Chest Radiology — MCQs

On this page
Which of the following is NOT an X-ray finding of Staphylococcus pneumonia?
A chest X-ray of a patient reveals hyperlucency of the right lung. What is the probable diagnosis?
All of the following show a miliary shadow on chest X-ray except?
A 40-year-old male presented to the OPD with fever and breathlessness. His X-ray is shown below. What is the most probable diagnosis?
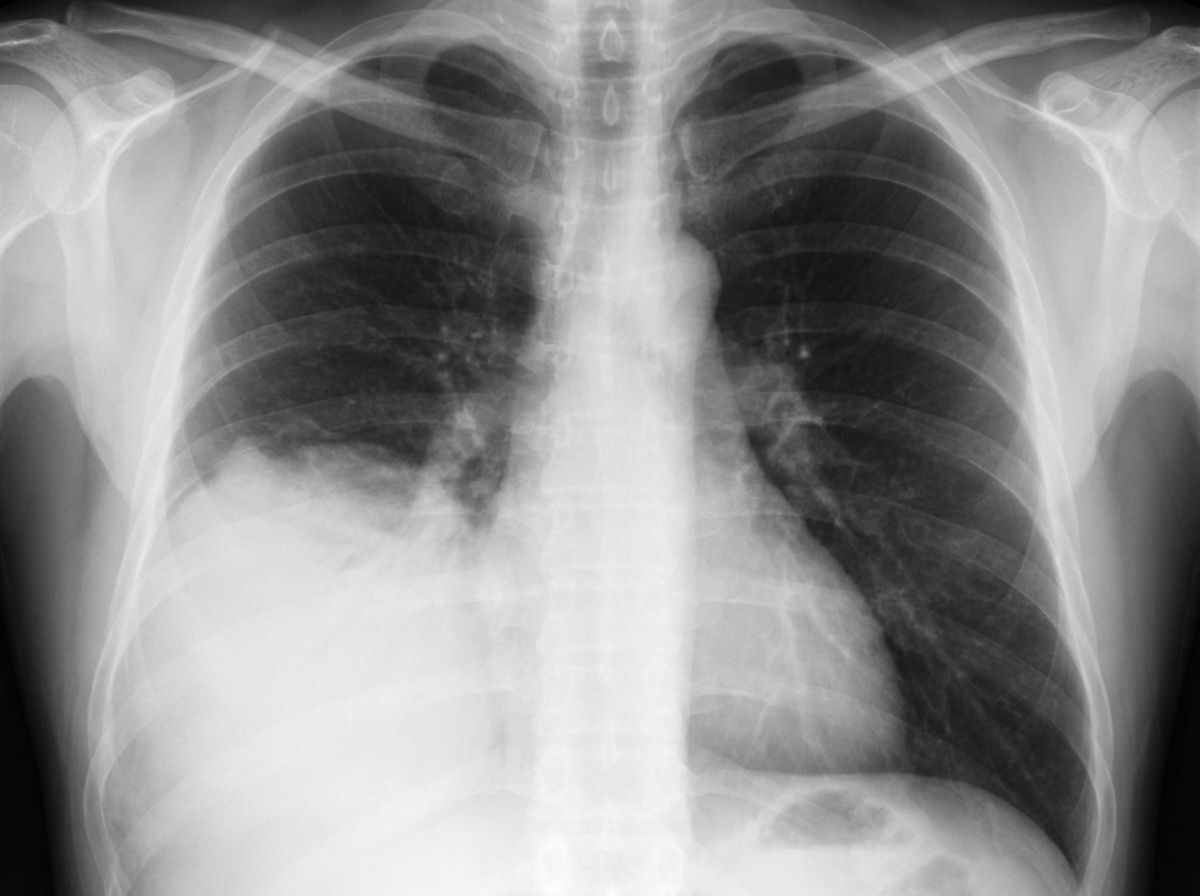
A patient presents with a solitary pulmonary nodule on chest x-ray. What is the most appropriate investigation to establish a diagnosis?
Kerley B lines are seen in which of the following conditions?
In pulmonary embolism, what are the characteristic findings on a perfusion scan?
A 35-year-old chronic smoker (10 years) presents to the emergency room 3 hours after an accident with signs of blood loss. The patient was transfused with a fixed component ratio of the same blood group. Four hours post-transfusion, the patient developed breathlessness and cough. A chest X-ray was advised. What is the most common blood component transfusion that leads to this condition?
Miliary shadows on chest X-ray are typically seen in which of the following conditions?
What is a Phantom Tumor?
Practice by Chapter
Normal Chest Radiographic Anatomy
Practice Questions
Radiographic Signs in Chest Imaging
Practice Questions
Pulmonary Infections
Practice Questions
Chronic Obstructive Pulmonary Disease
Practice Questions
Interstitial Lung Diseases
Practice Questions
Pulmonary Neoplasms
Practice Questions
Pleural Diseases
Practice Questions
Mediastinal Pathology
Practice Questions
Congenital and Developmental Chest Anomalies
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Chest Trauma Imaging
Practice Questions
Post-Surgical Chest Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
