Chest Radiology — MCQs

On this page
What is the best investigation when there is clinical suspicion of pulmonary embolism?
On barium swallow, which of the following causes a posterior impression?
Unilateral hyperlucent hemithorax on chest X-ray is seen in which condition?
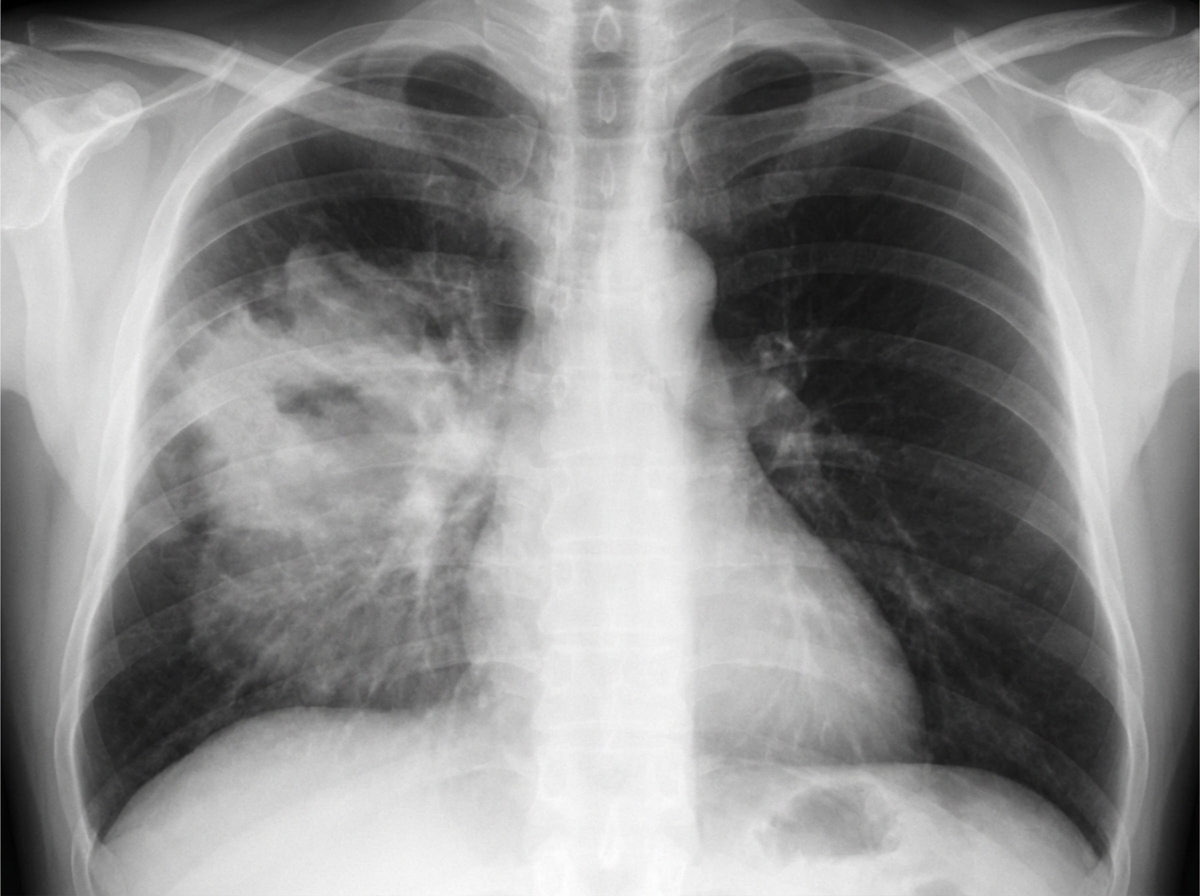
A 44-year-old man presents with dyspnea, cough, and mild pyrexia. Which lobe of the lung is most likely involved?
Which of the following is FALSE about Kerley's A lines?
A 75-year-old lady with severe chronic obstructive pulmonary disease (COPD) presents with acute breathlessness. The chest X-ray shows no focal consolidation. She is afebrile, but D-dimers are markedly elevated. Which of the following is the best investigation to diagnose this condition?
The 'tree in bud' sign on HRCT is suggestive of which condition?
What is the investigation of choice for pulmonary embolism?
What is the most common lesion found in the middle mediastinum?
What is the best radiographic view for demonstrating an interlobar pleural effusion?
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
