Chest Radiology — MCQs

On this page
The CT chest shows presence of:
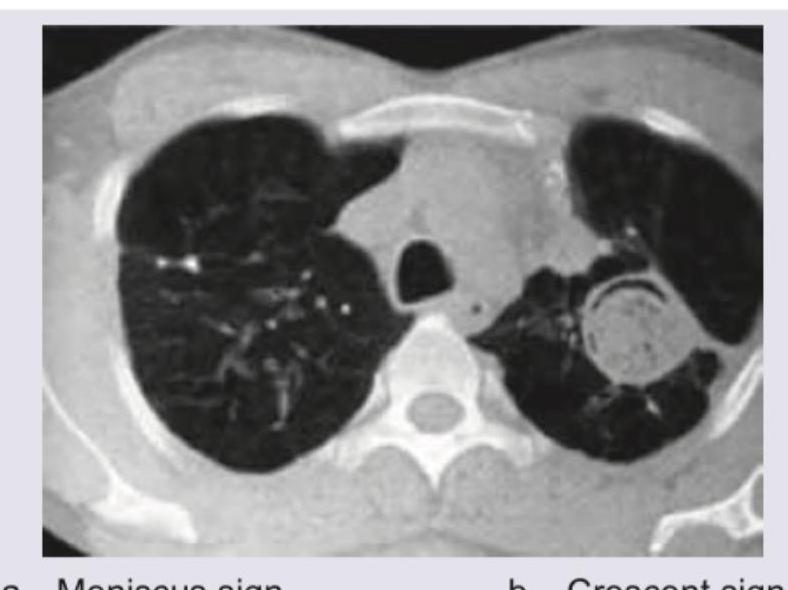
A 4-year-old child with high grade fever with chills and rigors for past 4 days and fast breathing is brought to the hospital. On examination subcostal recession and nasal flaring is noted. Since patient is already on antibiotics for past 3 days from another hospital a Chest X-ray and CT Chest was ordered. The diagnosis is:
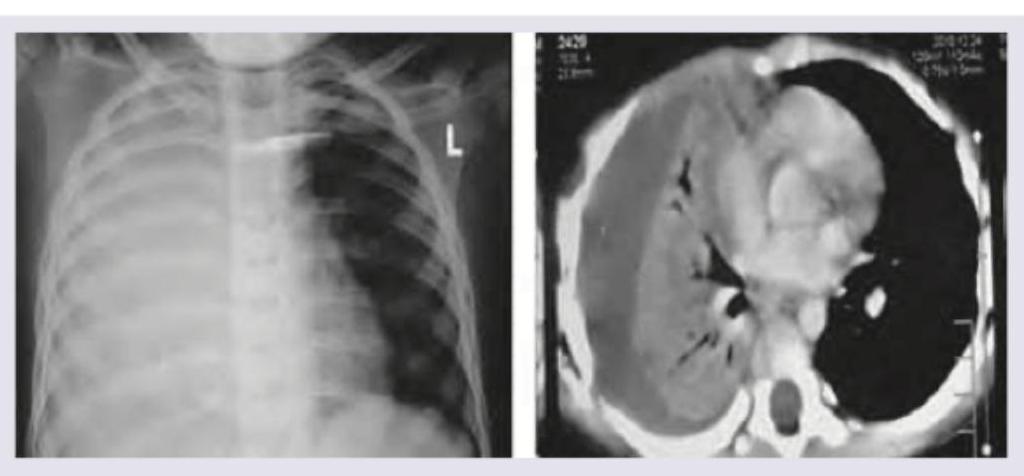
The chest X-ray of a cystic fibrosis patient shows presence of:
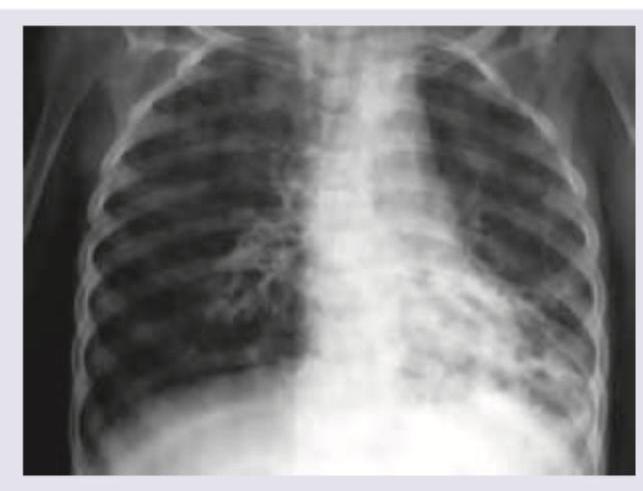
An axial HRCT of the chest is shown. The image demonstrates small peripheral branching opacities due to mucoid impaction of contiguous branching bronchioles. What is the most likely diagnosis?
