Cardiovascular Radiology — MCQs

On this page
Which of the following chemicals or isotopes is used in cardiac ventriculography?
A 63-year-old patient with a history of tachyarrhythmias is on an implantable cardioverter-defibrillator (ICD). The patient suddenly develops shock. Which of the following is the best investigation to assess the position and integrity of the ICD?
A 24-year-old woman presents with mildly painful swelling of her right leg and acute shortness of breath. She is 32 weeks pregnant with her second child and has no other medical history. Which of the following statements is NOT true regarding this condition?
In which of the following conditions is an increased cardiac silhouette NOT seen, except?
Rib notching is a feature of which congenital heart anomaly?
What is the characteristic radiographic appearance of aoitis?
Which of the following statements is FALSE regarding Coarctation of the Aorta?
What is the investigation of choice to confirm hemochromatosis as the cause of cardiomyopathy?
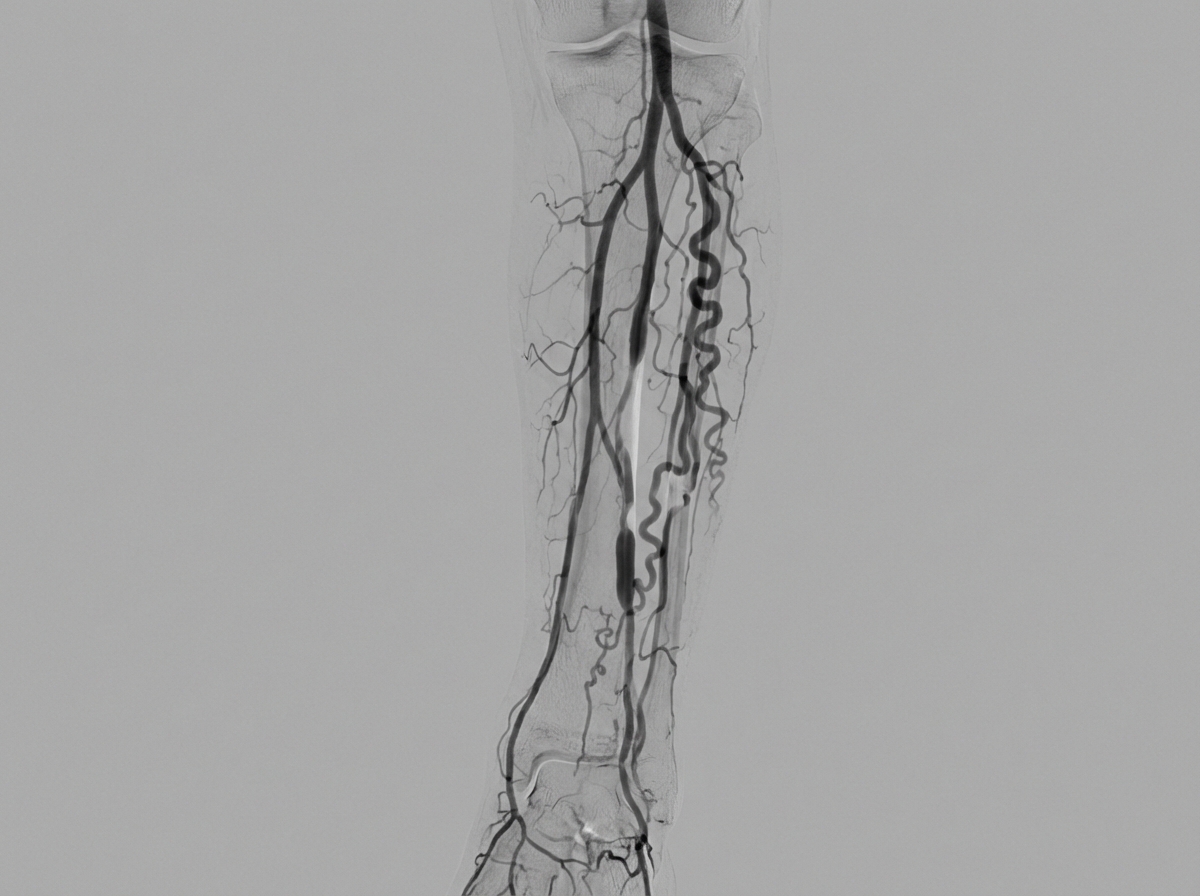
A digital subtraction angiography of a 35-year-old smoker is shown. What is the possible diagnosis?
What is the best initial investigation for a suspected case of Dysphagia lusoria?
Practice by Chapter
Cardiovascular Anatomy
Practice Questions
Cardiac CT Techniques
Practice Questions
Cardiac MRI Techniques
Practice Questions
Ischemic Heart Disease Imaging
Practice Questions
Valvular Heart Disease
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease
Practice Questions
Aortic and Great Vessel Imaging
Practice Questions
Peripheral Vascular Imaging
Practice Questions
Cardiovascular Interventional Procedures
Practice Questions
Post-Surgical Cardiovascular Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
