Chest Radiology — MCQs

On this page
A 35-year-old patient with a history of asbestos exposure presents with chest pain. An X-ray reveals a solitary pulmonary nodule in the right lower zone. A CECT shows an enhancing nodule adjoining the right lower costal pleura with a comet tail sign and adjacent pleural thickening. What is the most likely diagnosis?
Water bottle heart is seen in which of the following conditions?
The "floating water-lily sign" is characteristic of which condition?
Westermark's sign, Hampton's hump, and Palla's sign are all characteristic radiological findings suggestive of which condition?
Lucent hemithorax is due to all the following except?
Which of the following is NOT a radiological feature of chronic cor pulmonale?
Bronchography may be dangerous in a patient with which of the following conditions?
What is not a CT finding in bronchiectasis?
A 42-year-old female smoker with a 20-pack-year history is admitted with progressive shortness of breath. On examination, she has distant heart sounds with decreased breath sounds on lung exam bilaterally. No summation gallop is heard. ECG shows low voltage. Chest x-ray findings are shown. Which of the following findings on the chest x-ray may be associated with this presentation?
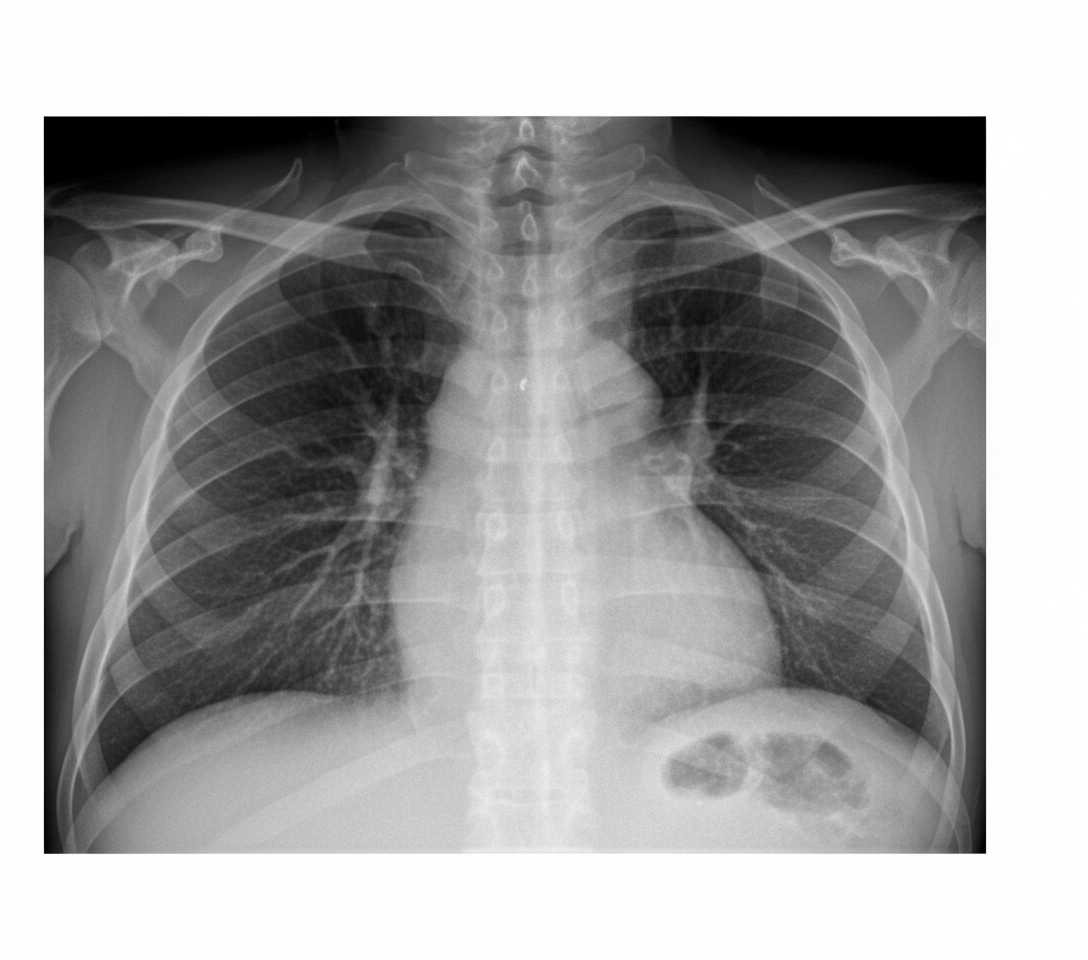
The CT chest of the patient shows the presence of which of the following?