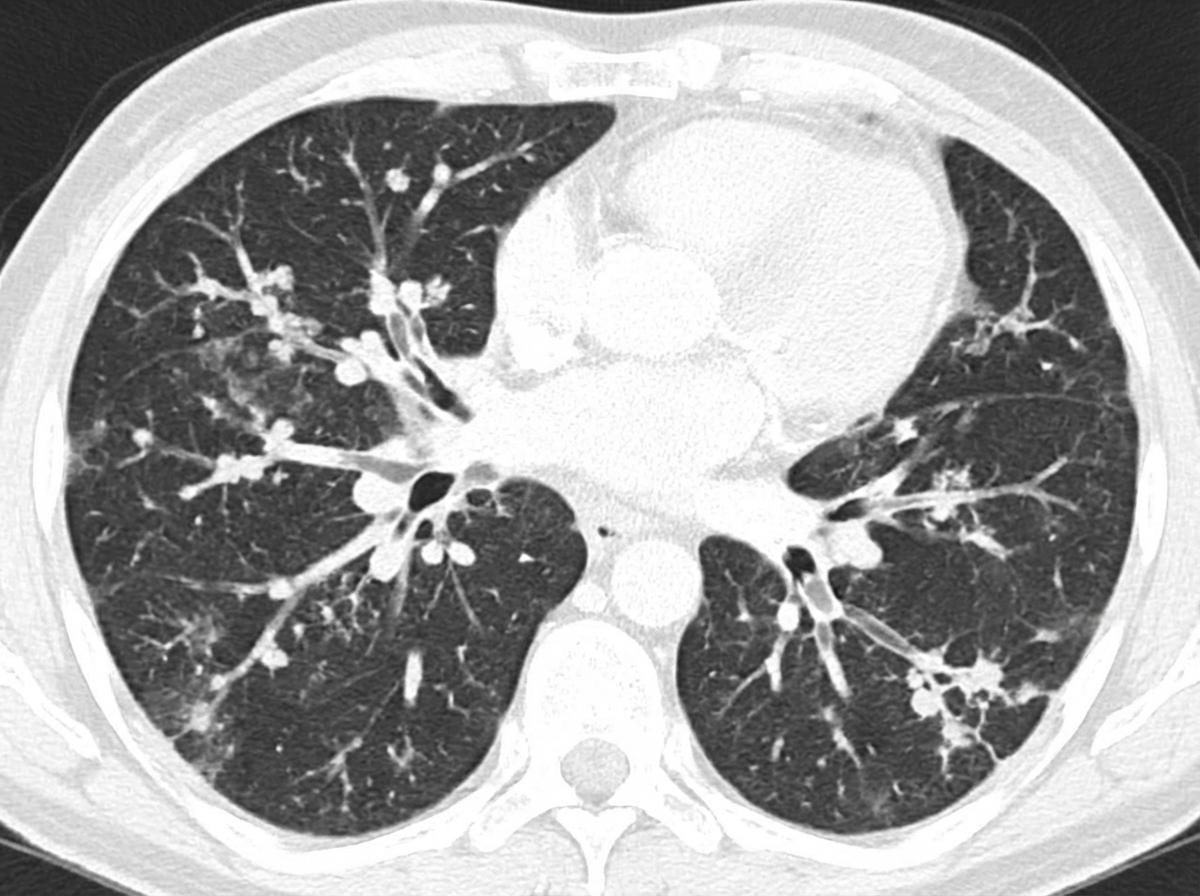
The CT chest image shows large bullae in bilateral lung fields. This is diagnostic of which condition?
