Chest Radiology — MCQs

On this page
How can an atrial septal defect (ASD) be differentiated from a ventricular septal defect (VSD) on a chest X-ray?
How can an atrial septal defect (ASD) be differentiated from a ventricular septal defect (VSD) on a chest X-ray?
All of the following are indirect radiologic signs of lung collapse EXCEPT?
The following CT chest shows the presence of?
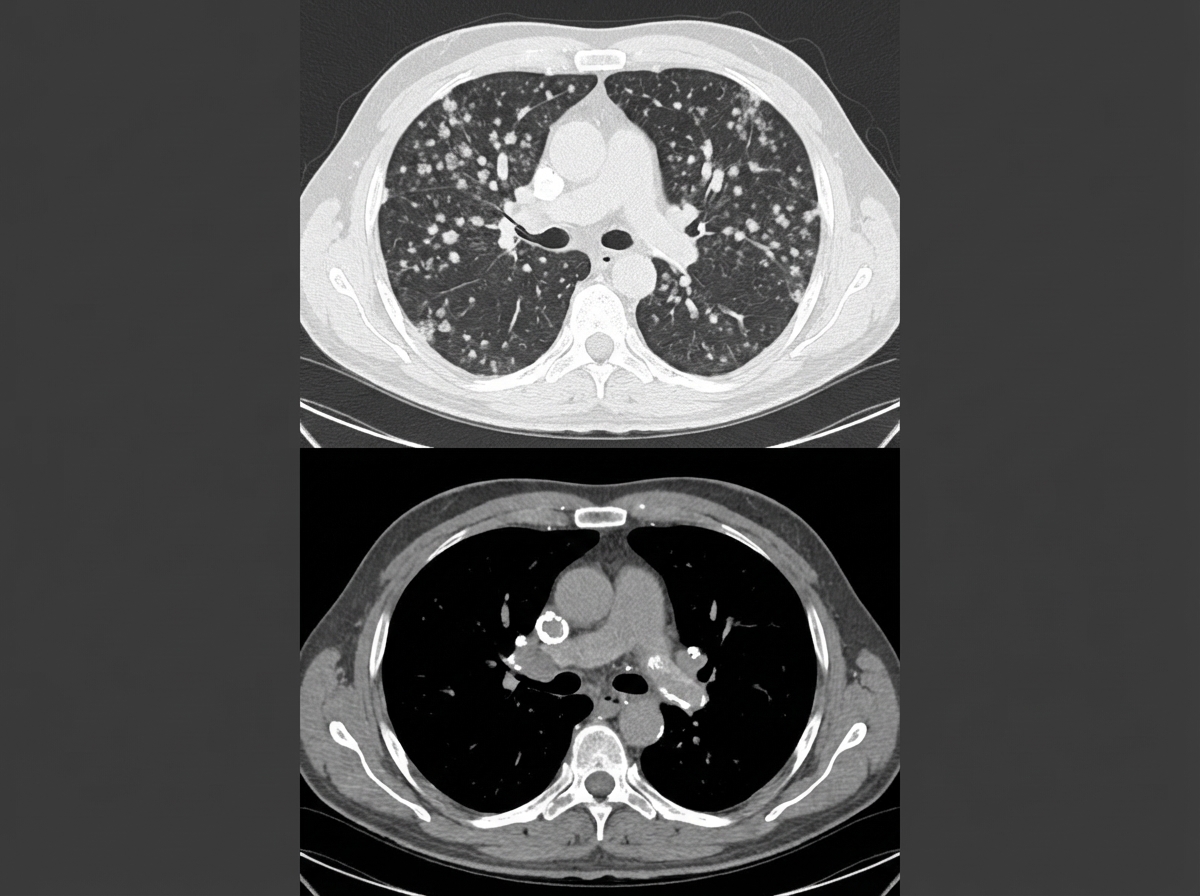
Atelectasis with reverse S sign is seen in which of the following conditions?
Perihilar fluffy opacities on chest X-ray are typically seen in which of the following conditions?
A right-sided pleural effusion is best visualized in which patient position?
Rib notching is seen in all except:
Which of the following features is characteristic of a benign lung lesion?
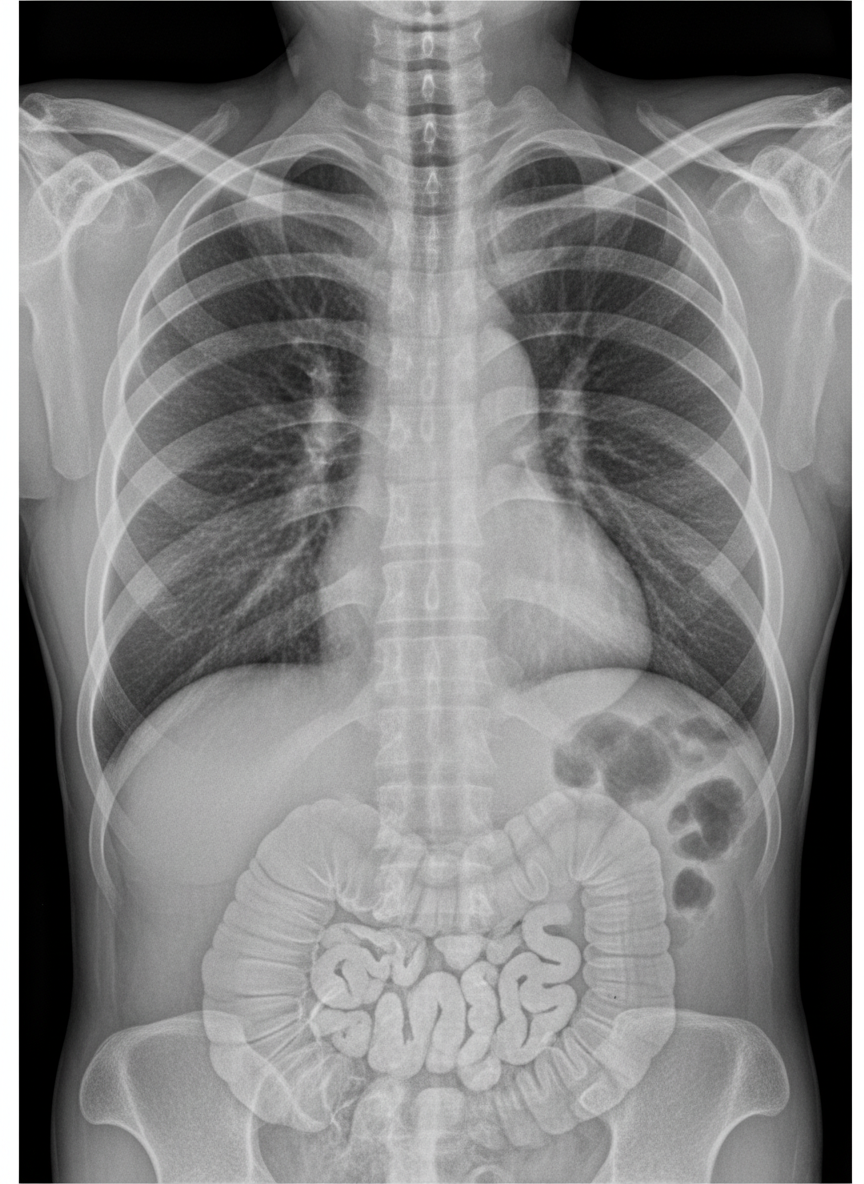
An X-ray shows findings suggestive of:
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