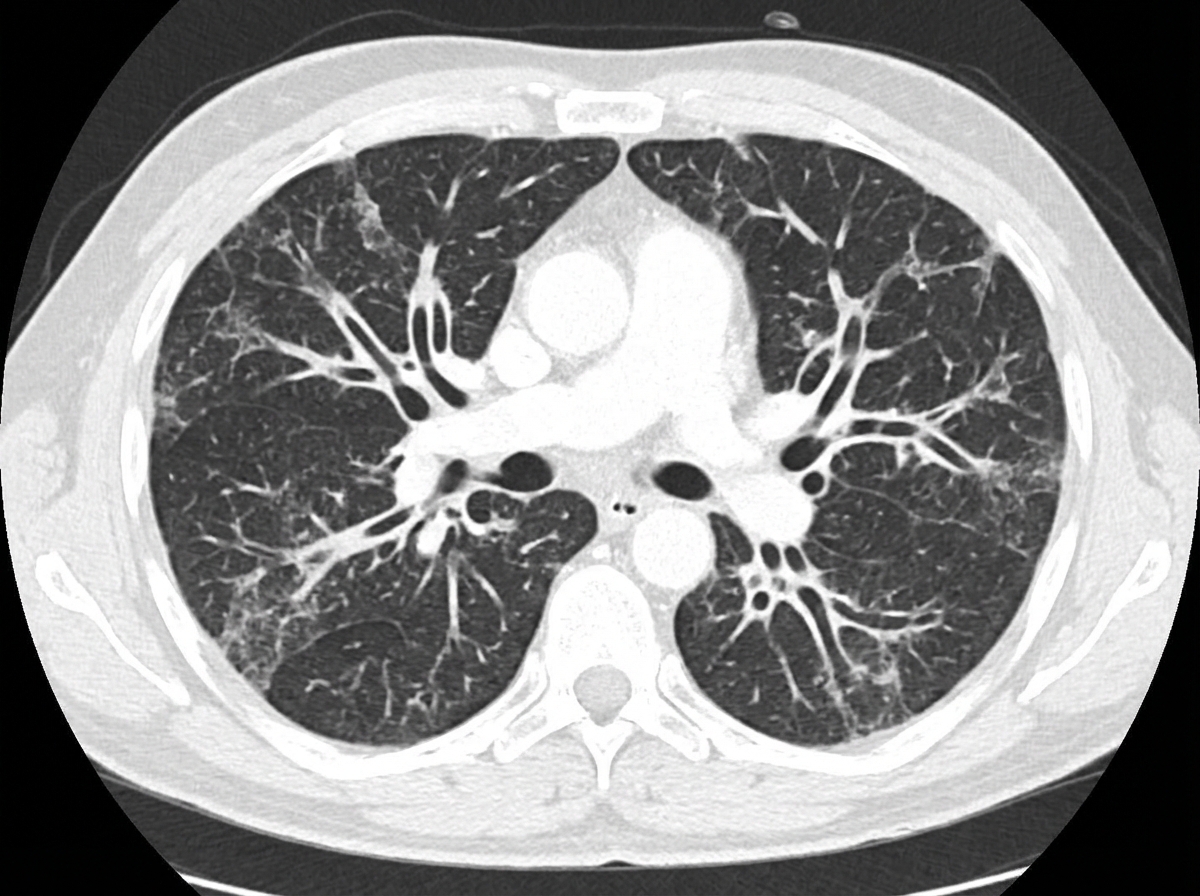
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