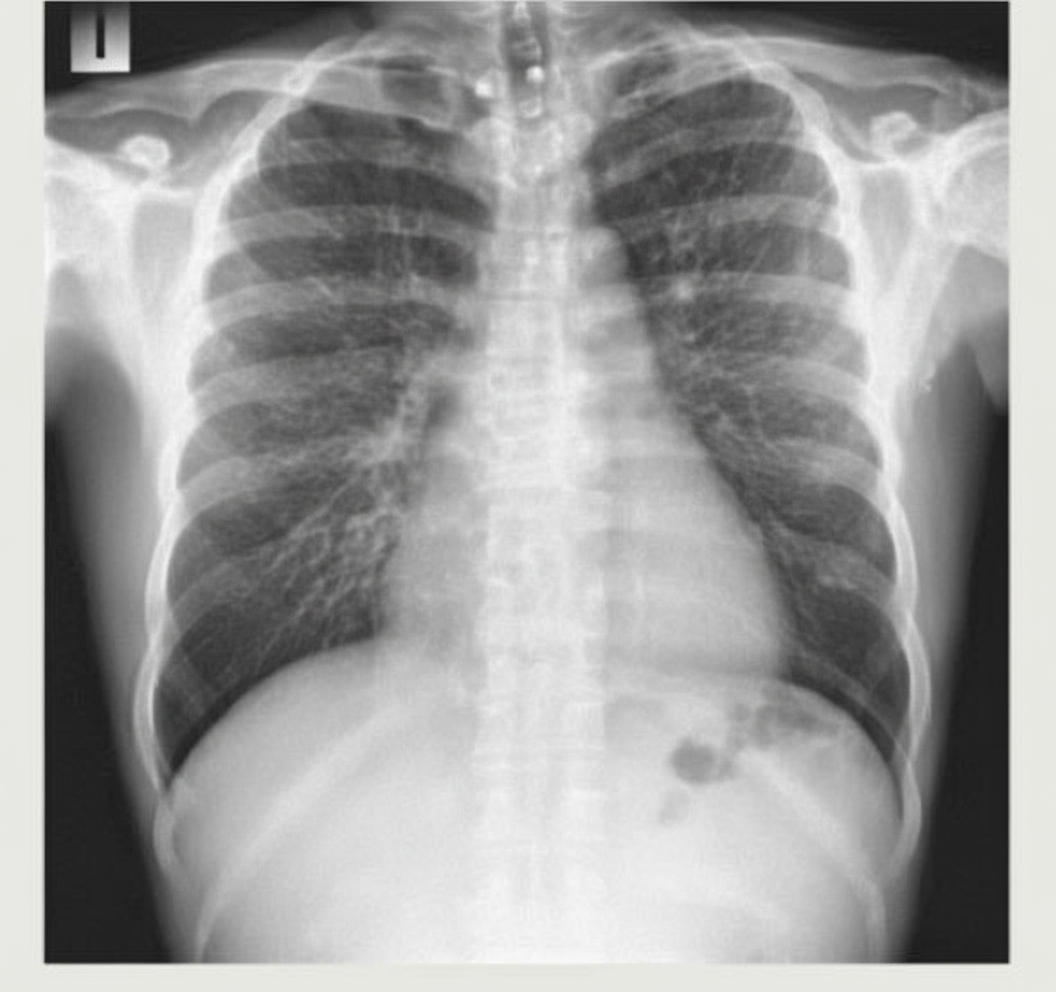
A chest X-ray shows bilateral reticular nodular shadows in both lung fields. The diaphragm is not flattened and the cardiothoracic ratio appears normal. What is the most likely pattern seen?
