Cardiovascular Radiology — MCQs

On this page
Notching of ribs is characteristic of which condition?
In which aspect is transesophageal echocardiography superior to transthoracic echocardiography?
String sign in angiography is suggestive of which condition?
A 69-year-old male, a heavy smoker (60 cigarettes/day for 40 years), presented with a 12-hour episode of slurred speech that resolved. He had a single episode of haemoptysis 4 weeks prior and has known lung cancer with brain metastases. An ECG revealed new atrial fibrillation, and all blood tests, including cardiac biomarkers, were normal. A chest CT was performed. Based on the clinical presentation and CT findings, which of the following is the most probable diagnosis?
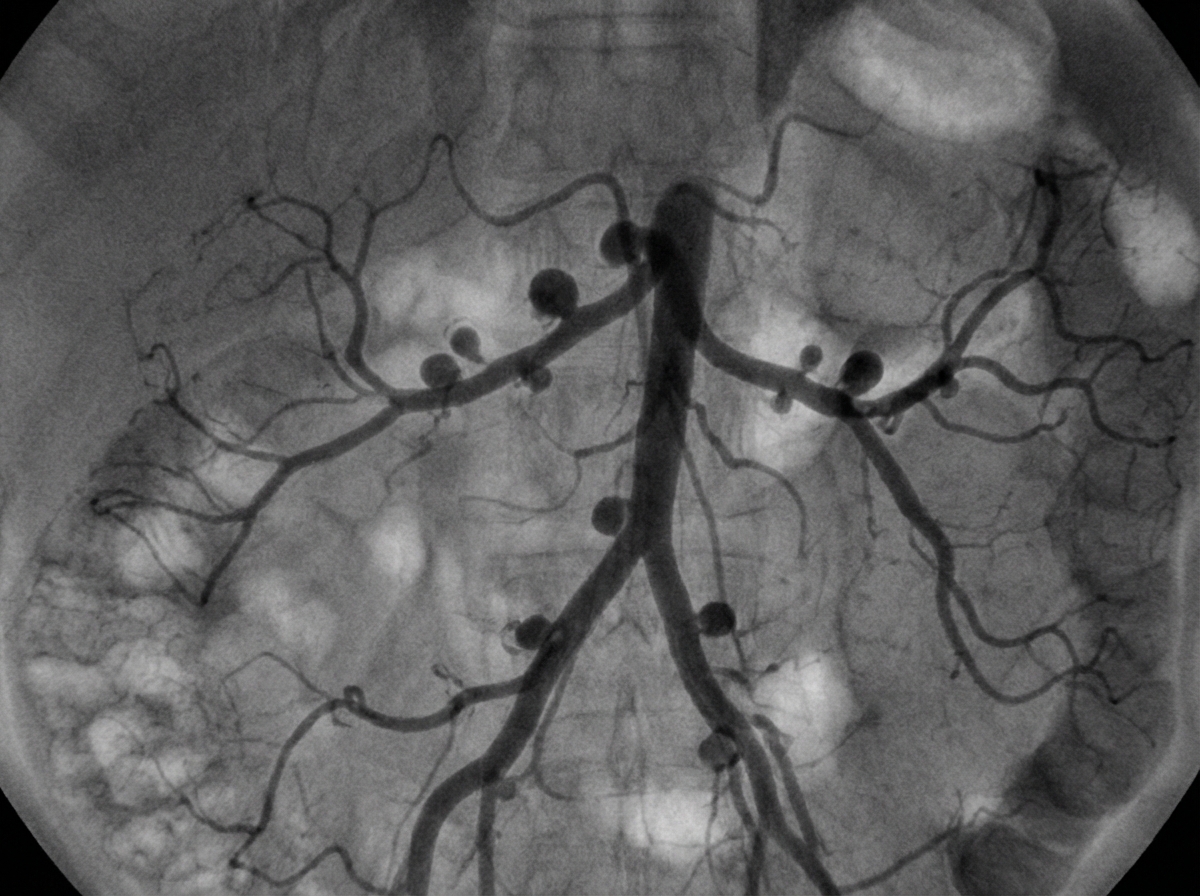
Which condition is most likely associated with the following angiography findings?
The cardiac silhouette can have an "egg on side" appearance in which of the following conditions?
What is the most important sign of significance of renal artery stenosis on an angiogram?
Bilateral rib notching is seen in which of the following conditions?
What is the best investigation for pericardial effusion?
What is the characteristic X-ray finding in Atrial Septal Defect (ASD)?
Practice by Chapter
Cardiovascular Anatomy
Practice Questions
Cardiac CT Techniques
Practice Questions
Cardiac MRI Techniques
Practice Questions
Ischemic Heart Disease Imaging
Practice Questions
Valvular Heart Disease
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease
Practice Questions
Aortic and Great Vessel Imaging
Practice Questions
Peripheral Vascular Imaging
Practice Questions
Cardiovascular Interventional Procedures
Practice Questions
Post-Surgical Cardiovascular Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
