Chest Radiology — MCQs

On this page
The chest X-ray shown is characteristic of which condition?
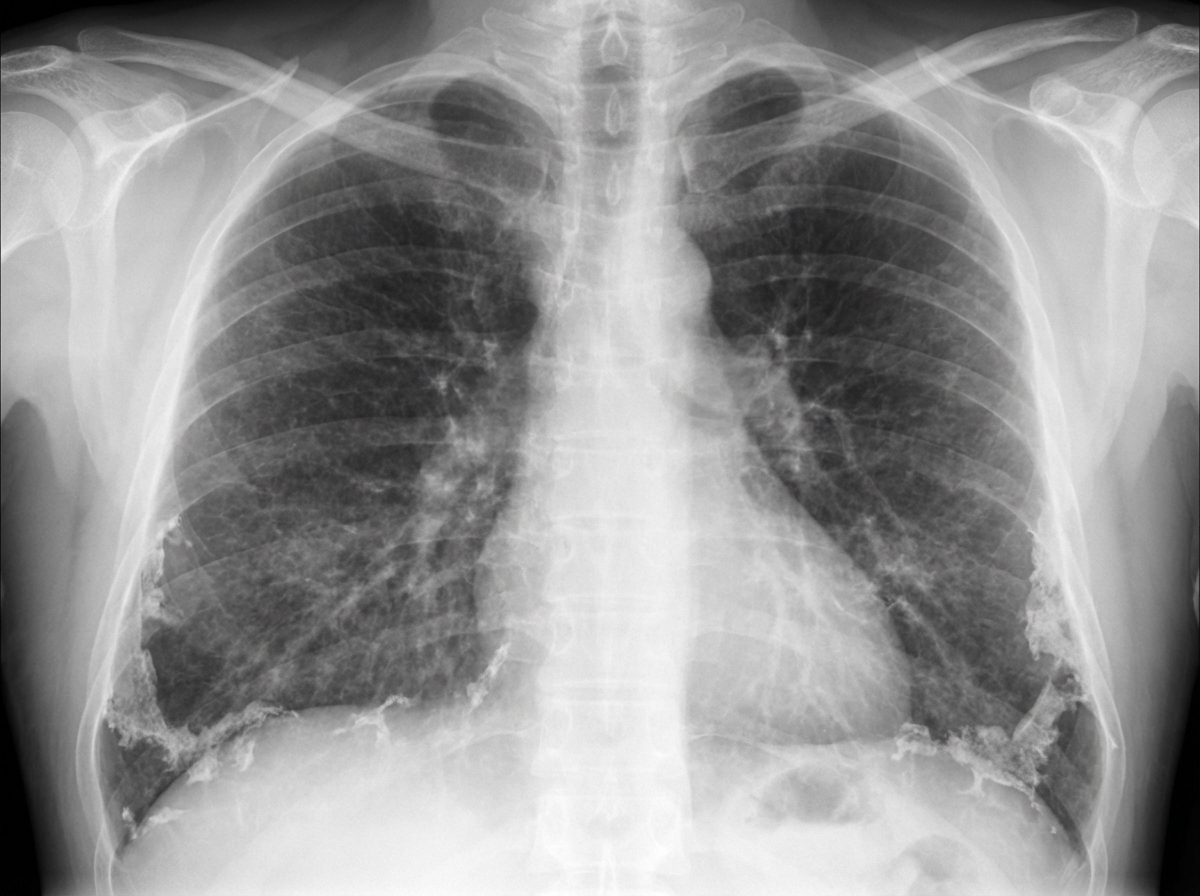
Which of the following is NOT a radiological feature of pulmonary edema?
All of the following can cause a miliary shadow on X-ray chest except?
The provided chest X-ray demonstrates findings suggestive of which of the following conditions?
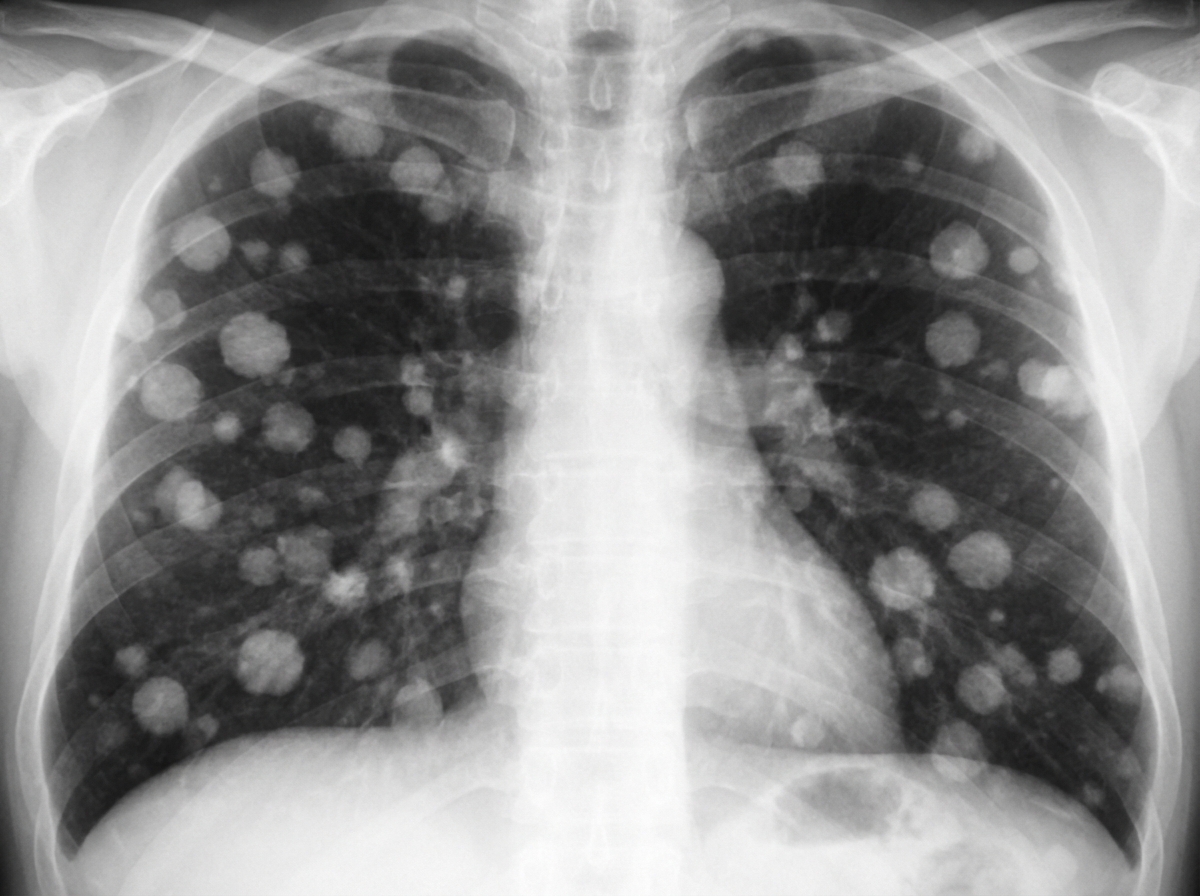
Popcorn calcification in the lung is characteristic of:
A lesion with sharp outlines extending above the clavicles suggests?
A CT scan of the lung bases shows cavitary lesions. What is the most likely diagnosis?
What is the most reliable sign of injury to the intrathoracic aorta?
In X-ray, loops of bowel are seen on the left side of the hemithorax with a shift of the heart shadow. What is the likely diagnosis?
Unilateral elevation of the diaphragm is commonly due to which of the following?
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