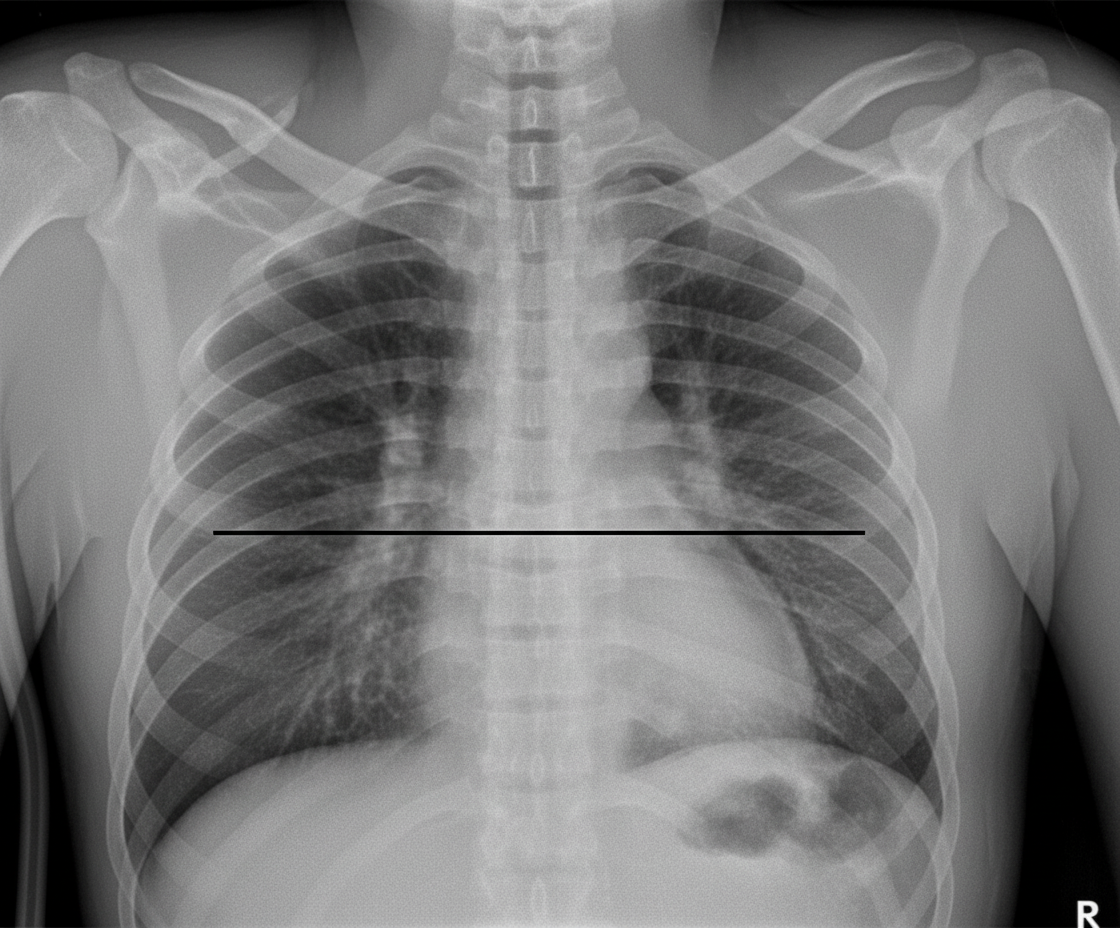
The image shows a standing upright chest X-ray with pleural reflection and a straight horizontal air-fluid level with absence of meniscus sign. What is the most likely diagnosis?
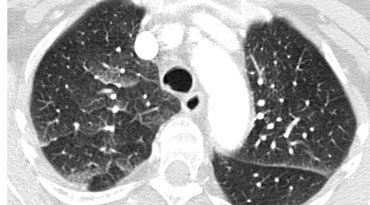
The CT chest image shows a hazy increased attenuation with preserved bronchial and vascular markings. What pattern is demonstrated?
