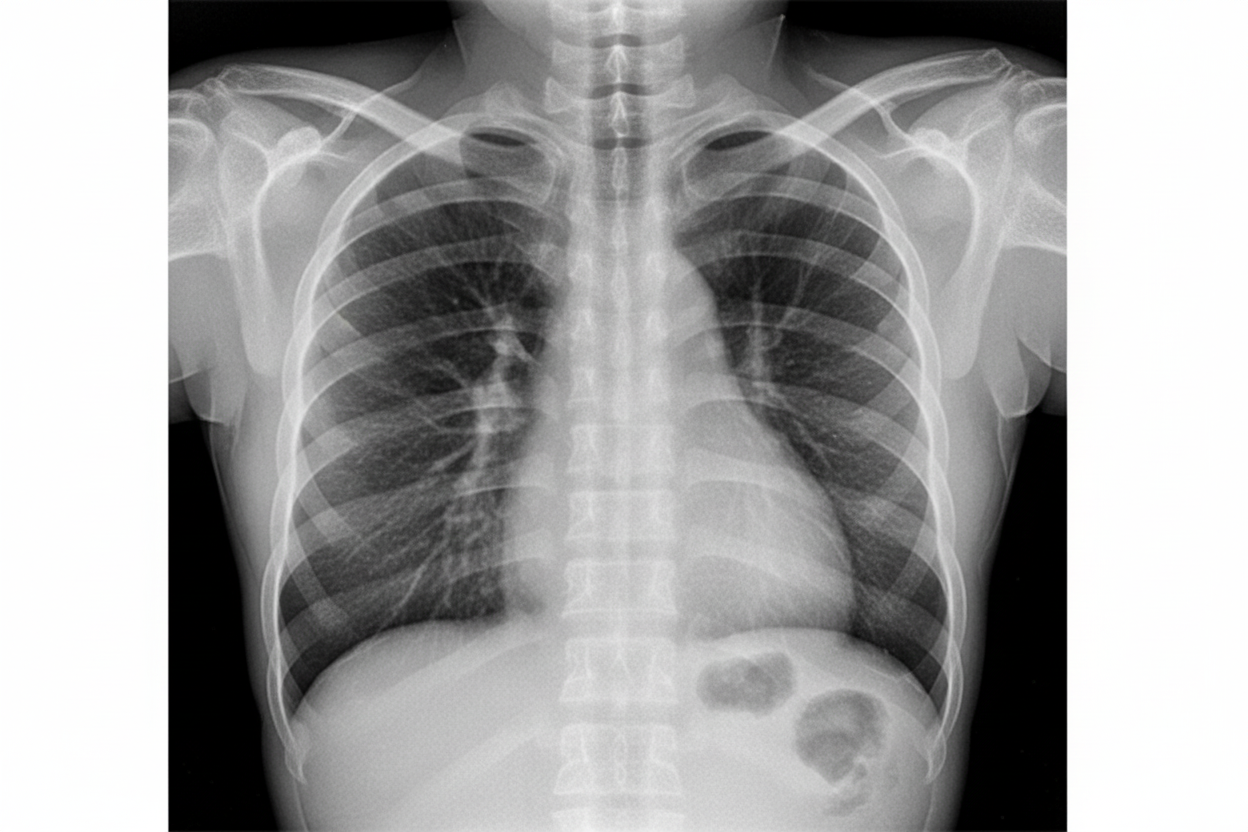
What is the likely diagnosis based on the provided chest X-ray?
Bilateral pleural thickening in the lower and middle lung zones is a radiological feature of which condition?
Which among the following is NOT a cause of calcification in an anterior mediastinal mass?
Which of the following features on X-ray chest can differentiate an Atrial Septal Defect (ASD) from a Ventricular Septal Defect (VSD)?
An X-ray film for closed pneumothorax should be taken during which of the following?
Which type of lung cancer resembles pneumonia with the air bronchogram sign?
Minimal pleural effusion is best detected by which X-ray view?
What are the X-ray features of sarcoidosis stage 2 according to the Scadding system?
What is the effective dose of a standard chest X-ray?
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
