Chest Radiology — MCQs

On this page
Superior rib notching is seen in all except?
A soft tissue mass in the chest with rib erosion in X-ray is seen in all except?
A boot-shaped heart on a chest X-ray is characteristic of which congenital heart defect?
A 60-year-old man with a 40-pack-year smoking history and 20 years of work as a construction worker presents with shortness of breath and occasional blood-streaked sputum. His ECG shows lateral wall ischemia. What is the likely cause of the findings on his chest x-ray?
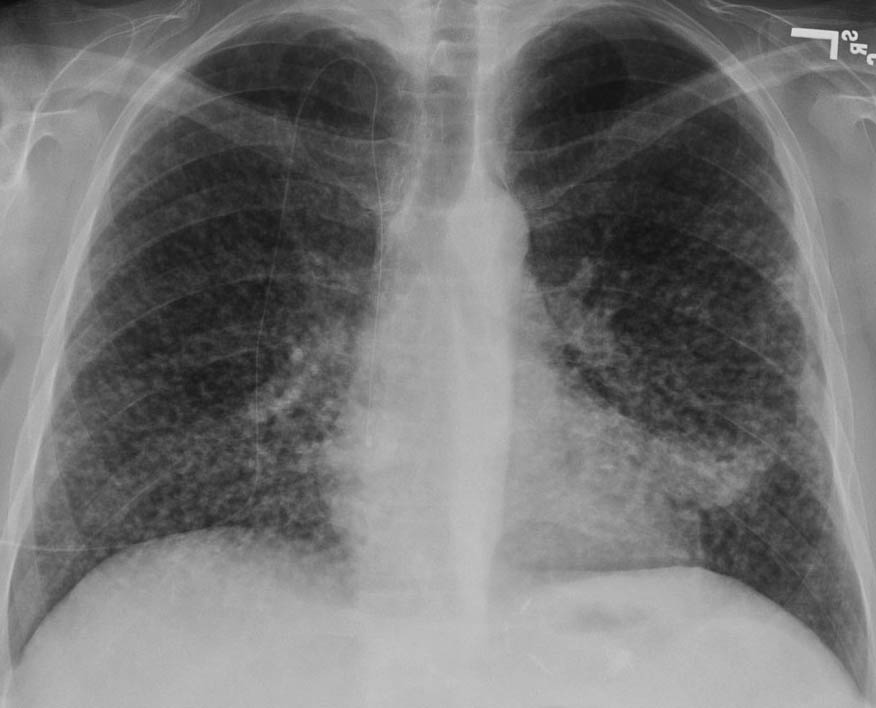
In a lung X-ray, what causes a heterogenous shadow?
What does a CT of the Thorax primarily represent?
Which of the following is NOT a chest X-ray sign of pulmonary embolism?
The "sniff test" is used to assess for which of the following conditions?
Deep sulcus sign is seen in which of the following conditions?
Popcorn calcification on chest X-ray is seen in:
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