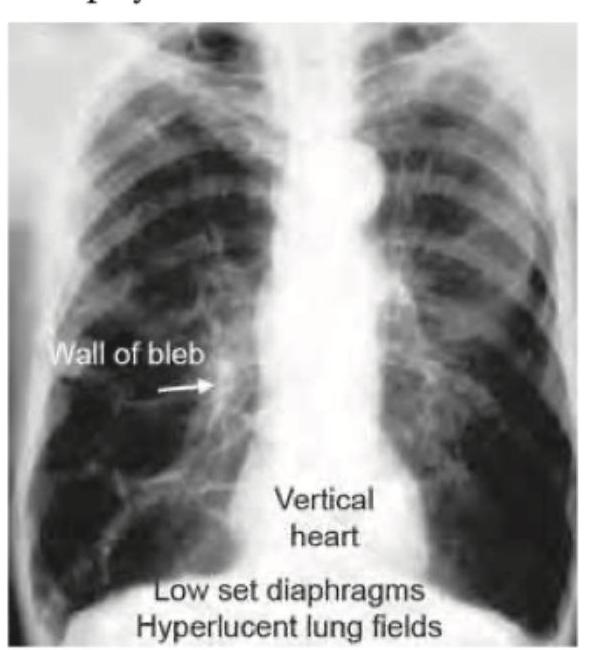
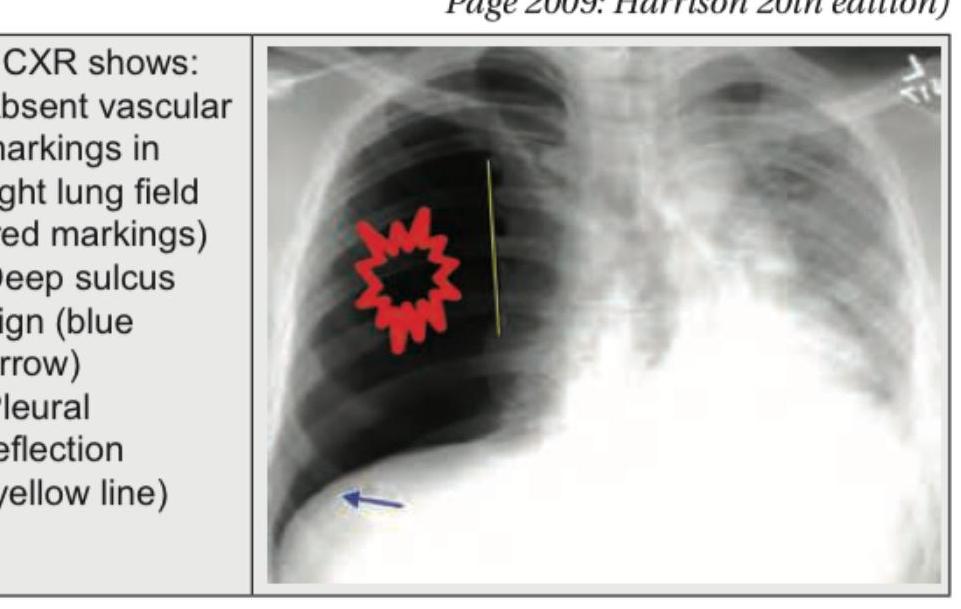
A 45-year-old male presents with sudden onset shortness of breath and chest pain. A chest X-ray is obtained. What is the most likely diagnosis based on the image?
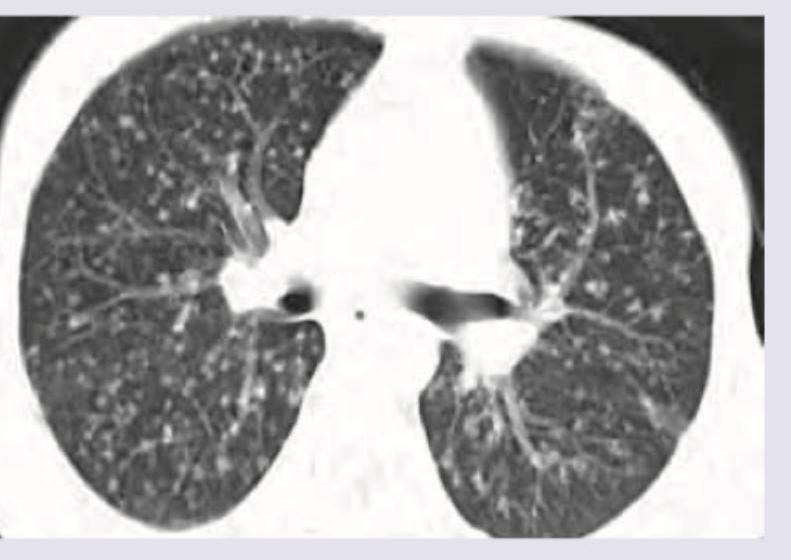
The following pattern in CT scan shown below can occur due to spread from:
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
