Chest Radiology — MCQs

On this page
What is the investigation of choice for a solitary pulmonary nodule?
A chest X-ray of an industrial worker with 20 years of asbestos exposure shows a diffuse appearance of the lower lobe with a 'comet tail' infarct on a PA view. What is the most likely diagnosis?
What findings are shown on the chest X-ray of the patient?
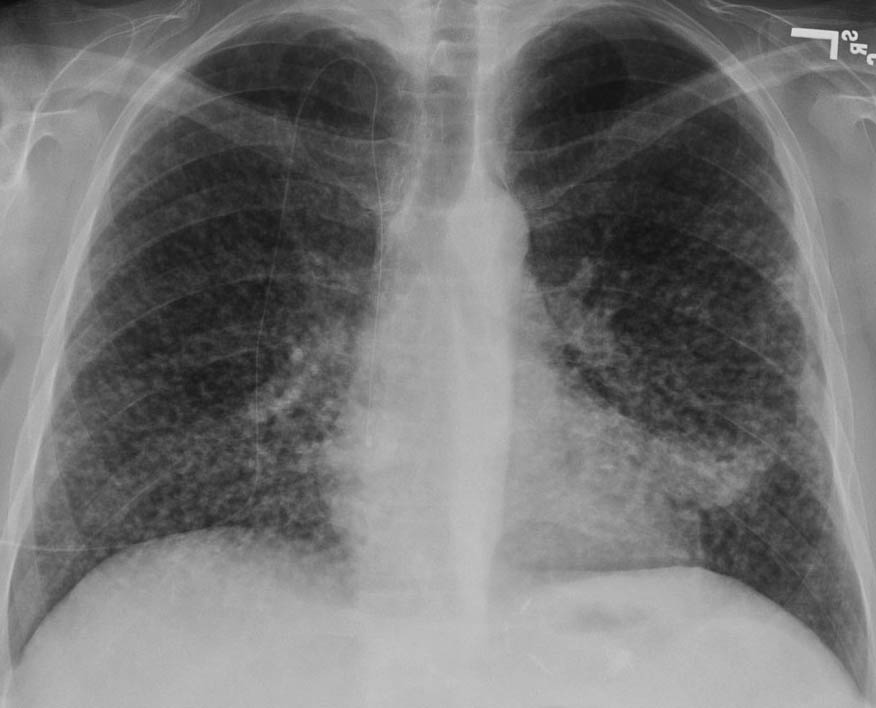
Obscuration of the left heart border is suggestive of which of the following conditions?
Millet seed like pattern is seen in which of the following conditions?
The "water lily sign" on a chest X-ray is characteristic of which condition?
Pulmonary embolism is best diagnosed by which imaging modality?
Which of the following statements regarding signs of pulmonary embolism are TRUE or FALSE?
Potato nodes are a characteristic feature of which of the following conditions?
Which of the following statements is false regarding the role of chest radiography in a patient presenting with acute abdomen?
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
