Chest Trauma Imaging — MCQs

Thoracotomy is indicated in all the following conditions except:
Which of the following injuries is the most serious?
The imaging modality primarily used in FAST (Focused Assessment with Sonography for Trauma) exam is:
All of the following are true regarding flail chest, EXCEPT:
A 60-year-old woman presents with a history of smoking and cough. Chest X-ray shows a solitary pulmonary nodule. Which of the following is the most appropriate next step in management?
Identify the most likely diagnosis based on the chest X-ray findings in a patient with low-grade fever.
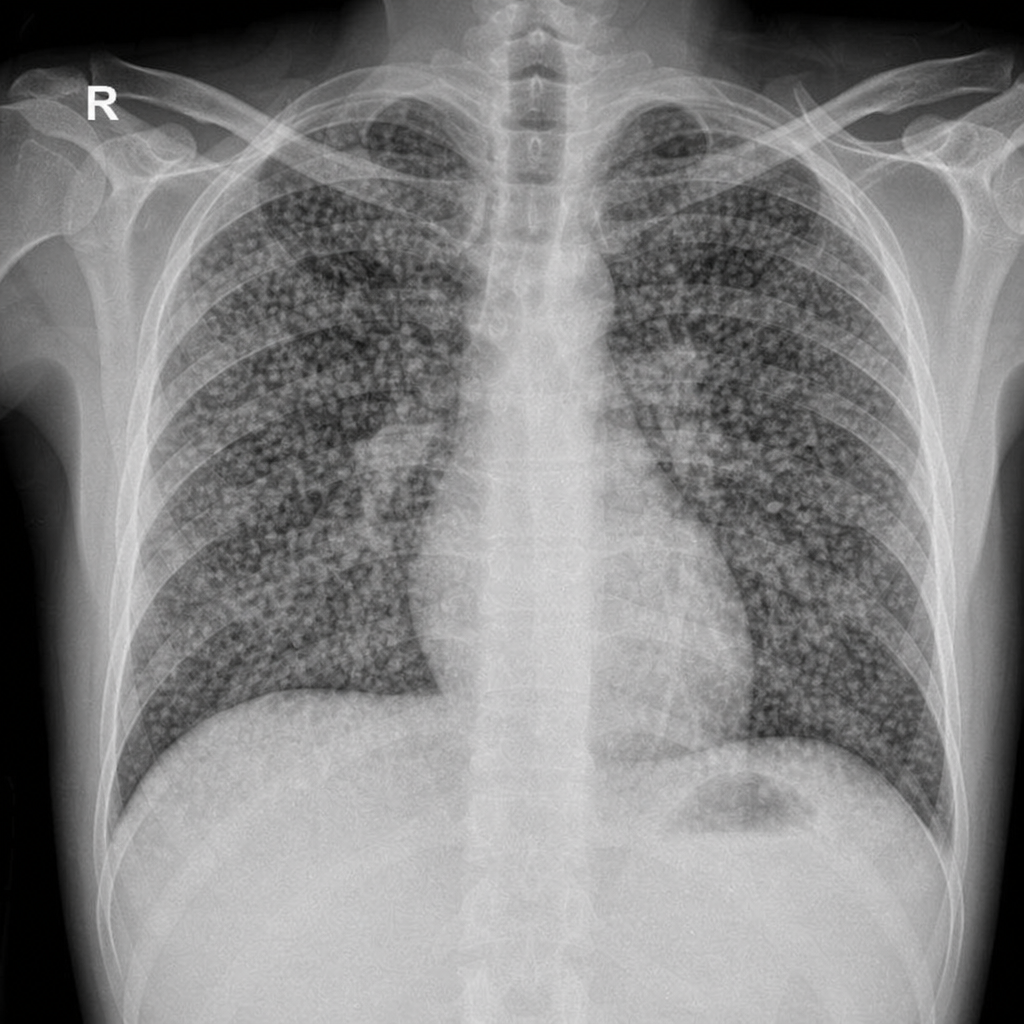
The following are direct signs of lung collapse seen on a chest X-ray, which one of the following is NOT a direct sign?
A patient after a heavy meal comes with epigastric pain. On examination, there is tenderness and rigidity in the upper abdomen. An X-ray shows pneumomediastinum. What could be the cause?
Most common type of shock in emergency room is
An incised-looking laceration is seen in all except:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
